Looking forward
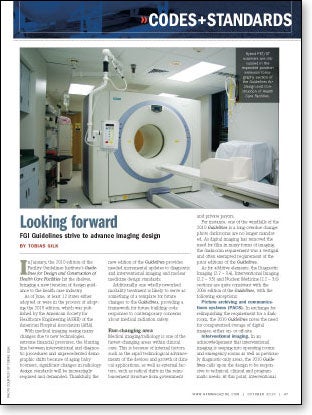
In January, the 2010 edition of the Facility Guidelines Institute's Guidelines for Design and Construction of Health Care Facilities hit the shelves, bringing a new iteration of design guidance to the health care industry.
As of June, at least 12 states either adopted or were in the process of adopting the 2010 edition, which was published by the American Society for Healthcare Engineering (ASHE) of the American Hospital Association (AHA).
With medical imaging seeing many changes due to new technologies, extreme financial pressures, the blurring line between interventional and diagnostic procedures and unprecedented demographic shifts because of aging baby boomers, significant changes in radiology design standards will be increasingly required and demanded. Thankfully, the new edition of the Guidelines provides needed incremental updates to diagnostic and interventional imaging and nuclear medicine design standards.
Additionally, one wholly reworked modality treatment is likely to serve as something of a template for future changes to the Guidelines, providing a framework for future building code responses to contemporary concerns about medical radiation safety.
Fast-changing area
Medical imaging/radiology is one of the fastest-changing areas within clinical care. This is because of internal factors, such as the rapid technological advancements of the devices and growth of clinical applications, as well as external factors, such as radical shifts in the reimbursement structure from government and private payors.
For instance, one of the windfalls of the 2010 Guidelines is a long-overdue change: photo darkrooms are no longer mandated. As digital imaging has removed the need for film in many forms of imaging, the darkroom requirement was a vestigial and often exempted requirement of the prior editions of the Guidelines.
As for additive elements, the Diagnostic Imaging (2.2 – 3.4), Interventional Imaging (2.2 – 3.5) and Nuclear Medicine (2.2 – 3.6) sections are quite consistent with the 2006 edition of the Guidelines, with the following exceptions:
Picture archiving and communications systems (PACS). In exchange for relinquishing the requirement for a darkroom, the 2010 Guidelines notes the need for computerized storage of digital images, either on- or off-site.
Interventional imaging. In an acknowledgement that interventional imaging is seeping into operating rooms and emergency rooms as well as previously diagnostic-only areas, the 2010 Guidelines calls upon the design to be responsive to technical, clinical and programmatic needs. At this point, interventional imaging is still amorphous with regard to its location, patients, acuity and even its immediate physician supervisors. Consequently, there are no prescriptive requirements for interventional imaging.
Positron emission tomography (PET). The new PET section has expanded beyond its generic placeholder from the 2006 edition. The section also describes the newer, more common form that contemporary clinical PET has taken, namely the hybrid scanner — PET coupled with computed tomography (CT).
While the 2010 Guidelines debatably states that a PET/CT scanner requires no more space than a PET, it does add programmatically critical holding areas and uptake (though the uptake room description appears to be a mash-up of an uptake room and a "hot" toilet room, which are often provided as separate rooms).
The PET section also expanded its siting description of a cyclotron room in the unlikely event that the facility generates its own radiopharmaceuticals. With post-9-11 Nuclear Regulatory Commission clampdowns on medical isotope security, in-house generation of nuclear material has become very regulatory intense.
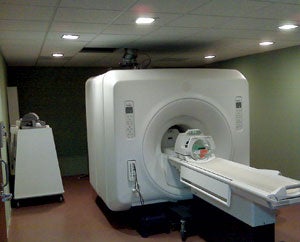 |
| The 2010 edition of the Guidelines for Design and Construction of Health Care Facilities seeks to incorporate physical safety standards for MRI where state and federal authorities have not. |
Magnetic resonance imaging (MRI). In contrast to the incremental changes elsewhere in imaging, far and away the largest change to modality design guidance in the 2010 Guidelines is for MRI. There was virtually no design guidance in the 2006 edition, apart from indicating that individual rooms within the MRI suite (control, patient holding and computer room) and critical infrastructures (power conditioning and magnetic shielding) were to be provided. The 2010 edition of the Guidelines seeks to incorporate physical safety standards for MRI units where state and federal authorities or accreditation have not.
The most profound change to MRI design standards in the 2010 Guidelines is the directive referencing the American College of Radiology's (ACR's) four-zone screening and access control protocols for suite design as published in the
"ACR Guidance Document for Safe MR Practices: 2007" Among these layout principles from the ACR document are the following required program and space provisions:
a. Patient interviews and clinical screening;
b. Physical screening and changing areas (as indicated);
c. Siting of ferromagnetic detection systems;
d. Access controls; and
e. Accommodation of site-specific clinical and operational requirements.
New to Guidelines requirements for MRI is the explicit requirement to protect against unscreened access to any area where the fringing magnetic field is equal to 5-gauss in strength. Also, the suite must be laid out so that the operators' console position has a view to the patient within the MRI scanner as well as line-of-sight to the MRI scanner room entrance.
A new section describes the unique mechanical design requirements for safe enclosure around superconducting MRI equipment and the large volumes of cryogenic liquid that are typically present. These elements include the standard cryogen exhaust (quench) pipe, an emergency exhaust fan and an overpressure-relief mechanism.
The Guidelines now explicitly describe accommodations that must be made for specialty radio-frequency shielding assemblies in walls, floors and ceiling. An extensive appendix entry describes the siting considerations for magnetic shielding, which may or may not be indicated for a given MRI installation.
Proscribed details include a floor structure to reduce vibration, knock-out panels or roof hatches for MRI system delivery and an illuminated "the magnet is on" warning sign. Finish materials inside the MRI scanner room should be selected to minimize maintenance or servicing (a significant safety consideration, given the strength of the magnets in contemporary MRI scanners) and should anticipate growth in interventional image-guided applications.
Critical magnetic field equipment tolerances should be marked on the finishes to ensure the safe use of clinical support equipment such as ventilators or medication pumps. Similarly, the extent of the 5-gauss magnetic field limits (sometimes referred to as the "pacemaker line") should also be site-marked for the safety of unscreened individuals.
The extent of the MRI suite design requirement changes are such that the only element unchanged from the prior edition of the Guidelines is the criteria to have a hand-washing station near, but not necessarily within, the scanning room.
In a separate section (2.2 – 3.3.2.6), the 2010 edition broaches the subject of intra-operative imaging with a short narrative stating that intra-operative MRI suites should conform with both the requirements for operating rooms and those identified in the diagnostic imaging section. It is presumed that similar mutual standards would apply to the variety of intra-operative (or co-located with surgery) imaging modalities used today, including CT as well as radiography and fluoroscopy.
Future design guidance
Within the health care design standards community, it has been acknowledged that all of imaging and nuclear medicine would benefit from the sort of rewrite and expansion provided in the MRI section of the 2010 edition of the Guidelines.
This acknowledgement began in whispers last year, when preliminary drafts of the 2010 edition were circulated for public comment. Since then, medical imaging safety has been the subject of intense examination on Capitol Hill and within the Food and Drug Administration (FDA). This contemporary attention only strengthens the desire for more comprehensive radiology design standards.
While much of the current concern about radiology safety is focused on the actual exam itself, it is expected that the attention also will enhance design considerations of equipment suites in light of the equipment, staffing and financial realities facing clinical providers.
The development of future design standards by modality will further differentiate the raw technical siting considerations in vendor prototypical plans from operational and safety requirements that are the domain of vendor-neutral codes and standards. Still, future iterations of the Guidelines' imaging sections will likely not go as far as the Department of Veterans Affairs' (VA) Imaging Series Design Guides (www.cfm.va.gov/til/dGuide.asp), which provide integrated technical, safety and operational guidance, sprinkled with VA standards.
While it is premature to speculate what future Guidelines will contain for diagnostic and interventional imaging and nuclear medicine, it is highly likely that the level of guidance provided in future editions will more closely resemble the 2010 standards for MRI, addressing safety and operational concerns rather than the purely prescriptive square footage requirements that were the historical foundations of these sections.
Tobias Gilk is president of Mednovus Inc., Leucadia, Calif., and senior vice president of RADIOLOGY-Planning, Kansas City, Mo. He has served on the Facility Guidelines Institute's 2010 Guidelines Patient Safety Working Group. His e-mail is Tobias.Gilk@Mednovus.com or TGilk@RAD-Planning.com.
| Sidebar - FGI keeps to its mission |
|
To create a more formal document-writing process and to keep the Guidelines for Design and Construction of Health Care Facilities current, the Facility Guidelines Institute (FGI) was founded in 1998 as an independent, not-for-profit 501(c)(3) corporation. The primary objectives of FGI are to see that the Guidelines are reviewed and revised on a regular cycle using a consensus process carried out by a multidisciplinary group of experts from the federal, state and private sectors; to stimulate research in support of evidence-based design and construction guidelines; and to reinvest FGI's share of the net revenue derived from the sale of Guidelines documents to support the next revision cycle and to fund research that will improve future editions of the Guidelines. FGI is primarily interested in consensus methodology and in overseeing the Guidelines revision process. Specifically, FGI wants to make sure the Health Guidelines Revision Committee is properly funded; operates under a formal set of bylaws; has a balance of stakeholder representation from individuals with expertise or jurisdiction; uses the consensus process; requests public input in the form of proposals for change and comments on proposed changes; and reviews and revises the Guidelines on a timely basis to maintain a balance between minimum standards and the state of the art in health care design and construction practices. |




