HVAC selection for health care facilities
Hospital HVAC system designs present unique challenges to facility managers due to the sensitivities of the hospital environment. The selection process is not straightforward, because in health care facilities there is an increased level of demand, a variety of required thermal conditions, and codes regarding reliability and hygiene. On top of that is increasing pressure to reduce energy consumption while maintaining a safe environment.
No two hospitals are alike, and while the facilities often contain the same program, varying size, location, priorities or goals can lead to completely different HVAC systems. The goal, then, is not to designate a universal HVAC system for all health care facilities, but rather to identify the various factors and general processes that need to be considered when selecting HVAC systems for health care.
Identify project goals. The initial step in the HVAC selection process is to meet with the project stakeholders to fully understand the facility’s specific or desired goals. The engineer should document the client’s measurable expectations and define any critical success factors. Establish whether there are specific infection control risk assessment goals the facility might be seeking, such as a departmental reduction in airborne contamination or a reduction in the number of hospital-acquired infections. Identify any quantifiable sustainable and energy-efficiency goals to improve the building environment and provide cost savings for long-term building operations and maintenance, such as whether the project will seek any voluntary or mandatory certification programs like LEED or Green Globes. Also, identify whether there is an overall energy-use intensity target, or a percentage of energy-use reduction the project is seeking. All goals should be identified, grouped into “required” and “nice to have” categories, because some may not be feasible due to project constraints.
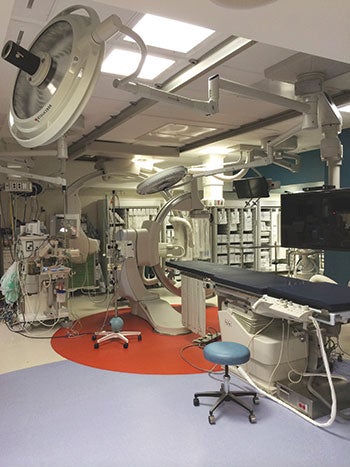 |
| PHOTO COURTESY OF RMF Engineering Recognize the specific pressurization requirements for the various medical programs within the building – isolation rooms, procedure rooms, waiting rooms – before selecting an HVAC system. |
Identify program requirements. Next, review the program requirements with the architect and medical staff. Discuss the temperature and humidity conditions for the various medical programs within the building, for example, in patient rooms, operating rooms, examination rooms and radiology — specifically whether any exceed the minimum requirements of ANSI/ASHRAE/ASHE Standard 170 — Ventilation of Health Care Facilities. Recognize the specific pressurization requirements for all the various medical programs, such as isolation rooms, procedure rooms, waiting rooms, kitchens and laboratories. Identify special filtration requirements of the medical programs — third-stage filtration, ultraviolet filtration, and bag-in bag-out infectious exhaust. Distinguish the specific ventilation requirements for each medical program, including minimum supply and outdoor air change rates. Discuss the need or desire for central facilitywide smoke control and the ability to provide pressurized compartments. Review the specific redundancy requirements for the project and consider hazard vulnerability analysis, including uninterruptible HVAC service above and beyond code minimum for all or part of the facility. Finally, identify the specific acoustic requirements for the various medical programs within the building.
Identify constraints. The engineer needs to fully understand the financial and physical constraints of the project and how they could limit the available HVAC system options or prevent the hospital from achieving any of its project goals. Prior to design, establish the allotted construction and mechanical costs for the project. The early programming and schematic phase of design can indicate the type and complexity of the budgeted HVAC system. Also, of greater importance, the mechanical costs may identify a disconnect between the HVAC scope and budget. Be sure to determine and understand the spatial limitations of the proposed or existing building. The size of the mechanical rooms, the method of vertical distribution, the floor-to-floor height, the desired architectural ceiling height and even the type of structure all will impact the HVAC design and may narrow the options.
Identify facility desires and expectations. It’s important to meet with the facility manager and associated staff to understand the needs, desires and expectations of those who will operate and maintain the HVAC system. Since the owners’ priorities do not always align with the priorities of individual departments, identify and resolve obvious disparities prior to design to satisfy all parties. Determine what is important to personnel in the HVAC design. Preferred equipment manufacturers, requirements for equipment accessibility, scheduled maintenance, historic reliability, controllability, system complexity, ability for measurement and verification, and system equipment size all can have an impact on the selection of the HVAC system.
Thermal and ventilation loads. Perform the cooling, heating and ventilation/air change loads for all of the individual program areas within the facility. Confirm the ambient outdoor design conditions based on the location of the facility, as well as the indoor temperature and humidity design conditions for each program or functional department. Integrate with the users, architect and other consultants to develop the optimal thermal resistance of the building envelope, building orientation, program occupancies, anticipated light and power loads, equipment loads, ventilation and infiltration/exfiltration. Developing accurate load calculations is an iterative design procedure that will have a direct impact on energy efficiency, occupant comfort, indoor air quality and building durability and, ultimately, will dictate the equipment selection. So, it is of significant importance that this process be performed correctly and that the results/outputs be fully understood.
Identify HVAC systems. Where possible (and initially based on the programmatic stacking diagrams), work with the design team to group the common program areas into functional departments with common HVAC requirements. Consider each functional department independently based on its differing HVAC needs, requirements and constraints. Through fact-gathering meetings and thermal and ventilation calculations, identify feasible HVAC systems that are appropriate for each functional department considering the project goals, requirements, constraints and expectations. It is likely that one specific system won’t satisfy all the criteria for each department, so all possible systems should be considered to determine which are most applicable and best suited for further evaluation. Several possible HVAC systems to consider as part of the analysis may include various configurations of the following options:
- Central air handling units (variable or constant air volume)
- Terminal heating and cooling systems (terminal reheat units, fan coil units, chilled beam units, radiant panels, water source heat pumps)
- Dedicated outdoor air systems
- Heating and ventilation systems
- Heat recovery systems/components (runaround system, fixed-plate system — air-to-air, heat pipes, heat wheel, enthalpy wheel)
- Exhaust systems (dry, wet, containment, infectious, kitchen hood)
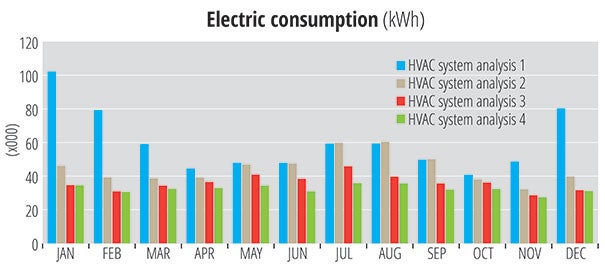 |
| Instead of focusing solely on upfront cost, perform a life-cycle cost analysis to narrow the list of HVAC options. |
Life-cycle cost analysis. Once the viable HVAC systems are determined for the facility, perform a life-cycle cost analysis (LCCA) on the selected systems, including factors such as first cost, annual energy usage, yearly maintenance, equipment lifespan and replacement costs to evaluate and quantify the performance of each system over a desired period (typically 30 years). At this stage, the information available is generally not detailed or fully developed; however, the results should represent fairly the estimated overall costs of the system alternatives for comparison, and identify the ideal system for an entire facility or systems for individual functional departments that will provide the lowest overall cost of ownership while achieving most or all of the project goals and expectations. Understand that the lowest resulting life-cycle cost may not necessarily be the ideal system, particularly if budget is not a high-ranking priority, and if the LCCA is simply another measurement to consider when developing the proposed system.
Owner review. After completing the LCCA and considering all the information gathered at this stage, the preliminary system that most satisfies the facility requirements can be selected. Depending on the functional departments within the facility, it is not uncommon for several different systems to be provided. It is important to present the design options from a performance and financial perspective to the project stakeholders for review, discussion and agreement. When possible, all process participants should be present and all parties should fully understand the results so that at the conclusion of the review, there is a clear agreement and a path forward regarding the HVAC systems to be designed.
There are many challenges related to selecting the proper health care HVAC system, and these challenges expand beyond those for a typical building. There is a direct connection among HVAC, patient outcomes and staff satisfaction, and while there is agreement that patient and staff safety are the first priority in health care design, beyond that the priorities differ. Design professionals must partner with stakeholders to study and identify the facility’s various needs, goals and objectives, so that a well-developed HVAC system can be designed to achieve the ultimate goal of improving patient care and maintaining health and wellness.
Craig Buck, PE, LEED AP, HFDP, is a mechanical engineer and associate at RMF Engineering with extensive experience in designing HVAC, plumbing and medical gas systems for health care facilities. For more information, email craig.buck@rmf.com.




