Testing for infection prevention
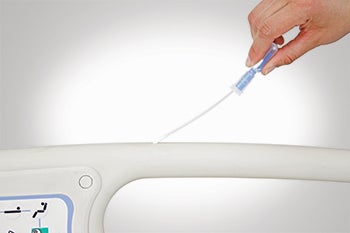 |
| Photo courtesy of Hygenia LLC It is important to validate the disinfection of high-touch surfaces that can become a source for transmission of pathogens. |
As the link between environmental transmission of germs and health care-associated infections (HAIs) has become clearer over the past several years, it has helped to build the bonds among environmental services (ES), infection prevention (IP) and nursing professionals who are fighting to keep patients safe.
By 2010, for instance, well-established studies had reported on the transmission of germs via the environment. Among them, the American Journal of Infection Control published an article titled “Evaluating hygienic cleaning in health care settings: What you do not know can harm your patients.”
You may also like |
| Using quality assurance monitoring |
| ES team thrives in complex environment |
| Cleaning ambulatory surgery centers |
| |
The Centers for Disease Control and Prevention (CDC) also published the “Options for Evaluating Environmental Cleaning” tookit that explains how to implement an objective ES monitoring program. It outlines the best surfaces to choose, how to partner for best performance and provides information about different types of environmental surface measurement devices.
The industry already had been following the CDC‘s 2008 Guideline for Disinfection and Sterilization in Healthcare Facilities, which warned of potential secondary transmissions, but these new documents made IP, ES and nursing leaders rethink how the environment can contribute to HAIs.
Validating competency
At Greenville, S.C.-based Bon Secours St. Francis Health System’s Downtown and Eastside hospitals, the ES team began looking for a method to objectively validate staff competency. Likewise, the organization’s IP team was looking for a way to to prevent HAIs from cross-transmission.
With 370 total beds, the two hospitals served high-risk patients requiring open heart surgery, neurosurgery, bone marrow transplantation, labor and delivery, or orthopedic surgery. When the ES team and IP professionals read the literature, they knew they needed to redouble their efforts. In a collaborative effort, both teams came together to reduce the risk for infection and thereby improve the well-being of the organization’s patient population.
To help in this endeavor, the ES team and IP professionals evaluated the pros and cons of the different adenosine triphosphate (ATP) bioluminescence monitors, looking for practicality and ease of use. ES purchased the first monitor and began random audits. ES employees were given immediate feedback, and results were used as a teaching tool, but the process was random. Results were not shared beyond the ES department.
Judging cleaning
The ATP system allowed the ES team to judge cleaning. No matter what the visual appearance of a horizontal or vertical surface throughout the hospital, ES staff could tell by swabbing and then testing the swab for 15 seconds whether the surface was clean. The team then started to do more swabs than first planned as they went from high-touch surfaces in patient rooms to departments, doctors’ lounges and public areas.
During monthly meetings with support services leadership, ES produced ATP results graphs showing current progress and areas for improvement. After a couple of months, the IP team wanted to talk about using the CDC cleaning evaluation toolkit as a way to validate cleaning effectiveness. The IP team was pleased that there were data available and that a process was already in place.
While the ATP results were first posted with the ES staff and the vice president of support services for review, ES and IP then enhanced the program by sharing results with more people. The IP professionals now attend ES meetings and other events. During ES Week, the IP team caters a meal for the ES team. As more ATP results started to come in and testing was being completed, weekly meetings with the IP team became a great way for ES staff to discuss any new articles or reports that could help to improve the success of the program.
As the ES team proceeded with testing and staff became more familiar with the process, they came up with a “Clean Team Challenge.” The idea behind this new program to enhance ATP testing was to separate employees into two teams that competed against each other by adding up the scores of the ATP results. The team with the lowest score won a gift. This friendly competition has been good for ES staff and, of course, for patients.
In November 2011, the IP team began using the CDC’s Excel validation tool for environmental disinfection. The ES supervisors shared their results with the IP team, which logged ATP results into the CDC spreadsheet under column headings such as High Touch I, High Touch II, High Touch III, Bathroom Surfaces and Equipment Surfaces.
Each Monday, the guest services director and his supervisors met with IP leadership to collaborate on which locations needed testing. For example, an IP leader might say, “You have tested 16 rooms on the sixth floor, but I don’t have validation of any rooms on the second floor. Would you test tables, doorknobs and phones in patient rooms on the second floor?” In this way, ES supervisors tested 678 surfaces for an overall environmental pass score of 78 percent and 82 percent at the two hospitals from November 2011 to September 2012. Each unit was given its own score via the CDC spreadsheet.
In November 2013, the IP team purchased its own monitor so that infection preventionists could assist with audits. By September 2014, an additional 796 audits had been collected for passing scores of 94 percent and 92 percent at the two hospitals.
Results were shared with the organization at its quality and patient safety council meeting, infection prevention committee meeting and board quality meeting. The unit-based scores were helpful because they allowed the guest services director to align his employees with each unit’s need. Some units needed faster turnarounds while others needed a more thorough disinfection process.
Additionally, the emergency department used the results of its initial low scores as impetus for a renovation project.
Uptick in Clostridium difficile
During this time, the IP team noticed an increase in Clostridium difficile infection (CDI). The hospital lab began using polymerase chain reaction (PCR) testing to more easily identify CDI. Test results were available within an hour instead of days. Moreover, PCR testing is much more sensitive.
In the first month of use, the CDI rate tripled. This included hospital, health care-associated, community-associated and recurrent CDI.
Additionally, in January 2014, the CDC eliminated the recurrent category from its reporting requirements. A patient with CDI was counted as hospital-acquired based on a hospital stay greater than three days, even if the patient had been diagnosed previously. Suddenly, it seemed as if CDI cases were exploding.
C. difficile is difficult to eradicate from the environment. The bacterium is extremely hardy and can contaminate hands and the environment, which can then be transmitted from patient to patient. Because it is spore-forming, most hospital disinfectants such as quaternary ammonium compounds do not destroy C. difficile spores. The ES team began using bleach-based disinfectants for those identified with CDI upon discharge.
In September, the nursing house supervisors and the infection preventionists teamed up. All agreed that when a patient diagnosed with CDI discharged in the evenings, weekends or holidays, the nursing house supervisor would conduct ATP testing. The IP team would swab test during the day. With each discharge, five room surfaces were tested once an ES staff member had completed room disinfection.
Because there are many nursing house supervisors who cover both St. Francis hospitals and work during the evening hours, an infection preventionist created and laminated ATP testing reminder cards. The IP professional attached a card to each of the two additional monitors that nursing purchased and gave nurses in-service training.
The guest services director and his supervisors continued to conduct random audits and all sent their results to the infection preventionist, who entered all of the swab results into the CDC spreadsheet. Random testing also began to occur in dialysis, the operating rooms and the newborn nursery.
As it turned out, the nursing house supervisors loved testing. They wanted to test more than five surfaces. If a room surface failed so that it required another disinfection, they wanted to retest. They wanted to test surfaces outside of the patient’s room. In fact, the ES and IP professionals had to hold them back by sticking to five swabs post-CDI discharge and room disinfection.
Whenever a room was tested, results were given immediately to the ES professional who had performed the room disinfection. If the surfaces in the room passed, then the ES person was told “great job,” but if a surface did not pass, the ES person was asked to return to the room to disinfect again. Each time a room is tested, guest services receives notice as well. Consequently, in 2014, 1,436 surfaces were tested at both St. Francis hospitals.
Because the CDC refined its definition for hospital-acquired CDI and for other commonly identified HAIs, it is difficult to determine what effect ATP monitoring has had on reducing the risk of health care-associated infections. The ATP monitoring program also coincided with an increase in the overall rate of community-onset CDI, making it even more difficult to establish a causal relationship.
However, the ATP testing program has instilled more confidence in the ES department’s credibility. Prior to testing, there was no method to validate the patient room disinfection performed by ES staff. Now, hospital employees feel reassured that when a patient admits to a room, it is clean and ready for use.
As more of the 15 Bon Secours hospitals learned of the process that was implemented, it was judged a best practice that all should follow. As a result, each hospital purchased at least one ATP monitor and a policy was written. Ultimately, the St. Francis process was implemented at all 15 hospitals.
A united front
Projects like Bon Secours’ adoption of ATP testing can provide a template for other ES, IP and nursing professionals who are seeking to work beyond their silos to form a united front against HAIs.
Michelle Bushey, R.N., MPH, CIC, is director of infection prevention and patient safety, and Bill Clough, CHESP, is administrative director of guest services at Bon Secours St. Francis Health System, Greenville, S.C. They can be reached at Michellem_Bushey@bshsi.org and William_Clough@bshsi.org, respectively.
For further reading
The references noted in this article can be accessed at the following websites:
• Centers for Disease Control and Prevention’s toolkit titled “Options for Evaluating Environmental Cleaning"
• American Journal of Infection Control article “Evaluating hygienic cleaning in health care settings: What you do not know can harm your patients”
• Centers for Disease Control and Prevention’s Guideline for Disinfection and Sterilization in Healthcare Facilities, 2008


