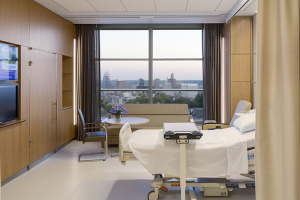
Dignity in design for pediatric behavioral health facilities

At University of Minnesota Masonic Children’s Hospital, semitransparent materials between intake and treatment spaces and warm finishes such as wood window seats reduce feelings of anxiety for patients.
The case for more and better mental health care has never been louder as communities struggle with years of neglected services and overwhelmed emergency departments. With greater understanding of the links between behavioral health and physical health, the focus is sharper than ever on mental health services.
However, the picture of what behavioral health care looks like is unclear for most providers. By understanding the differences, organizations can pursue designs that communicate an appropriate welcoming message. The design strategy is one that is human-centered, finding a balance between dignity and safety. With a patient whose world is out of proportion, the idea is that the environment becomes part of the care regimen to help ground the patient back to reality.
Over the past couple of decades, the physical health care environment has evolved significantly as more is learned about the role physical space plays in the outcomes of patients. A warmer, more comforting environment can help patients heal faster, accommodate families in their care better and serve the staff more efficiently. So, it would seem natural that those practices should be adopted in behavioral health care spaces.
Thoughtful balance
When designing a children’s behavioral health facility, the most important questions are: What can the design do to make children feel comfortable? How can the design make parents feel confident they are making the right decision? What can design do to create the safest environment for effective treatment?
The ideal environment also considers how family members feel the minute they walk through the front door. First impressions can be lasting impressions. From the overall first impression to the fine details, the built environment can influence the perception of the quality of care. Together, the quality of care and environmental design can provide a sense of reassurance for parents, allow caregivers to provide successful treatment, enhance patient satisfaction, improve outcomes and ultimately speed the healing process.
Also in this article |
| Designing for safety |
|
|
The environment in which the patient is admitted can either amplify the illness or immediately begin to treat it. One of the family's first encounters is with the admitting process. As for the child or young adult who struggles with mental illness, an admission into a behavioral health facility is often not easy. Suffering from a disorder that can manifest itself in adversarial behavior, the symptoms of the disorder can increase early in the admission process as the patient enters an unfamiliar environment marked by limits and boundaries.
For the patient, the unfamiliar setting is compounded by parents who are exacerbated, concerned and sometimes fear for the safety of their child. When they arrive at a facility, they should enter through a space that feels calm and respectful rather than institutional. Transitions between spaces are carefully considered and may include features such as semitransparent doors so the patient is offered a glimpse of the activity within the unit before entering, reducing apprehension that may be associated with an unknown space. The admitting process should be intentionally designed to instill confidence in patients and families.
Safety and security
An overall goal for designers may be to create a space that is a warm, caring and beautiful, but safety must be embedded into every design decision. It is imperative that the design of the built environment ensure safety, not only for the patient, but also for families and staff. Meanwhile, security should be seamlessly integrated into the design, allowing caregivers to provide effective treatment and focus on care activities.
Therapy, durability, safety and security are not always mutually exclusive. Purposefully planned care environments can contribute to reduced incidents of restraints and seclusion to protect staff and other patients. High-
quality facilities also can help to improve the outcomes for patients and change the way the community views and accesses behavioral health care.
The small details make design for behavioral health challenging. Found throughout the unit, new anti-ligature designs are creating better environments for patient privacy and dignity. From sentinel event-reduction wood bathroom doors to safe sprinklers and door hardware, the environment feels less institutional, yet improves patient safety.
Details communicate messages to the patient — locked doors, hinges on a door, windows at the end of a long hallway. Understandably, previous design practices often looked at these elements with an eye toward prevention and durability. The unfortunate outcome of such practices is that the safe environment often assumed the look of a highly institutional environment. Therapy meant restriction of movement, choice and comfort.
You may also like |
| Building better behavioral health facilities |
| Pediatric facility designs embrace family |
| Guiding strategies for behavioral health care |
|
|
Design as therapy
A walk through the entrance of University of Minnesota Masonic Children’s Hospital, Minneapolis, finds that patients are greeted with colorful, nature-focused designs intended to reduce the fear children often have going to a clinical environment. Parents with a mild understanding of what ails their child as well as confidence in the care they are accessing play into that strategy by complementing the environment with assurances to the child that he or she will be fine.
Much of it begins with the intake process. At Pine Rest Christian Mental Health Services, Grand Rapids, Mich., the Van Andel Center uses a mix of wood and stone, including design features such as a fireplace, to create a warm and welcoming atmosphere. The colors and art in the entrance feel familiar, evoking images of the western Michigan region where the center is located. Carpeting in the entrance helps to mitigate sound that otherwise could create a more chaotic environment.
Wood accents can soften a place traditionally designed to prevent against injury and self-harm. Strategically designed color patterns on the floor can give patients personal zones where they feel safe while still integrating them into the patient community. On the patient room level, a well-positioned desk can give patients a secondary, inviting place to sit in a room.
By changing the physical image, organizations — even those with higher acuity levels — can evoke a positive response from the moment patients arrive. Controlling for sight, smell and sound, facilities can help patients start to de-escalate at the beginning of a stay, which also helps to create a safer encounter for staff. As research has demonstrated, utilizing the physical structure as an element of care can help patients feel that they can develop coping skills to aid in controlling their behavior, emotions and lives rather than feel as though they are being controlled.
Benefits of choice
A study of the remodeled child and adolescent behavioral health unit at the University of Minnesota Masonic Children’s Hospital, published in the October 2016 issue of Health Environments Research & Design Journal, found that “design features in which patients have choice and control offer greater perceptions of calm during their stay.”

The open environment in the inpatient unit at Pine Rest Mental Health Services’ Van Andel Center allows patients to build a sense of control over their actions while creating an environment in which they can feel both physically and mentally healthy.
In the unit, choice takes on many shapes. In patient rooms, light dimmers and color-changing accents allow patients to set the lighting and music levels they desire to help them feel calm and regulate their bodies. Different seating options including a window bench and desk with chair give the patient choices on where they find the most comfort. The individual desks allow patients to maintain a sense of dignity and personalization while the curved window bench provides an option for patients to curl up, creating feelings of individual comfort, security and safety.
At the entrance to rooms, floor patterns create “front porches” for patients who may want to leave their room but still don’t feel mentally healthy enough to socialize with other patients. This space marks a transition zone between patient room and community space, allowing patients to orient themselves to a more public atmosphere while transitioning in their treatment journey. Half-moon shaped seats are integrated near or within these zones to give patients a place to sit and feel part of the social environment without feeling forced to socialize. They also provide staff with the option to sit on the seats and talk with patients who feel more comfortable inside the private zone of their patient rooms rather than out of it.
Complementing the patient rooms, spaces such as sensory rooms, quiet rooms and activity rooms provide patient choices on where to go to re-regulate their minds and bodies or spend time in therapeutic activities. The sensory room is equipped with multiple elements to engage patients — an LED bubble column, zip line, hammock swing, user-adjustable lighting and vertical writing services.
In the quiet room, gently curved walls with soft colors create a calming atmosphere that includes cozy seating choices, user-adjustable lighting, window bench and a circular wall alcove with curved bench. The alcove provides patients a place of retreat, focused relaxation and sense of protection.
The activity room offers patients a space for large-muscle movement with an interactive video gaming system and large projection screen as well as adjustable accent lights to personalize the atmosphere. Interactive floor tiles encourage movement and creativity.
Together, the rooms give patients options to spend time in activities outside of their patient rooms. Individually, they provide spaces that match the unique needs of each patient. The sensory room has become the “heart of the unit” as described by staff, giving them a room in which to guide patients with “active energy” away from other patients to avoid a negative contagion.
In the University of Minnesota Masonic Children’s Hospital study, staff noted that the positive impact of offering choices to patients in what they can do and where they can go allows them to practice positive coping skills. In one interview, reflecting on the sensory room in particular, a staff member said, “There are a number of kids who ask, ‘Can I go there if I’m having a hard time?’” The elements create a convenient environment for patients to self-recognize which spatial strategies might help him or her cope with behavioral or emotional challenges.
The study also found that the option-laden environment allows patients and staff to work together, brainstorm and address patient needs in a collaborative manner. It has led to fewer incidents when staff have had to physically restrain the patient, leading to fewer injuries.
Dignity-focused
The unintended consequences of previous behavioral design strategies that emphasized safety exclusively often created harsh environments with severe physical and perceived boundaries between patients and staff.
Through a more empathetic and patient dignity-focused design approach, designers and facility operators are uncovering opportunities to see the space beyond its protective value.
Design elements for modern behavioral treatment centers that provide more space choices, user environmental controls, nature-inspired colors and artwork, and comfortable furnishings create an environment that expands the toolkit for staff who work with innovative care models.
Behavioral health facilities can be deinstitutionalized while still incorporating supreme safety features, providing welcoming aesthetics with high durability, and promoting dignity for patients and their families.
Stephanie Reem, CID, CHID, EDAC, LEED AP ID+C, is senior interior designer at BWBR, Saint Paul, Minn. She can be reached at sreem@bwbr.com.