Hand hygiene device makers expect growth

Despite significant advances in hand hygiene compliance monitoring (HHCM) systems, actual usage remains relatively low, according to manufacturers that supply the nation’s hospitals.
“Based on recent data we’ve collected, about 90% of hospitals are still measuring hand hygiene performance with pen and paper, while 4% are using electronic monitoring, and an additional 4% are reporting manual observation through a mobile application, such as iScrub, which we acquired in 2018,” says Yuri Malina, co-founder of SwipeSense Inc., Chicago, who adds that the remaining 2% of respondents declined to participate.
However, manufacturers believe that patient safety and satisfaction initiatives will drive greater growth, reinforced by increasing focus from accreditation authorities and The LeapFrog Group’s Leapfrog Hospital Survey on the quality of analytics for hand hygiene compliance. Additionally, they say, more clinicians are accepting HHCM systems.
“We are seeing a substantial increase in active SmartLink hand hygiene deployments over the last 12 months,” says Tim Cambier, business development senior director at Gojo Industries Inc., Akron, Ohio. “Hospitals realize that hand hygiene is foundational to patient safety and is the primary measure to prevent health care-associated infections (HAIs) in health care facilities. It also is one of the only metrics in which every single person in the hospital has a stake.”
Value proposition
Clinicians and other employees see the value in HHCM technology as it streamlines their processes and directly contributes to the ultimate objective of improving patient care, according to Jacob Wischnia, director of business development at CenTrak, Newtown, Pa. “As adoption of real-time locating systems (RTLS) has gone up, adoption of electronic hand hygiene compliance monitoring systems has followed this trend.”
Clinicians are more likely to adopt HHCM systems that fit into their clinical workflow and provide reliable data and feedback, experts agree. If systems are difficult to integrate into patient care activities or use a “blame or shame” approach with negative performance feedback, clinicians are less likely to adopt them into practice.
“Health care organizations must teach their clinicians that the tool is being used collaboratively to improve compliance and increase patient safety and care. Also, the caregivers being monitored must be part of the early discussions about adopting an HHCM system,” says Sagi Geva, director of RTLS solutions at Stanley Healthcare, Waltham, Mass.
Beyond hospitals, market penetration into small off-site facilities is slow but showing growth. “We have seen many of our customers focus on inpatient care units as they establish their new HHCM system,” says Martin McGonagle, general manager of health care at SC Johnson Professional, Charlotte, N.C. “After hospitals incorporate data from the system into their infection prevention strategies and notice the culture change that follows, we see them expanding their installation into outpatient and procedural areas.”
John Lee, president of Proventix, Birmingham, Ala., says that where Proventix has installed its system in small off-site facilities, hand washing monitoring was not the main focus. “Other components such as labor utilization and tracking were the motivating factor for acquiring the system,” he explains.
Small off-site facilities are not a good fit for HHCM systems that are too complex, according to Chris Hermann, founder and CEO of Clean Hands – Safe Hands LLC, Atlanta. “However, the Clean Hands – Safe Hands system has been adopted by a number of long-term acute care and similar facilities because it has a small information technology (IT) footprint.”
Data collection
Data collection from HHCM systems is important because it gives staff the ability to objectively measure hand hygiene events, which, unlike traditional direct observation methods, is not subject to the Hawthorne effect on subject behavior, human error or manipulation.
When hospitals monitor hand hygiene compliance and incorporate the data into patient safety and infection prevention programs, caregivers demonstrate improved adherence to hand hygiene and are more likely to prevent HAIs. “When applied effectively, hand hygiene performance data provides feedback to hospital workers on their performance, promotes increased awareness of hand hygiene practices and identifies opportunities for improvement,” says Amna Handley, director of clinical development at Georgia Pacific’s GP Pro, Atlanta.
Granular-level data collection helps hospital administrators make decisions that improve patient care. “For example, hospitals need to know that only soap is being dispensed when clinicians cleanse their hands, as this is the most effective way to prevent Clostridium difficile from spreading,” Lee says. “Proventix captures this data to help identify any negative outcomes as well as opportunities for improved hand hygiene practices.”
Data can be used as a real-time actionable tool, according to Geva. “Some of our customers display the real-time compliance of caregivers with their names at the nurse station,” he says. “Caregivers can quickly see how they are doing and how they compare to others in their unit, which creates healthy competition.” Such use of real-time data has helped raise compliance rates to 100% with some caregivers, Geva adds.
Seamless interface
The latest HHCM solutions interface seamlessly with other systems and are used more for coaching than as a punitive tool. For example, the DebMed badge-free system from SC Johnson Professional measures hand hygiene performance during direct patient care and provides compliance scores based on the World Health Organization’s My 5 Moments.
Dispensers of any brand are monitored to record hand hygiene events, and data is transmitted wirelessly to a secure off-site server, with no integration with hospital Wi-Fi or IT infrastructure. The software compares hand hygiene event data to opportunities to calculate a compliance rate. Unit-specific details such as patient care needs and hourly unit census are key elements in customizing the benchmark for each facility.
GP Pro has introduced the SafeHaven Personal Hand Hygiene System, a wearable sanitizing device with cloud-based reporting that fits seamlessly into the clinical workflow to provide point-of-care hand hygiene and real-time monitoring with automated positive feedback. The system can be deployed in many health care settings, including specialty areas such as the operating room, special procedures and even home health.
Gojo Industries Inc. recently introduced the Purell SmartLink integrated monitoring system (IMS), which uses Bluetooth low-energy technology to capture hand hygiene events in real time. Through the system’s clinical support feature, education and coaching of front-line staff can be tailored to each unit’s culture and workflows while data management and analysis can help create and improve hand hygiene initiatives.
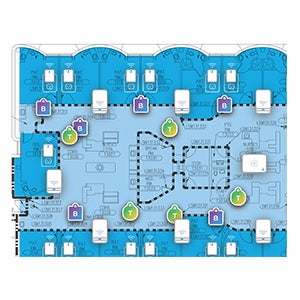
SwipeSense’s HHCM solution is part of a full-stack platform that integrates connected devices, intelligent algorithms and dashboards, providing actionable data and insight. Smart sensors are installed throughout a facility, creating a digital map of a hospital’s most valuable assets: their staff and their equipment. Data is analyzed and reported through user dashboards, providing real-time visibility into critical processes such as hand hygiene compliance, asset tracking or nurse rounding.
The Proventix nGage solution is designed to capture group and individual compliance for detailed feedback to staff. This service coordinates with the hospital’s census data to provide real-time rounding data that prompts staff to avoid missed visits to patient rooms.
Clean Hands – Safe Hands has introduced a number of features to its HHCM solution, including two in-the-moment interventions: A real-time voice reminder uses a human voice to gently remind clinicians to clean their hands when they forget, and real-time text messaging sends a text message to unit leaders when hand hygiene falls below an expected level.
Another feature, the adaptive room modes, allows staff to quickly change room modes based on patient conditions — for example, allowing more time to gown and glove for isolation rooms. Or in Clostridium difficile mode, the voice reminder tells clinicians to use soap and water when exiting the room.
CenTrak’s HHCM solution combines its RTLS platform with hand hygiene software. Staff badges leverage RTLS to communicate with monitors that can be integrated with or mounted to a variety of dispensers and automatically collect hand washing compliance data. The system is deployable as a standalone option or as an interface with other solutions provided by CenTrak’s enterprise location services, such as nurse call automation and staff duress.
The BioVigil HHCM Solution from BioVigil Healthcare Systems Inc., Ann Arbor, Mich., identifies rooms that have been designated for special contact isolation protocols. Different hand hygiene protocols, such as soap and water hand washing, are applicable in such circumstances, so BioVigil sensors recognize and accommodate these situations.
The BioVigil solution also recognizes when a worker has moved between patient care areas without performing hand hygiene and the resulting elevated risk for cross-contamination. The system reacts in real time in these circumstances to alert the caregiver and reduce contamination risk to the patient. Detail and aggregate data sets are available for export, on an ad-hoc or automated schedule, in a variety of formats from the BioVigil data suite.
Stanley Healthcare’s HHCM solution, part of its RTLS platform, is comprised of Wi-Fi badges that are worn by caregivers. The badges are assigned to each caregiver and act as unique identifiers. An analytics module provides visual dashboards that show the compliance data by caregiver role, by unit or for the entire hospital. The interactive dashboards allow users to slice the data by applying filters for date ranges, time of day, shifts and room type.
Ecolab Inc., St. Paul, Minn., offers the Ecolab hand hygiene system, which can track hand hygiene events at the bedside rather than at the door. “This provides more meaningful data in double-occupancy rooms where a health care worker may be moving from one patient to the next,” says Linda Homan, senior manager of clinical affairs. “The system also can be used to identify which workers have come in contact with a patient with an infectious disease.”
The system provides immediate feedback to the worker regarding missed hand hygiene opportunities. It also can support customization to a wide range of workflows and hospital layouts.
Greater granularity
What near-future advances do vendors see for HHCM technology? Sanjay Gupta, CEO of BioVigil, predicts there will be increased migration from direct observation to electronic hand hygiene monitoring to provide more granular analysis and staff accountability.
Neal Lorenzi is a freelance writer and regular contributor based in Mundelein, Ill.

ALL HANDS IN
The Purell Smartlink integrated monitoring system is part of a total hand hygiene improvement solution. Gojo Industries Inc.
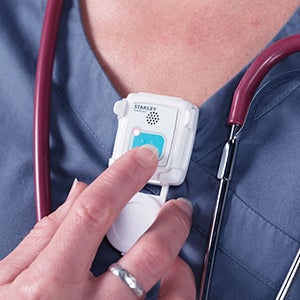
FULL COMPLIANCE
Use of automated monitoring staff badges helps increase compliance rates to reduce risk of health care-associated infections and enhance patient safety. Stanley Healthcare
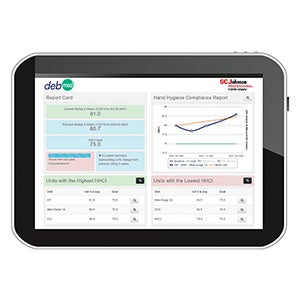
EXACT LOCATION
The DebMed Dashboard provides highly customizable reporting based on facility, unit and room-level compliance for any given period of time. SC Johnson Professional

GOOD TO GO
This badge reminder sequence displays green, yellow and red lights to alert health care workers to clean their hands. BioVigil Healthcare Systems Inc.

FLEXIBLE DESIGN
CenTrak’s electronic hand hygiene monitoring system captures 100% of hand hygiene events and is deployable as a standalone solution or as part of enterprise platform. CenTrak

HELPFUL FEEDBACK
The nGage Communication Unit is placed next to any soap or sanitizer dispenser and records each time a health care worker washes or sanitizes their hands. Proventix

BEDSIDE SOLUTiON
The Ecolab Hand Hygiene System can track events at the bedside, providing more meaningful data in double occupancy rooms. Ecolab

GERM KILLER
SafeHaven Personal Hand Hygiene System provides point-of-care hand hygiene and helps prevent the spread of health care-associated infections. Georgia-Pacific
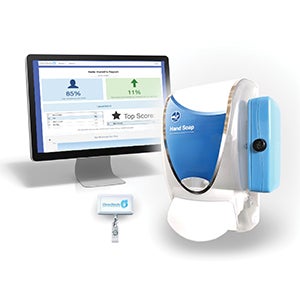
WITH THE FLOW
The Clean Hands – Safe Hands system is lightweight, nonintrusive and doesn’t interfere with clinicians’ regular workflows. Clean Hands – Safe Hands LLC