Hospitals and health systems adapt to fight COVID-19

Patient care units under construction inside the Jacob Javits Convention Center in New York City.
Image by James D’Ambrosio
Disaster planning and emergency preparedness have taken center stage as U.S. hospitals battle the COVID-19 pandemic that, by mid-March 2020, had threatened to overwhelm hospital staff and resources nationwide.
“This is unprecedented,” says Chad Beebe, deputy executive director, American Society for Health Care Engineering (ASHE) of the American Hospital Association. “There’s no way we could have realized all of the potential problems.”
It was a month between the first reported case of COVID-19 in the United States on Jan. 21 and the first case of suspected local transmission. In one month more, New York City had seen more than 15,000 people test positive for COVID-19, roughly half the total number of infections in the country.
At press time, hospitals and health systems across the nation followed New York’s lead in bracing for a patient surge.
Moving to temporary facilities
The upshot is that many hospitals and health systems are entering uncharted territory. Meeting the sheer volume of patients coming in for respiratory distress has been a leading challenge, as public health experts predict anywhere from tens of thousands to millions of U.S. citizens will need hospitalization for COVID-19 during the pandemic.
In preparation for a surge, ASHE has created an online resource page, ashe.org/covid19resources, to help facilities managers and engineers reduce the spread of coronavirus through best practices in the physical environment. The page also features concept studies and webinars to help health care organizations convert alternate spaces such as schools and hotels into temporary patient care spaces.
Hospitals across the United States have erected triage sites in parking lots and at medical offices to separate COVID-19-infected patients from others in order to “flatten the curve” of infection. Reid Health, Richmond, Ind., for example, has converted an urgent care facility to solely address respiratory illness. The system opened a nearby temporary facility to address nonrespiratory urgent needs.
“This will allow us to better manage potential COVID-19 patients and patients with other signs and symptoms of respiratory disease with a dedicated space, and processes to expedite evaluations and decisions about further care,” says Annuradha Bhandari, M.D., Reid Medical Associates. “It will also help us keep potentially infected people away from those who likely are not.” The dedicated clinic is also expected to relieve pressure on nearby emergency departments.
However, health systems in the worst-hit areas — including the New York City epicenter — have gotten creative in converting non-health care spaces for temporary patient care.
“We are even looking at the potential possibility of utilizing cruise ships for some type of health care facility,” Beebe says. “We also are looking at CONEX-type containers and how those can be utilized to build temporary hospitals. The most desirable solution so far is converting hotel space for caring for patients with lower acuity.”
The Center for Health Design is working to connect hospitals with that desirable space through its MakingRoom online database. Hospital representatives can submit their space needs at www.healthdesign.org/makingroom, and owners of hotel or high-occupancy residential facilities can volunteer their space to meet those needs in real time.
The American Institute of Architects and its Academy of Architecture for Health have also developed the COVID-19 ArchMap that describes health systems’ strategies for meeting space needs. Facilities can post solutions ranging from temporary hospitals to HVAC adaptions that meet negative air pressure needs for airborne infection isolation rooms. The map includes contact information to connect facilities in need with solutions.
Convention centers nationwide are also on standby to serve as temporary medical stations. The U.S. Army Corps of Engineers (USACE) is taking the lead here, beginning with a conversion of New York City’s 160,000-square-foot Jacob Javits Center into a Federal Medical Station with up to 2,000 beds. The center will house non-COVID-19 patients, thus allowing better-equipped hospitals to focus solely on treating patients with respiratory complications.
However, as Beebe points out, securing this space is only half the challenge.
“Our members are working on setting these spaces up, and they’re looking around and thinking, ‘Once I have this space set up, who is going to staff it?’” Beebe says.
These spaces will also need to be supplied with medical equipment that someone will have to maintain, he adds.

USNS Mercy arrived in Los Angeles March 27 to support the nation’s COVID-19 response.
U.S. Navy photo by Mass Communication Specialist 1st Class David Mora Jr./Released
“A temporary facility is going to be labor intensive,” he says. “You have to be there to troubleshoot issues on the fly.”
Recognizing this multifaceted challenge, the Navy deployed two ships to offer relief.
In New York City, patients without COVID-19 are being diverted to the 1,000 beds aboard the U.S. Naval Ship (USNS) Comfort. The USNS Mercy serves the same role in Los Angeles. The ships contain 12 operating rooms, a medical laboratory and two oxygen-producing plants, among other features.
As hospitals seek new ways to create more care sites, they are also using telehealth to keep non-COVID-19 patients at home and free up existing spaces for more acute patients, such as those experiencing respiratory distress.
Mount Sinai Health System in Brooklyn has adapted its Telestroke program to keep stroke patients and clinicians at home. The program had been implemented several years ago to bring off-site stroke-team specialists into the exam room to assist with diagnoses. Now the team is treating high-risk patients using telehealth, keeping patients at home. The technology also allows the system to implement a work-from-home policy for its care providers.
Many patients don’t need urging to reach out through telehealth rather than coming in for care. As of March 20, Geisinger Health says it had seen a 500% increase in telehealth visits and trained and equipped 1,000 additional clinicians to provide this care.
Geisinger CIO John Kravitz noted during a podcast with The Big Unlock that this pandemic could be “the tipping point for people to really use telehealth.”
Infection prevention emphasis
Regardless of the environment, limiting the spread of infection quickly became the No. 1 driver, making environmental services (EVS) professionals an even more central part of the front-line care team. However, as hospitals face challenges in equipping staff with appropriate personal protective equipment (PPE), anxiety was running high at press time.
“There has been a great deal of press around PPE running low — and, in some places, rightfully so,” says Brad Winnie, CHESP, president of the Association for the Health Care Environment (AHE) of the American Hospital Association and director of environmental services at North Shore Medical Center in Miami.
“We’re telling EVS leaders to partner with nursing. If you’ve got a COVID-19 patient who’s in airborne isolation and you’re running low on PPE, partner with nursing to minimize the number of people going in and out of the room. Give nursing some just-in-time coaching on how to clean and disinfect the high-touch surfaces.”
He advises EVS to work with nursing staff by providing approved ready-to-use wipes to clean high-touch surfaces after they attend to patients. “Then, upon discharge, EVS will go in and follow the discharge cleaning process for the stated isolation,” Winnie says.
Winnie also is reminding EVS leaders to reference AHE’s online resource at ahe.org/covid-19-resources-evs-professionals-2020, which is filled with tools to use against this new threat.
“COVID-19 is caused by a new or novel coronavirus from a family of coronaviruses that caused MERS and SARS, so EVS has experience,” he says. “Working as a well-informed hospital team will help all of us get through this even though there are some things we may not yet know.”
Winnie also notes that AHE’s online member community has been filled with discussions about how to field concerns from staff who may be anxious to be on the front line of the pandemic. AHE is working to increase that confidence by offering the online portion of its Certificate of Mastery in Infection Prevention as a solo course for a reduced fee.
Designing for new normal
In the meantime, designers, architects and engineers are also evaluating the physical environment solutions that seem to be the most successful in helping to manage this pandemic. Many of those solutions could emerge as future best practices in medical facility design.
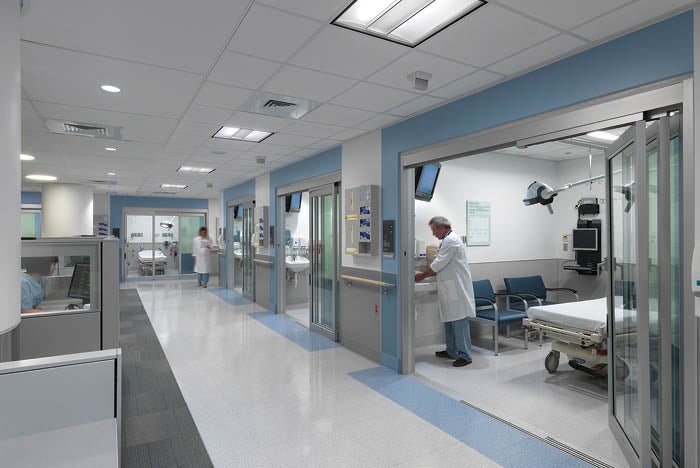
Rush medical center’s ED is designed to prevent the spread of airborne diseases.
Image by James Steinkamp Photography
For example, mechanical, electrical and plumbing contractor Dynamix Engineering points to the 2014 expansion of the Lexington Medical Center in South Carolina. The project added 250 beds, including 60 dedicated to critical care and 100 stepdown. Because the hospital’s goal was to build in flexibility to anticipate a wide range of problems, the project also included an HVAC system that allows for patient rooms on entire floors of the patient wing to operate in negative pressure when needed. This allows Lexington to change room and floor conditions at the touch of a button.
At the onset of the COVID-19 pandemic, Lexington reached out to Dynamix for advice on how to adapt its HVAC system. Dynamix responded with a list of possible control changes and, within 12 hours, the hospital had created 12 additional negative-pressure rooms and was working to convert entire floors.
In Chicago, Rush University Medical Center built its hospital tower in 2012 in anticipation of an emergency event. The center’s lobby features columns equipped with electricity and medical gases to supply patients during a surge. As the hospital now prepares to treat more COVID-19-infected patients, that feature seems a particularly prescient choice.
The hospital also was designed to serve as one of the nation’s premier bioterrorism preparedness facilities. The emergency department can be divided into three 20-bed units, each of which can be converted to a negative-pressure space. To further limit the spread of infection, the ambulance port leading to these treatment areas was designed with decontamination showers and space for tents and triage assessment areas.
Into the unknown
While many continue to study this novel virus in hopes of finding a cure, Dr. Omar Lateef, CEO of Rush, says that hospitals have moved from preparedness planning to action, and will continue working to prohibit its spread.
“While COVID-19 and other infectious disease threats are deeply troubling and create tremendous anxiety, it is important to consider that all such new threats are ‘novel’ at first,” Lateef says.
“It is the organizations like Rush University Medical Center and others that take them seriously — preparing and drilling to mitigate risks as rapidly as possible — that are best equipped to serve as a community resource and help shape the response to protect public health. It is what we do.”




