Bulk medical oxygen systems
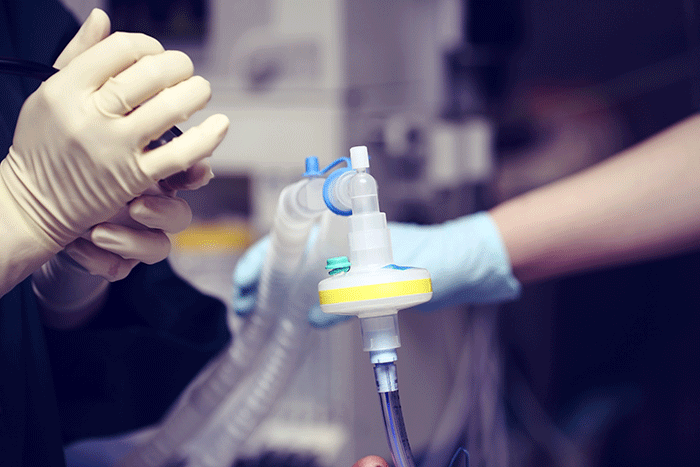
Health care facilities managers know that their internal hospital systems need to be sized to intake the amount of oxygen being demanded by ventilators.
Image by Getty Images
The novel coronavirus, known as COVID-19, is a pandemic that has caused health care facilities managers to take unprecedented steps in managing building systems. One system in particular, the bulk medical oxygen system, can be greatly impacted.
What we are learning and want to share with health care facility managers is the increased high flow oxygen demand within the hospital can be the cause of ice accumulation on the vaporizers that will reduce bulk medical oxygen supply system capacity, which can be relieved with methods known by oxygen suppliers and discussed below. However, most importantly and despite these efforts, the key is that health care facility managers know that their internal hospital systems need to be sized to intake the amount of oxygen being demanded by ventilators.
If the hospital system does not have the capacity to handle a surge of oxygen demand, the hospital can experience a reduction in oxygen pressure or a shutdown of their entire oxygen delivery system. To assist in determining the demand, Medical Air and Oxygen Capacity Tools have been posted to the ASHE COVID-19 Resources webpage.
Extraordinary usage
Extreme pressure has been put on the system due to the patient treatment efforts of COVID-19. According to Patricia Covelle, associate chief nursing officer at Beverly Hospital, an urban facility and a member of Beth Israel Lahey Health System, just outside Boston. “The novel coronavirus attacks the lungs of infected patients, resulting in extraordinary usage of oxygen within the hospital,” she says.
Fortunately, the supply of medical oxygen to hospitals is not currently a concern. Rich Gottwald, the president and CEO of the Compressed Gas Association (CGA), says, “There is no shortage of medical oxygen, nor do we anticipate any shortage.” That is partly because companies such as Airgas USA LLC, Linde plc and Air Products have ramped up production and shifted capacity to serve the most hard-hit areas of the country, he says. The concern is hospital bulk medical oxygen systems may not be sized for the COVID 19 pandemic demand.
On April 17, 2020, Beverly Hospital received a letter from their medical oxygen supplier, Airgas, which reminded the hospital that the bulk medical oxygen supply system installed at their facility has limitations on the amount of vaporized medical oxygen that it can deliver to patients due to the capacity of the customer’s oxygen delivery system.
CGA also encouraged gas customers to understand the facility’s oxygen supply system maximum operating capacity, considering tank volume, vaporizer capacity and in-house piping flow limits. An unprecedented increase in medical oxygen demand (the number of patients needing oxygen above normal conditions) under certain circumstances can lead to shutdown of the hospital’s oxygen delivery system as a whole due to an inability for the hospital’s system to process the required oxygen.
Related to a potential accumulation of ice, systems constructed to the National Fire Protection Association's NFPA 99, Health Care Facilities Code, are designed to vaporize cryogenic (super-cooled) liquid oxygen from the storage vessel(s) using finned aluminum exchangers called ambient vaporizers.
This process occurs in the aluminum coils known as the ambient air vaporizers. Once the liquid oxygen is converted to oxygen gas, the pressure of the gas is pushed throughout the hospital into lines feeding medical oxygen connection ports in patient unit head walls.
By design, the ambient vaporizers will accumulate a small amount of ice at the inlet, while delivering gas near ambient temperatures on the outlet. However, when flows significantly exceed design rates, the ice further accumulates on the vaporizer fins, resulting in less surface area for heat exchange. This drives the delivered oxygen temperatures lower to the point where frost and condensation form on the hospital line, posing risks to the safe operation of the hospital oxygen equipment.
Another limiting factor for the supply system is the capacity of the pressure regulators that deliver the constant pressure during normal operation. These regulators have a fixed-flow capacity, and when it is exceeded, they are not able to maintain the desired pressure.
This will drop the actual pressure in the hospital network possibly setting off alarms and potentially disrupting the operation at the patient use points. There is a critical point in which safe operation of the system will reach its ultimate limit and could cause a shutdown of the entire bulk medical oxygen system.
To understand this further, facilities professionals should consult the “Additional Ventilators May Pose a Risk to Hospital Gas Systems” guidance document published by the American Association for Respiratory Care.
At Beverly Hospital, a typical day’s usage is 12 inches of liquid. However, between April 8 to April 15, the hospital used 22 inches of liquid daily due to an increase in oxygen demand. During this time period, the number of patient ventilators in use, as well as low and high flow oxygen therapy for patients suffering primarily from COVID disease, had increased.
According to the hospital's Respiratory Therapist Manager Alicia Logan, “We seem to have approximately five patients each day using high-flow nasal cannula oxygen (HFNC). These patients are on maximum settings of 60 liters per minute (LPM) at fraction of inspired oxygen (FiO2) 100%. There are also approximately eight to 12 patients throughout the hospital who are on non-rebreather masks running with flushed flow meters, which can generate flows of up to 40-60 LPM as well. Ventilator patients actually require less flow, maybe around 25 LPM.”
Logan advised usually when a patient is on a ventilator, they blend oxygen with medical air. However, in late March to early April, the hospital had 11 patients on ventilators and were using 100% oxygen with no mix. "That's probably where the spike in use is coming from," she says. "The hospital is averaging six to 10 patients on ventilators each day.”
Mitigation strategies
Tho help alleviate the problem, the following mitigation strategies were implemented:
- Vaporizers. The first step after receiving notice from Airgas was to assess the hospital’s current situation. A trip to the medical gas bulk storage area located across a campus road on the other side of the central power plant was made to make observations of the current condition. The following is a picture showing a hospital bulk medical oxygen system with vaporizer showing signs of icing.

Increased high flow oxygen demand within the hospital can be the cause of ice accumulation on the vaporizers.
Photo by Edmund Lydon
Within a short period of time, the facilities staff began the deicing process using steam from the central power plant. Water, hot water, steam are all acceptable approaches to removing the ice buildup. Application of such deicing methods must be done in accordance with the gas supplier so that it is done safely. For example, it is very hazardous to use a mallet or hammer to knock ice from a vaporizer.
The second most immediate step was a visual daily monitoring of the hospital medical gas oxygen system.
In a similar situation, according to WIRED.com, “Two hospitals in Queens, New York, moved 10 COVID-19 patients to a Navy hospital ship docked offshore last week, after their ventilators couldn’t supply as much oxygen as the patients needed. The problem was not with the hospitals’ total oxygen supply or with the ventilators themselves, but with coils of aluminum in which oxygen changes from a liquid into a gas. The fix came from the hoses of the New York Fire Department.”
- Pressure regulators. The hospital must work with their gas supplier to evaluate current and projected peak flows and make necessary adjustments to the system regulators. Potentially, a system upgrade or even supplemental supply might be needed. Coordination with hospital personnel is critical to monitor the pressure at the source and in the hospital during the demand and after.
- Other elements. Emergency oxygen supply connections (EOSC) are required by NFPA 99 and should be checked that they are readily accessible to allow connection of a temporary auxiliary mobile source and that all facility and security staff are aware of the location.
Work with suppliers
For additional information, facility managers should work with medical oxygen suppliers and review the applicable content in the governing codes for medical supply systems and health care facilities (NFPA 99 and NFPA 55, Compressed Gases and Cryogenic Fluids Code). This is to ensure safe elements of the medical oxygen installation continue to be in place, such as safe distances from oxygen hazards, delivery access and security.
Edmund Lydon, CHFM, FASHE, is senior director of facilities and support services at Beverly Hospital, a member Beth Israel Lahey Health System. He can be reached at edmund.lydon@lahey.org.




