Five ways to improve IAQ
Indoor air quality (IAQ) has never been more important in health care. While it’s good to acknowledge this fact, turning awareness into action to advance IAQ isn’t quite as simple. There are competing priorities that result from the need to keep hospitals and clinics operating safely and efficient. The fiscal considerations are also significant. COVID-19 has not only put pressure on the system from a care perspective, it has caused acute financial stress.
According to the New England Journal of Medicine Catalyst Connect, “The intensity of care required for treating COVID-19 patients and maintaining isolation has strained both labor and supply costs.” As a result, health care facilities may not be able to allocate funds for major heating, ventilation and air-conditioning (HVAC) upgrades to address air quality.
It’s a definite obstacle but not a dead end for IAQ improvements. Based on recommendations from ASHRAE, the Centers for Disease Control and Prevention and other organizations, there are steps that building operators can take to modify and fine tune existing HVAC systems to deliver cleaner, healthier air. Plus, many of the measures are low-to-no cost.
Here are five core HVAC domains and potential changes for facilities managers to explore — territories and modifications that can pay immediate IAQ dividends.
Filtration
A comprehensive analysis of building filtration strategies is a fundamental first step, which can guide a variety of IAQ-boosting measures. ASHRAE states that, “The use of highly efficient particle filtration in centralized HVAC systems reduces the airborne load of infectious particles.” Specifically, ASHRAE recommends upgrading to MERV 13 filters, which capture 50% of 0.3 to 1 micron-sized particles, such as bacteria and sneeze nuclei, or employing the highest achievable filtration.
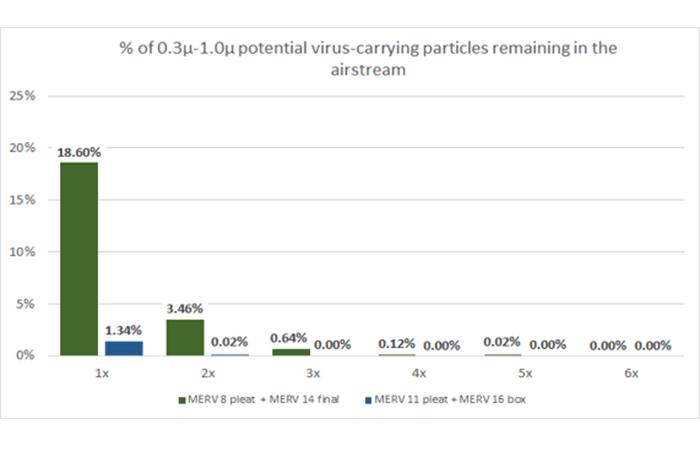
In tests, the combination of a MERV 11 prefilter and MERV 16 final filter removed 98.66% of potential virus-carrying particles after the first pass.
Image courtesy of Daikin Applied
The “or” is important because, due to high demand and supply constraints, MERV 13 filters can be difficult to source. (The membrane for these filters is built using the same material found in N95 masks and other personal protective equipment, a significant reason for the current shortage.) Consequently, it may be necessary to step up to the MERV 14 to 16 range or down to MERV 9 to 11, which all are effective in producing hygienic environments.
A multi-filter strategy is also highly beneficial. Many hospitals in the U.S., for example, rely on a MERV 8 prefilter with a MERV 14 final filter. Upgrading to a MERV 11/16 combination removes 98.7% of 0.3- to 1-micron particles after the first pass; it takes three circulations to achieve the same efficiency using the more common approach. A simple step such as sealing filter edges to limit bypass improves effectiveness as well.
It’s important to note, however, that while increasing filtration may reduce the transport of infectious aerosols, it may result in additional stress on supply fans and lead to higher energy cost. If changes to the central system are not practical or possible, consider adding portable room air cleaners with HEPA or high-MERV filters.
Ventilation
Increasing outdoor air ventilation is one of the cornerstones of ASHRAE’s recommendations for enhancing IAQ. There are several straightforward means and measures toward that end.
Cleaning cooling coils in an HVAC system will recapture lost heat transfer from fouling and improve ventilation. Disabling demand-control ventilation and opening dampers to 100% as indoor and outdoor conditions permit help as well. And when pandemic concerns exist, it’s best to bypass energy recovery wheels that could leak exhaust air back into the outdoor air supply.
Take these steps and assess current capabilities before making major hardware or building automation system (BAS) investments. If a capital outlay is necessary, using equipment that can operate efficiently at lower part loads, along with next-generation compressors, electronically commutated motor fans, and plug-and-play remote monitoring technologies, balances ventilation needs and energy use.
Air cycling
Developing a strategy to conduct a building purge at the optimal temperature and humidity levels, based on time of day and outdoor air conditions, is also essential. It allows for more air exchanges and keeps the cost of cycling in clean air to a minimum. Increasing the air changes per hour — from two to six in a patient room, for instance — has a positive IAQ impact, as well.
ASHRAE also suggests operating HVAC systems with maximum outside airflows for two hours before and after occupied times. Of course, this is heavily dependent on geography. A clinic in Florida won’t be able to adopt the protocols in the summer months, whereas a facility located in New York will have ample opportunity to adjust its cycling practices in the fall.
Humidity control
Humidity regulation is all about finding equilibrium. If relative humidity levels are low, dry airborne pathogens can exist longer and travel further. And, on the other end of the spectrum, high levels can lead to mold, mildew and related issues.
Testing and scientific evidence have shown that a mid-range of 40% to 60% relative humidity creates ideal conditions for human health, decreasing virus “float” and survival times, and boosting immunity. According to Dr. Stephanie Taylor, an infection control consultant at Harvard Medical School and member of the ASHRAE epidemic task group, “This is the optimal level for our respiratory immune system and will reduce the spread of seasonal respiratory illnesses and their burden on society.”
Adding in-room relative humidity sensors and interlocking them with variable air-volume controllers is a basic, yet effective way to monitoring and control inside air conditions. More complex solutions depend on a facility’s existing control strategies and BAS.
Remote monitoring
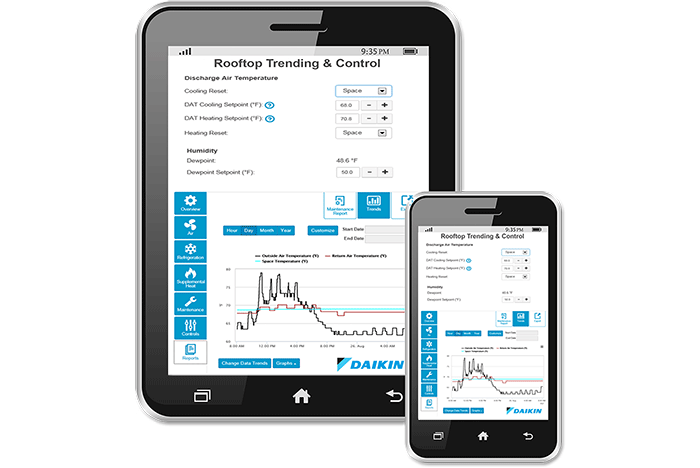
Remote monitoring technology allows facility personnel to view and manage HVAC equipment performance while limiting on-site exposure.
Image courtesy of Daikin Applied
COVID-19 has changed any number of protocols and procedures within health care facilities. It has altered how occupants access and navigate buildings, or if they even enter buildings. Hospitals and clinics often have to limit the number of people on-site. The transformation also extends to the hardware and controls at the heart of the physical structure. Comfort remains the driving force behind the sequence of operations for HVAC, but its definition has expanded to include IAQ and risk mitigation from infectious aerosols.
Fortunately, technology advancements have made it easier for facility personnel to adapt.
Remote monitoring and maintenance in particular have helped address both occupancy constraints and air-quality needs. Operators can now track key IAQ indicators such as economizer operation, fresh air ventilation and humidity remotely, and address faults as needed. If a site visit is required, technicians can arrive more informed of the issue and with the necessary parts.
The expense of remote monitoring systems has been a barrier in the past but costs have dropped significantly as sensing technology and cloud connectivity have become ubiquitous.
While there is no silver bullet to eliminate the issues presented by COVID-19 or other airborne pathogens and viruses, experts agree there are multiple measures — both immediate and longer term — that the health care field can employ to clean the air and decrease potential risk.
Garrett Holloway is health care market manager at Daikin Applied. He can be contacted at garrett.holloway@daikinapplied.com.




