Exploring the use of hypochlorous acid for disinfection
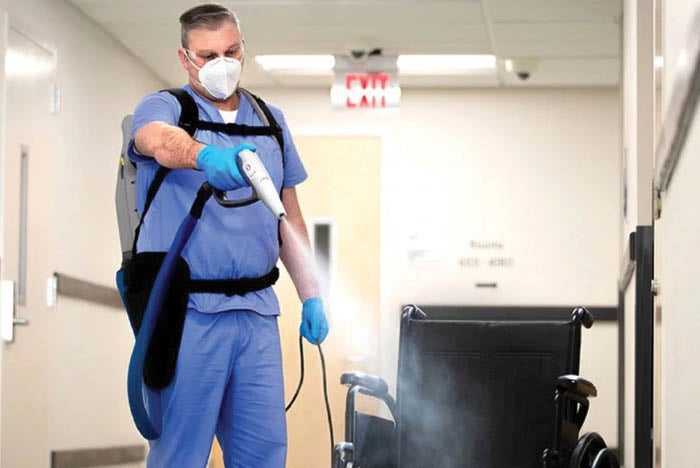
An environmental services staff member using an electrostatic sprayer.
Image courtesy of the author
In 1834, the French chemist Antoine Jerome Balard discovered hypochlorous acid (HOCl) when he added a dilute mix of mercury (II) oxide in water to chlorine gas. Additionally, he discovered that HOCl was an effective and safe disinfectant solution.
Later in the 19th century, Michael Faraday was the first scientist to develop a successful technique that generated HOCl from saltwater. The process was called and continues to be known as electrochemical activation.
Although HOCl was a safe, nontoxic and effective solution to many problems, it was complicated and expensive to maintain a stable version of HOCl with a long shelf life. It was not until recently that scientists were able to produce and maintain stable and cost-effective HOCl and it became suitable for commercial use.
Powerful oxidant
HOCl is the most powerful oxidant in the chlorine family — more so than sodium hypochlorite (bleach). It has a weak, slightly acidic, neutral pH of 5-7 and naturally occurs in all mammals’ white blood cells. HOCl has been around since the dawn of animals and humans. It is soluble in water and forms an effective disinfectant; it benefits from being a nontoxic solution.
HOCl has a neutral charge; therefore, it does not repel bacteria but attracts them. HOCl easily penetrates bacteria walls, resulting in it quickly killing the cells.
Medical professionals know that HOCl is naturally present in all protecting and healing mammals; that includes close to 8 billion humans. HOCl defends against all manner of pathogens and potential pathogens that attack the body from both outside and inside.
HOCl is used in wound care, skin disinfection, food safety, water treatment, purification of oil and natural gas wells, deodorization and skin products, and as a food-safe sanitizer on both food products and food preparation surfaces.
It is a strong disinfectant in health care and is an excellent cleaning solution.
The World Health Organization includes HOCl in its list of essential medicines, based on the following approvals:
- The Food and Drug Administration (FDA) approval for uses on food products like meat, fruits and vegetables as well as on food-contact surfaces, utensils and other food-processing equipment.
- The FDA’s approval of more than 10 medical-grade HOCl solutions for wound care.
- The Department of Agriculture’s approval for use in the National Organic Program.
- The Environmental Protection Agency’s (EPA’s) approval as a no-rinse food sanitizer and for use in drinking water as well as 17 product approvals for COVID-19 disinfection purposes.
- Health Canada, the Australian government and the Japanese National Institute of Technology and Evaluation’s use against coronavirus.
During the COVID-19 pandemic, many countries introduced continuous HOCl misting and fogging tunnels for entry and exit corridors at mass transit facilities. Buildings, including hospitals, used them to disinfect anyone entering their facilities.
Easily generated on-site, HOCl is so effective and inexpensive that even developing nations use misting and fogging tunnels at entrances to health care and business occupanies. Many developing nations also use HOCl misting tunnels as a prerequisite to ambulance stretchers entering hospitals. Some of the most populous cities, such as Mumbai, found HOCl use in hospitals and train terminals reduced the number of citizens potentially exposed to the SARS-CoV-2 virus.
Hospital usage
Given the wide acceptance of HOCl, the following questions must be asked:
- Why are hospitals in the U.S. and Canada not using HOCl generators to reduce the numbers of disinfectants used?
- Why do chemical companies have such control on the disinfectant markets in North American hospitals and medical facilities?
- Do hospitals realize that they can generate HOCl on-site for pennies per quart that is 100 times more effective than bleach and is infinitely safer for people and environments?
- Do hospitals know that HOCl meets the safety, efficacy and cost decision pillars of the Association of Healthcare Value Analysis Professionals and the Association for the Health Care Environment’s Value-based Product Evaluation and Implementation certification course?
- Do hospitals know that HOCl does not leave floors sticky like quaternary ammonium compounds and is virtually odorless, emitting only a mild swimming pool smell?
HOCl is safe for staff who use it as well as for the patients and family members who are the beneficiaries of the cleaning and disinfecting process. It is safe for the health care environment and the waste stream. Finally, it is cost-effective. Indeed, a disinfectant, cleaner or cleaner/disinfectant need not be expensive to be safe and effective.
For a disinfectant to be effective, it must contact the bacteria or suspected pathogens. That means removing biofilm, dirt and dust from a surface first. Then, a disinfectant is applied using a health care grade ultra-microfiber (HGUM) wiper/cloth or mop designed to transfer sufficient disinfectant solution to the intended surface and trap and remove the organic matter (dirt, biofilm, virus and bacteria) on the surface.
Some may ask, “What about using bleach everywhere?” Even the world’s largest bleach manufacturer states that bleach is not a cleaner; it is an oxidizer and disinfectant. Bleach has its benefits, but it also has its burdens. There are risks and rewards associated with every disinfectant, and this needs to be understood by all decision-makers involved in selecting disinfectants.
Cost seems too often to be the motivating factor in environmental services (EVS) purchases, so why not use a high-quality, safe and cost-effective disinfectant? Advantages of on-site generation include:
- Improved efficiency, reducing the number of disinfectants on hand.
- Reduced training costs, with fewer chemicals to study and no solutions to mix.
- Reduced material costs, inventory challenges, chemical waste, and water use and waste disposal.
- Noncorrosive, eliminating damage to health care surfaces.
- Reduced time and labor, workman’s compensation liability due to inhalation and splash injuries, and absenteeism due to sickness.
- No supply chain issues, less reliance on disposable plastic and cardboard, and reduced machine maintenance.
- Environmentally responsible and contributes to improved indoor air quality.
- Prolongs the life of reusable HGUM mops and wipers/cloths.
- Will not damage carpets, cloth surfaces, uniforms and scrubs.
Will the on-site generation of HOCl replace every germicidal, pseudomonacidal, tuberculocidal, fungicidal and virucidal currently used in hospitals? No, and it is not intended to.
Not all disinfecting situations require a pseudomonacidal, tuberculocidal, fungicidal or virucidal, and these pathogens are not found throughout a hospital, so their use is unnecessary.
Disinfectant solutions
Multiple pathogens have developed into “superbugs,” which have developed antimicrobial resistance to antibiotic medications. Health care is experiencing the advent of many of those bugs on environmental surfaces. They have developed the capacity of existing outside of the human body for hours, days, weeks and months; the longevity on surfaces depends on the bacteria and environmental conditions.

A hypochlorous acid disinfectant and sodium hydroxide generator with a 55-gallon storage tank for each solution in a hospital EVS clean storage room.
Image courtesy of the author
With the advent of superbugs in the health care environment, professionals must be more knowledgeable about the disinfectants used to destroy them. Professionals must broaden their knowledge and education regarding efficacy. Efficacy does not equate to cost. Just as in treating maladies, expensive does not always relate to desired results.
What disinfectant solutions should be available to the EVS staff? Only those that are effective and measured.
Should a one-step cleaner/disinfectant be used, or is a two-step process more effective? What about using bleach everywhere as a germicidal, pseudomonacidal, tuberculocidal, fungicidal and virucidal? It destroys everything, doesn’t it? However, it is not needful.
Is the “shotgun” approach (use a broad-spectrum disinfectant and hope for the best) or the “rifle” approach (go after only the most pathogenic bacteria and hope for the best) most appropriate? What about dwell and kill times? What about solution percentage efficacy? Which bacteria are present in health care environments? What bacteria will visitors and staff carry and potentially transfer to a patient? Which disinfectant is the safest and most effective?
While this is not a science or chemistry class, the information perhaps will expand existing knowledge that the disinfectants accessible in health care settings are not the safest for patients, staff and the environment.
According to the EPA, disinfectants are pesticides. If a chemical or solution kills a living organism — even a solution as safe as HOCl — it is classified as a pesticide by the EPA. Many people think that because a chemical is listed as hospital grade, it is safe. However, very few disinfectants are genuinely safe for personal contact, surfaces and finishes, and the environment.
HOCl is genuinely safe. Under its Safety Data Sheet (SDS) first aid measures, it says “none required” for inhalation, skin contact, eye contact and ingestion. By contrast, the SDS and container labels for the chemicals currently used in most hospitals, including chlorines, chlorine compounds and sodium dichloroisocyanurate (NaDCC) tablets, are fraught with warnings. Many facilities prefer to use the tablets, as they are stable, but NaDCC tablet solutions are acidic, not alkaline like bleach solutions.
What should EVS or infection prevention (IP) professionals do? Budgets often dictate which disinfectants to use and, sadly, the emergence of more multidrug-resistant organisms (MDROs) require newer and, understandably, more costly and effective disinfectants. EVS and IP departments are facing a conundrum. Does IP recommend new products that they recognize will be more expensive yet more productive for EVS in eliminating MDROs from the environment, and how will EVS adjust their budgets to allow for the newer disinfectants?
Before focusing attention on multiple bacteria appearing in hospitals, the paradigm had been to use whatever disinfectant was both the cheapest and effective. This resulted in EVS departments stocking various disinfectants that were EPA-registered and hospital grade, yet pathogen-specific, such as one targeted to tuberculosis. The big question remained: What pathogens were in the environment, and how was an EVS technician to choose the appropriate disinfectant?
Some disinfectants are effective against gram-positive pathogens but not gram-negative. Many were effective against vegetative Clostridioides difficile (C. difficile) yet ineffective against its spores. Unfortunately, C. difficile spores usually appear after a patient exhibits signs of C. difficile infection, thus causing a host of other complications.
All disinfectants come with SDSs, containing everything needed to know about the chemical and resulting solution. Many disinfectants are disruptive to the skin and mucous membranes in their non-diluted form. When it comes to contact with organic matter such as blood, urine, fecal matter, vomitus, sputum, phlegm or any number of biofilms present in a health care environment, many disinfectants lose their efficacy. Couple these shortcomings with not knowing which pathogens are present, and the EVS and IP disciplines faced with the proverbial menu from which to choose each may have their own preferences.
Many disinfectants lose efficacy in solution with hard water. Wipers and mops made of cotton or other organic material have a binding effect primarily on organic fibers. Some chemicals are positively charged ions, and cotton and other natural textiles are negatively charged.
Finally, many disinfectants are not suitable for use on food-contact surfaces, so a food-safe sanitizer is required. This requirement increases the inventory cost of adding a sanitizer and increases the chances of a staff member involved in a cleaning process choosing the most convenient but not appropriate solution despite their training, to name a few concerns.
A game-changer
In May 2012, the European Journal of Clinical Microbiology & Infectious Diseases published “Electrochemically activated solutions: evidence for antimicrobial efficacy and applications in health care environments,” in which it stated: “Electrochemically activated solutions (ECAS) have been shown to have broad-spectrum antimicrobial activity and have the potential to be widely adopted within the health care environment due to low-cost raw material requirements and ease of production (either remotely or in situ). Numerous studies have found ECAS to be highly efficacious, as both a novel environmental decontaminant and a topical treatment agent (with low accompanying toxicity). However, they are still not in widespread use, particularly within the health care environment.”
EVS managers can log on to hypochlorousacid.com to search over 300 published research scientific and peer-reviewed articles on HOCl. HOCl by many manufacturers appears on EPA List N. HOCl is not the silver bullet needed to rid the world of pathogens, but it is a game-changer that is practical and worthy of investigation and use by health care professionals.
Disinfection as an EVS process
Part of the health care disinfection process must allow sufficient disinfectant time to dwell and kill potential pathogens on surfaces. This step in the process is the most overlooked and skimped due to the environmental services (EVS) technician’s requirements to turn the room over quickly.
The questions must be asked: Can nurses shorten the time and technique involved in putting a peripherally inserted central catheter? Can a pulmonologist take shortcuts when intubating a patient? Can a surgeon rush the transplantation of a heart, lung or cornea? The answer to these questions is a decided “no,” unless there is no consequence for safety and positive patient outcomes.
Patients present to hospitals with more complex underlying health care issues than ever before, including exotic and “superbug” pathogens. Health care-associated infections cost hospitals and health care systems millions of dollars in lost revenue due to reimbursement issues.
The chemicals EVS departments use, or need, to address this onslaught are limited. Budgets are strained to the point that operational compromises and staff reductions occur to absorb the ever-increasing costs of supplies. Few infection preventionists receive training to understand the chemistry involved in disinfectant decisions.
By using hypochlorous acid (HOCl), a health care organization can incorporate a different and some might say “novel” approach of an incredibly safe, effective and low-cost disinfectant into its infection prevention armory.
HOCl has been protecting the human body since its creation; EVS departments now can harness that protection to collaborate with the body in protecting it from harmful elements found in the health care environment.
John Scherberger, FAHE, CMIP, T-CHEST, T-CSCT, T-CNACC, VPEI, is president and founder of Healthcare Risk Mitigation, Spartanburg, S.C. He can be contacted via email at jfscherberger@me.com.


