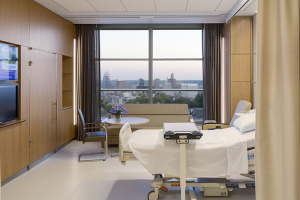
Cost-effective design
About this articleThis feature is one of a series of quarterly articles published by Health Facilities Management magazine in partnership with the American Academy of Healthcare Interior Designers. |
Evidence continues to mount that patients' and visitors' impressions of a health care facility's interiors directly relate to customer satisfaction. Specifically, surveys show that people make judgments about the quality of care they receive based on the condition of the health care environment.
The importance of cleanliness, condition of furnishings and pleasing design and colors is demonstrated by the fact that the Hospital Consumer Assessment of Healthcare Providers and Systems, commissioned by the Centers for Medicare & Medicaid Services, includes the hospital's environment as one of the key areas of its survey.
Knowing this, most facilities support and budget for attractive, welcoming environments in the planning stages. The larger challenge is keeping the spaces as attractive, functional and hospital-grade clean 10 years down the road. In most institutions, this can be more difficult to accomplish because the budget for maintenance and interior finishes and furnishings has to compete with other critical expenditures.
Limited budgets are all the more reason to plan, purchase, manage and maintain furnishings cost-effectively. By following a carefully considered plan and taking a proactive approach to interior design, health facilities professionals can take advantage of an opportunity to save money.
Smart purchasing
Considering that facilities professionals need to make decisions about a broad range of items including furniture, flooring, wall coverings, lighting and cubicle curtains, a facilities team needs a comfortable learning curve of several years. It is a huge asset in this early phase to have the input of a health care interior designer who has worked in numerous facilities and has knowledge of new products and the latest standards. Working together, the project team can identify a list of interior finishes and furnishings that merit consideration and develop a plan to research them.
It's common to ask vendors to install mock-ups a year or two before the hospital plans to purchase interior materials. This gives the facilities team the opportunity to test them in the exact conditions in which they will be used. For the sake of apples-to-apples comparisons, the team selects one type of space — exam rooms or patient rooms, for example — and furnishes each with different products. This "try before you buy" approach provides a meaningful way to experience the pros and cons of each item.
The next phase of research involves having the project team visit facilities that are using the finishes and furnishings being considered. Facilities professionals should make sure to include installations of various ages to determine durability and cleanability for short, medium and long time frames. Additionally, the maintenance or environmental services staff at each location should be asked about the cleaning procedures and schedules they follow. If the materials require frequent cleaning or time-consuming maintenance, it will add to staff time and cleaning supply requirements, which translates to higher costs.
At this point, facilities professionals can confidently eliminate from consideration any items that didn't meet the team's standards and begin to develop comparisons based on more quantitative information. Materials, interior finishes and furnishings should be evaluated for life-cycle costs, including the cost of cleaning, repairing or refinishing an item over time. For example, vinyl composition tile (VCT) has a low first cost and is a durable flooring product. The downside is that it requires frequent cleaning and buffing to keep it looking shiny. As a result, over 10 years, VCT is actually a more expensive choice than a solid vinyl tile that has a higher initial price tag but lower maintenance requirements.
Another key issue affecting the purchasing decision is the replacement schedule. Facilities professionals should aim to have resources earmarked to replace or refinish products before they look worn. The schedule needs to consider the status of all interior finishes or furnishings in a defined area so the team can avoid combining new furnishings with ones that look dated.
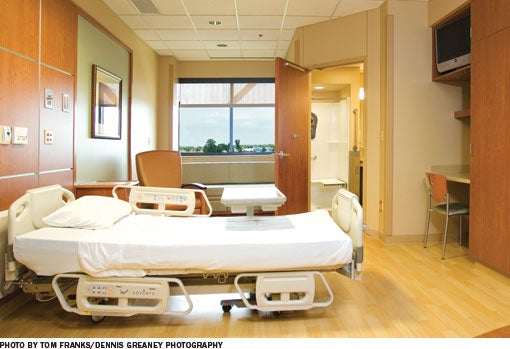
The replacement schedule also needs to take into account the facility's budget forecasts as well as plans for expansion or remodeling. For instance, if the hospital expects to expand its emergency department in five years, the facilities professional will need to consider the potential effect of that project on the area that's being furnished. Will the floors need to be torn up or will they abut a non-matching flooring material? If they will be disrupted or reconfigured, it's a waste of money to invest in something that will outlast the time they will be used. In one real-life scenario, when Mercy Willard (Ohio) Hospital designed the lobby areas in its new facility, the project team chose a carpet that was not as durable as some other options since they planned to replace it in five years.
Even if facilities professionals plan around these scheduled events, they won't be able to predict what might happen to necessitate replacing some parts of the interior environment they so carefully designed. This makes a strong case for using a neutral palette, especially for items that will be kept for the long term. It will give facilities professionals more options in finding new furnishings that coordinate with existing ones.
Finally, vendors will recommend that the facility order a certain percentage of "attic stock" to have on hand for repairs and replacement. This is a good idea, but facilities professionals should use their own judgment to determine the amount that should be kept on hand. Diane Darr, director of support services at the Bellevue (Ohio) Hospital, confirms that, oftentimes, too much attic stock is ordered. "Storing it year after year can be an inconvenience and, if not inventoried properly, it is hard to keep track of," she cautions. "As a result, it can become more of a liability than an asset." A master plan for interiors can help health facilities professionals make an accurate estimate [see sidebar, Page 32].
Installation and maintenance
Once facilities professionals have decided what to purchase, they will want to compile a broad range of information about the products. In addition to owner's manuals and maintenance instructions, facilities professionals should record contact information of their vendor or representative as well as the company's website. Clearly labeled samples of all materials and finishes should be kept. This information will become part of the facility's master plan.
One of many advantages of working with an interior designer is that he or she typically has leverage with a variety of vendors. The designer is in a position to advocate for repairs or replacement of products as well as solutions to other problems that might arise. The designer also can arrange for the vendor to conduct a lunch and learn to explain product features or recommended cleaning and maintenance regimens.
An interior design strategy that prevents damage can save on costly repairs. Some examples include:
• Taking into account the use of a space may warrant going beyond standard installation procedures. For instance, flooring under patient beds is vulnerable to cracking or delaminating. These areas hold up better if a two-part epoxy adhesive is applied on the subflooring.
• Linoleum floors are popular in health care environments. Heavy furniture such as sleeper sofas can mar the floor if they are dragged by maintenance staff for cleaning or repositioning. One creative solution to the problem is to replace the feet of sofas with lockable casters that will allow them to be moved more easily.
In these and other cases, observing and documenting how and where damage occurs can lead to devising preventive measures. High traffic and moving furniture and equipment take their toll on walls and door jambs, particularly in patient rooms. In their visits to other hospitals during the planning phase of an interior design project, the team at Mercy Willard Hospital noticed that crash rails in patient rooms did little to control some damage. Instead, they installed rigid sheet wall protection that fully protects a greater expanse of wall.
The selection process for health care interior materials often is practical and pragmatic. However, when it comes to hard flooring purchases, perception and bias play a major role. Most interior designers and environmental services managers would recommend a low-gloss, solid-vinyl floor for clinical areas. However, glossy floors provide the perception that they and their surroundings are clean. Sometimes this makes it difficult to convince hospital administration that a dull finish is a better choice.
One issue is that a glossy finish tends to attract dirt and show scuffs, so the extra expense of regular buffing is required to keep these floors looking clean. Conversely, low-gloss, solid-vinyl flooring is durable and can be cleaned with disinfectants without damaging the finish. Unlike glossy floors, there are no issues with glare, a characteristic that can affect the depth perception of people with poor eyesight, causing them to have difficulty walking. In addition, shiny floors have a tendency to be slippery when damp.
This brings up the issue of the recommended cleaning standards set by the Centers for Disease Control and Prevention and other authorities. Because of the high level of foot traffic on patient floors, hard floors are not expected to be disinfected unless they are in operating rooms. However, surfaces that are touched still regularly need to be disinfected, including door handles, faucets, bed rails, counters and an extensive list of many other interior elements.
Checking performance
Cleaning and repairs can keep health facilities professionals focused on day-to-day operations but there is a more proactive step they can take — an annual well-check. It will allow facilities professionals to anticipate maintenance issues and address problem areas while they are still simple to remedy.
Conducting an annual well-check of the interior environment is a simple process. Armed with an inventory of the furniture and materials in each room, facilities professionals merely use a numerical scale to record the condition of various aspects of each item on a form that can be entered into a spreadsheet.
The top of this checklist would provide the department and number of the room being inspected. Below that would be a grid showing interior elements such as flooring, walls, casework, ceilings and furniture with spaces for staff to rate each element's overall appearance, damage and unique characteristics on a 1 to 10 scale. Other spaces can be used to log the estimated replacement date, estimated replacement cost and maintenance concerns for each element.
Facilities professionals should schedule the first well-check a month in advance of the expiration of any warranties. This will provide time to request new materials or monetary adjustments if things are not performing as expected.
A staff member should have responsibility for scheduling the annual well-check and creating a report of all findings, including anything that needs immediate attention. Any items that are wearing faster than anticipated also should be noted so their replacement schedules can be adjusted appropriately.
Savings and quality
While it takes significant resources to create and maintain an environment that is welcoming and comfortable, cleanliness and condition of interior spaces often lead patients and visitors to anticipate a good experience.
From that perspective, interior design elements are a valid business investment, even though interior finishes often are more vulnerable to budget cuts than items more directly related to patient care.
Many of the suggestions presented can be implemented immediately at a relatively modest cost. Other than time from staff or an interior designer, they also don't require training or new technology.
If facilities professionals focus on making purchasing decisions based on overall facility needs and are proactive with maintenance, an interior design program will aid efforts to save money and still deliver the spaces that patients and visitors associate with exceptional care.
Lynne Gochenour, IIDA, AAHID, LEED AP, is a senior interior designer and senior associate at SSOE Group's Toledo, Ohio, office. She can be reached at lynne.gochenour@ssoe.com.
| Sidebar - Creating a master plan for interiors |
| An interior design master plan acts as the repository of all plans, information and reports related to the facility's interior elements. Creating an electronic or print go-to space where anyone can find all the data related to interiors is essential to the effective functioning of a health care facility. It also will be extremely helpful in training new staff members. The master plan should feature: • As-built drawings. These should include architectural and engineering construction documents. • The replacement schedule. This is essential to the budgeting process and should include a 10-year forecast. It also should be updated at least annually. • Maintenance instructions. These should be organized by item type and include a picture of the product or a clear definition of the area to which it applies. • Product information. These include warranties, vendors, history of purchase or repair, assembly instructions and swatches, if applicable. • Inventory of attic stock. This should tell what the attic stock is for, its quantity and where it can be found within the storage space. • Annual well-check reports. These can be kept on paper or in a spreadsheet software program. Whether assembling and updating the information is the job of the facilities manager, interior designer or some other individual, the responsibility for the tasks should be clearly spelled out. |