Clean design

When a patient develops a health care-associated infection (HAI), it is often difficult to determine where it originated. It could be from ambient air, countertops, water faucets, privacy curtains, bed rails, direct hand contact or any combination of these.
This has elevated the importance of the design professional's role in mitigating these events through material specification, planning and engineering. In fact, the interior designer often is required to navigate between departments such as environmental services and infection control to help determine the most appropriate solutions.
Environmental factors
Disease-causing pathogens can survive on objects for extended periods of time, often months. In contact transmission, transfer of pathogens to the patient can occur in two ways. The first occurs via the direct contact of a patient with a contaminated surface. The second is through the direct contact of the caregiver with a contaminated surface and then with the patient.
Sources of surface contamination can be ranked from those that are frequently touched by caregivers and patients to those that are rarely touched. Some typical "high-touch" surfaces include overbed tables, light switches, telephones, grab bars, door handles, bed rails, medical equipment, toilets, sinks, privacy curtains and patient chairs.
The system often breaks down in practice. Cleaning a typical private medical-surgical patient room can require 30 to 60 minutes; and intensive care unit rooms require roughly 45 minutes. Due to high census numbers in many health care facilities, the actual available time to clean a room between patients may be far less. In a busy emergency department, for example, the amount of time scheduled for cleaning may be 8 minutes and contingent upon whether the cleaning staff can access the room between patients.
Overall, the most effective infection prevention measure is through proper hand hygiene.
Design implications
The movement toward single-occupancy patient rooms is an important step in reducing infectious disease transmission. The ability to keep patients physically separated from each other allows for infectious conditions to remain within each particular patient environment.
Within the room itself, the location and design of the sink area is a key factor. Properly designed hand-washing sinks should be located at least 36 inches away from patients and clean supplies or they should be equipped with splash guards to avoid splash contamination. The sink must be deep enough to allow for proper hand-washing techniques. Placement near the entry door is optimal.
Location of sharps containers, glove boxes and alcohol-based, hand-cleaning dispensers should be considered in the overall design of the room and should be in accordance with Centers for Disease Control and Prevention (CDC) guidelines. Involvement of the hospital's infection control specialist is important in arriving at the optimal solution.
In all inpatient environments, personal protective equipment such as masks, gowns and eye protection should be provided outside the patient room in a location that is convenient yet out of the way. A means of indicating when personal protection is required should be placed outside the room.
| Lower Left: For the new patient tower at Advocate Lutheran General Hospital, Park Ridge, Ill., mock-up rooms were used to determine the best location for the hand-washing sink, privacy curtain configuration and the finishes in the sink area. | Lower Right: The design for Advocate Lutheran General's patient care tower incorporates one personal protection supply storage cabinet for every four patient rooms in an unobtrusive yet convenient location outside the rooms. |
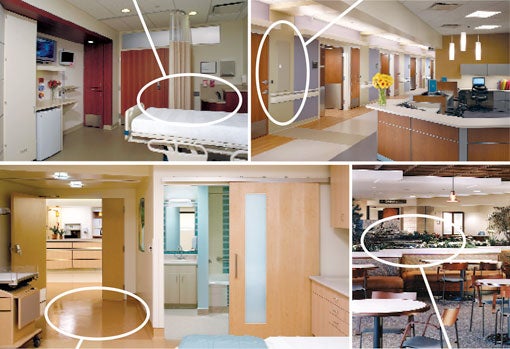 | |
| Upper Left: The high-risk birthing rooms at Banner Good Samaritan Regional Medical Center in Phoenix were designed with seamless flooring material and an integral cove base to facilitate cleaning. | Upper Right: Regular maintenance and testing is conducted to ensure that no infectious microorganisms exist in a water feature designed for the public area of Arlington Heights, Ill.-based Northwest Community Hospital's North Pavilion. It is one of four water features successfully implemented on campus. |
Transmission types
Each type of infection transmission presents its own challenges to the hospital interior design team. Advice on answering these challenges includes the following:
Surface transmission. The evidence doesn't yet exist to prove that surface materials alone directly contribute to contamination. Thus, it is incorrect to say that changing only one component of the built environment will have an impact. A more comprehensive approach is called for that considers the design of all of the high-touch surfaces.
Transmission of Clostridium difficile (C. difficile) via contact is a high concern related to surface materials because it is very easily transmitted through contact. Given that it is resistant to routine cleaning measures, 10 percent bleach-based cleaners have resurfaced as the most commonly used and most effective disinfectant measure against C. difficile. However, there are limited materials that can withstand the use of bleach cleaning methods.
Because patients and caregivers come in direct contact with furniture arms, backs and upholstery, it is possible to transmit pathogens this way. Many types of disinfectant products can damage wood frames and certain upholstery fabrics. Thus, design professionals must understand the specifics of the cleaning products and methods being used to properly specify the furniture and upholstery products.
Fortunately, there are more patient room furnishings that can stand up to rigorous cleaning than there have been in the past.
Privacy curtains are frequently touched by caregivers and thus can become contaminated, particularly at the edges. Curtains are not always cleaned until they are visibly soiled. The location of the privacy curtain relative to the hand-washing sink and gloves can mitigate contamination by touching to a degree. Often, the curtain configuration is based upon solving patient privacy needs alone. Understanding the sequence of activities caregivers typically engage in after washing their hands and putting on gloves will assist in determining the configuration and placement of the privacy curtain.
Wall surfaces adjacent to sinks and toilets also are likely to become contaminated. Typical finish choices for these locations include solid surface materials, ceramic tile and scrubbable paint. However, in many health care facilities, the environmental services staff is unable to keep the grout joints of ceramic tile or textured wall finishes properly cleaned. Likewise, painted surfaces may not be able to withstand the harsh cleaners used. In general, these surfaces must be smooth, nonporous and water-resistant.
Countertop surfaces adjacent to wet areas, such as hand-washing sinks, require particular attention. Because these are subject to nearly constant contact with water, they can become a source of bacterial growth. This would include the countertop as well as the adjacent wall surfaces. Wall surfaces also are subject to damage from most antibacterial hand soaps. Seamless, water-resistant materials are warranted in such areas.
Wall finishes in patient care areas should be smooth, fissure free and able to withstand harsh cleaning agents. The substrate under vinyl wallcovering has been the source of mold growth in moist environments and the textured surfaces used in many wallcoverings are difficult to clean effectively. As a result, vinyl wallcovering should be considered carefully.
In addition, the detailing in wall and ceiling architectural elements should be evaluated carefully, with consideration given to patient acuity levels. Ledges or reveals that create places for dust to accumulate can be problematic for immunocompromised patients.
Floor surfaces typically come under considerable scrutiny in health facilities. Hard-surface flooring must have the ability to withstand harsh disinfectants and motorized cleaning equipment. Seamless flooring is often used to eliminate the collection of dirt in seams between tiles or between the flooring and the wall base.
Flooring installers must be properly qualified to install welded seams and integral cove bases. Often, poor installation can lead to joints that are not smooth and are difficult for environmental services to keep clean. Visible indicators of cleanliness, such as shininess, are a poor gauge yet often become the focus.
The debate over the use of carpet in health care settings continues. Carpet designed for these environments has been engineered to prevent moisture from being absorbed into the slab and to prevent odors that are often associated with "hospital smell." The stain resistance of carpet has greatly improved and many carpets are cleanable with bleach-based solutions.
The advantages of carpet include improved acoustics and underfoot comfort, as well as a more hospitality-like aesthetic. However, carpet is more resistant to rolling loads and has a shorter lifespan than hard-surface flooring. While some studies find that carpet can harbor bacteria, there are many other studies reporting that carpet does not contribute to HAIs. Because there is very little direct contact by individuals with the floor, it is an unlikely source of transmission.
Airborne transmission. Hospital construction, renovation and maintenance have been linked to outbreaks of mold infections. Interior design professionals, hospital facilities staff and contractors need to take measures to proactively minimize dust associated with construction activities and, most importantly, prevent dust infiltration into patient care areas. Even simple inspections that involve the removal of ceiling tiles and touch-up painting or the replacement of light fixtures can contribute to the spread of mold spores.
Activities that involve sanding walls, new wall construction, minor duct work, removal of floor coverings or any fixed building component create the potential for the spread of infection. For even minor renovation work, interior designers should advise clients to implement the proper infection control precautions.
There also is some potential risk associated with routine carpet vacuuming. Unprotected vacuuming can force dust and microorganisms into the air, creating a risk for immunocompromised patients in particular. Carpet should be limited in these areas.
Other sources of airborne transmission can occur from the malfunction or contamination of ventilation systems. Hospital ventilation systems that are not properly cleaned, operated or designed can become sources of dust and moisture, increasing the risk of transmission of fungal spores and bacteria. For immunocompromised patients, this is of particular concern. High-efficiency particulate air (HEPA) filtration systems are recommended in all health facilities and, in particular, areas being renovated.
Waterborne transmission. Fixtures such as showers, sinks and toilets can become reservoirs for Legionella. Regular cleaning and disinfection of faucet aerators is recommended to help prevent and control Legionella.
Additionally, the design of the hand-washing sink basin has an impact on the amount of spray generated when a person is washing their hands. The manner in which the water from the faucet hits the drain should be carefully considered. The potential for contaminates to spray onto the face of the person washing their hands must be eliminated.
Water features are often a topic of debate among infection control specialists and other health facilities professionals. While the CDC does not believe that decorative water features pose a risk of spreading infection, there are many design and maintenance precautions that must be addressed.
Certainly, the risk level of the patient environment is paramount. The design of the water feature can either increase or limit the level of aerosolized liquids present and an effective water treatment system must be in place.
Institutional not an option
While some may conclude that reverting to sterile, institutional environments is the only way to handle HAI concerns, that would be a disservice to those who are in the hospital to heal, work or visit.
Instead, the problem of HAIs requires a strategic approach using a collaborative team that includes interior designers, infection control professionals and environmental services managers reviewing a variety of methods and technologies.
With today's product and material advances, the opportunities to create environments that are safe and easily maintained, yet still appear patient-focused, readily exist.
Jocelyn M. Stroupe, IIDA, AAHID, EDAC, is principal at Cannon Design, Chicago, and president of the American Academy of Healthcare Interior Designers. She can be reached at jstroupe@cannondesign.com.
| Sidebar - New FGI Guidelines address HAI concerns |
| The much anticipated 2010 Guidelines for Design and Construction of Health Care Facilities addresses many needs in mitigating the spread of health care-associated infections (HAIs) through design and materials. For example, specific dimensions and materials for hand-washing sinks are defined, as well as materials for adjacent countertop surfaces and substrates. The area of the basin is recommended to be not less than 144 square inches with a minimum 9-inch width or length. Basin and countertop materials are to be porcelain, stainless steel or solid surface. Plastic laminate will be allowed as long as the substrate is marine-grade plywood. The discharge point for the faucet shall be at least 10 inches above the bottom of the basin and water pressure should be regulated. Recommendations for the number of hand-washing sinks for placement in infusion therapy as well as fast track and pediatric services in the emergency department are included. Ambulatory facilities will be expected to meet similar guidelines as acute care facilities in terms of hand-washing sinks and material selection. Special patient populations, such as oncology, pediatrics and bone marrow transplant, are specifically addressed with requirements for HVAC and material usage. For oncology units, light coves or other areas that collect dust should not be used. For pediatric oncology units, playrooms should be designed with easily cleanable surfaces. In bone marrow transplant units, sealed windows are recommended to prevent infiltration from the outside. An infection control risk assessment (ICRA) is called for in the specification and selection of furniture and equipment in hospital settings. An ICRA should be employed to determine the number of airborne infection isolation rooms for cancer treatment and infusion therapy areas. The guidelines also devote considerable attention to the area of acoustics in health care. This will present additional challenges for design professionals in that acoustical materials may be at odds with cleanable surfaces. |
| Sidebar - New technology hype and reality |
| There is considerable marketplace buzz about new interior finish technologies such as antimicrobials, metals and nanotechnology. Following is a look at the hype and reality of these materials:
|



