Medical equipment maintenance
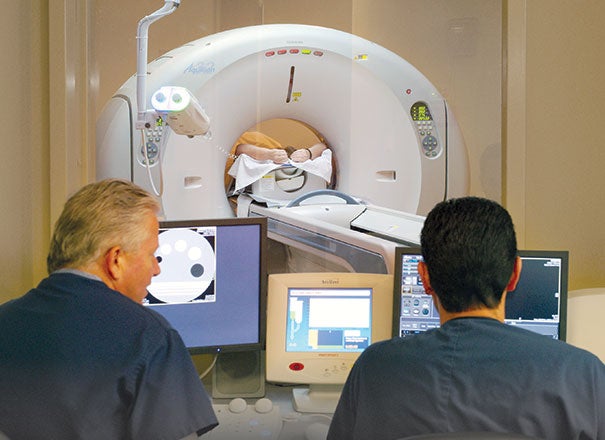 |
| PHOTO BY VALERIE LAKTASH While most imaging equipment work is outsourced due to its specialization and sophistication, it is still the biomedical engineer’s responsibility to ensure that the work is performed in a timely manner by a qualified contractor. |
The management of medical devices has taken on a new level of complexity in recent years, due in part to the increased sophistication and specialization of equipment, integration with electronic networks, dependence on outsourcing for specialized maintenance and repair, and ever-increasing requirements for compliance, safety, reliability and accuracy.
All of these issues need to be addressed while maintaining an equipment inventory capable of providing the right equipment at the right time for the right application.
By using medical equipment historical data and conducting an equipment audit, health facilities professionals can analyze the techniques they are using in their management programs as well as improve efficiency and compliance while decreasing costs.
Baselines and methodologies
Before starting, it is important for health facilities professionals to establish a baseline. Because facilities are different sizes and utilize different levels of technology, dollars spent is not an accurate comparison. Rather, professionals should calculate their biomedical equipment program’s cost of service (COS) ratio.
Ted Cohen, clinical engineering manager at UC Davis Medical Center, Sacramento, Calif., developed the COS ratio to determine the financial effectiveness of a biomedical maintenance program. There are other benchmarking models, but the COS ratio takes into account the technology and the cost to maintain it, which is represented by the higher acquisition cost compared with the total spent.
The COS ratio is calculated by dividing the total annual cost of operating the medical equipment program (labor hours, parts, repairs and external contracts) by the value (initial acquisition cost) of the medical equipment in the inventory. In Cohen’s 2007 benchmarking series for the Association for the Advancement of Medical Instrumentation’s Biomedical Instrumentation & Technology journal, he stated that the COS ratio in the United States is between 5 and 10 percent, which excludes outliers. A facility’s COS ratio compared against its established goal provides direction on how many ideas can be considered when attempting to reduce costs and increase efficiency.
Medical equipment management programs (MEMPs) have been around for more than 25 years, and most hospitals have gone from a fix-it-when-it-is-broken inspection and maintenance program to one that is time-based, then predictive, then condition-based, and, finally, to one that is risk-based. Preventive and corrective maintenance are mostly concerned with frequency-scheduled activities as well as repairs after the equipment is out of service; they miss opportunities for optimization, including the ability to set maintenance intervals based on meaningful data.
Some of the newer equipment management models include input into more categories that yield valuable data and that can increase medical equipment reliability and reduce maintenance costs. These fields include “corrective,” “preventive,” “criticality factor,” “failures,” “condition analysis,” “reliability factor” and “predictive services” types of work performed. By inputting executed maintenance or repair into these subcategories, valuable data can be obtained on mean run time before failure, age-related repair costs, the type of equipment that is out of service most often and the average duration. Add this to the risk value and patient outcomes, and results will increase efficiency by providing optimal observation times, decrease failure rates and allow for replacement planning ahead of emergency situations.
Analyzing a program
There always will be a place for routine preventive maintenance but many hospitals perform both corrective and preventive maintenance with very little predictive or reliability-centered maintenance.
Which additional data fields will provide an organization with information it needs to improve efficiency and reduce failures? Have there been any equipment-related patient outcomes? If so, is there a place in the equipment record and a process to track these by function of equipment, manufacturer, risk category, age of equipment or utilization? Each organization needs to decide which data fields will contribute to the goal it seeks. The biomedical engineer knows which equipment actually breaks, which causes the most user errors, and on which he or she performs preventive maintenance that has never needed calibration or repair. Facilities professionals should start by asking where time seems to be wasted or what equipment fails the most and focus the initial improvements in those categories.
For each category, professionals should identify the current process, the new process, steps to achieve the new process, expected outcomes and revisit the process as much as necessary to achieve the expected outcomes.
This extra input and reorganization can seem daunting. However, most of this information is already being entered into the maintenance database, but may be not entered into fields that link together. Other information only has to be entered once, such as planned operational time, which is obtained from a national database. Facilities professionals should work with their information technology staff to set up links that will enable beneficial reporting. If the organization has a maintenance program purchased from a vendor, ask for programming and training support.
This can be as easy as taking one item or group to try to accomplish one goal. For example, most hospitals track the number of user errors on patient-controlled analgesia machines (PCAs). This information can be expanded from the standard number of user errors to include the ability to report on user errors by department, shift, employee and PCA make or model.
This can help to identify if further education is needed on a particular shift, by a particular PCA model, or perhaps just for an individual. Most of the time spent documenting equipment performance and maintenance is in opening the program and searching for the record; the input user name, department or shift fields take seconds, especially if drop-down menus are utilized. If the data output is not exactly what is needed, the process can be revisited and fields added or deleted as needed.
Performing an inventory
The ability to use use such data requires conducting a complete inventory of biomedical equipment in the facility.
If a facilities professional doesn’t have time to do the entire inventory process at once, he or she can break up the process by categories over a year’s time. Categories can include equipment with outsourced service contracts, imaging equipment, equipment integrated with information technology (IT) networks, equipment by risk or department, or by any other groupings that have a common association.
This inventory needs to be as comprehensive as possible. Aside from such obvious information as manufacturer and asset number, fields to consider include function, mission criticality, utilization, availability of alternate devices, failure frequency, detectability, failure consequence, operational consequence, downtime, repair cost, repair criticality, recalls, manufacturer guidelines, type of maintenance (preventive, corrective, predictive, emergency or condition-based), planned operational time, whether the maintenance is outsourced, number of user errors, number of "cannot duplicate" and IT integration values.
The ability to export the database to a spreadsheet improves the process by allowing added fields and easy sorting and analysis.
Working information
Whether health care facilities professionals have performed a complete equipment audit or are planning it by category, the information can be put to work for organizations in a number of ways. They include:
Increased efficiency. Even if an in-depth biomedical equipment audit is still underway, there probably is a list of the total equipment at the facility.
The equipment list can be sorted by department. Each department director can be emailed a list of equipment assigned to his or her cost center, making sure to copy anybody else who has knowledge of what is being utilized. In addition, the list should be sent to central supply employees for any equipment they might clean or store. They know how often equipment is utilized and what, if any, equipment is not being used. By far, the easiest way to eliminate labor hours is to eliminate the maintenance on equipment that is not being utilized.
Another reason for sending each department a list of equipment being utilized in its area is because departmental employees are responsible for point-of-use maintenance, a factor most front-line staff either forget or neglect. Most equipment should be wiped down daily when in use, and a visual check performed on all fittings and accessories. It is important for clinical users to understand the reason and function of the equipment to an extent that they can be alert to changes in the equipment and call the biomedical engineer in time to preclude any safety concerns.
Equipment replacement. Newer equipment often comes with increased efficiency by enabling data collection, providing additional quality through reduced exposure or additionally captured data.
These things can increase throughput, support high-quality decision-making, and drive efficiency and productivity. Some manufacturers offer upgrades or support to help bridge the gap between older and newer generations of equipment. However, the technology of the older equipment eventually becomes obsolete or may no longer be supported by the manufacturer. Even if the parts are still available, they may be so expensive that the unit is no longer economical to repair. Older equipment also involves a higher risk of failure or malfunction.
Facilities professionals should work with their administrative and purchasing teams to develop a replacement plan. Some facilities benefit by having specific guidelines, such as 60 percent of equipment less than five years old, 30 percent of equipment between six and 10 years old, and 10 percent greater than 10 years old. For progressive facilities, 10 percent of equipment older than 10 years is unacceptable due to the rapid pace at which technology for biomedical equipment is progressing. These general guidelines also can be modified based on risk, current repair data or reliance on IT integrated information.
Outsourcing. Once a complete and accurate inventory of biomedical equipment has been assembled, a report that lists all outsourced equipment should be produced.
This means that outside vendors are brought on-site to perform preventive maintenance or repairs on specialized pieces of equipment. Most health care facilities are co-sourced. Even if they normally contract biomedical engineers on-site, they also hire specialized biomedical engineers for some specialized or sophisticated equipment, such as magnetic resonance imaging and positron emission tomography.
If the facility is part of a larger health system, facilities professionals should investigate whether synergy can be achieved by sharing resources. While a full-time imaging maintenance technician might not be economically beneficial at a single location, for instance, it might save money for multiple facilities when utilized as a shared resource. If this is impractical, facilities professionals can look at the ability of a single outsourced vendor to perform maintenance and repair on all specialized equipment for a discounted rate.
The biomedical engineer or manager needs to be included in all equipment acquisitions. He or she needs to speak up about proprietary parts issues, or about the reliability of one brand over another. At minimum, facilities professionals should see if their maintenance contracts can be renegotiated to reduce costs.
Informatics. If a facility is small, a contract might be needed for biomedical informatics, which is a hybrid of biomedical equipment and information technology.
As the electronic health record (EHR) continues to evolve, so will the interface capabilities between the biomedical equipment and the patient’s EHR. Without proper training or a biomedical informatics contract, medical equipment with an IT interface can be shuffled back and forth between the biomedical engineer and the informatics technician. The costs of downtime are many, with the unavailability of required equipment needed for patients being an unquantifiable cost.
Maintenance frequency. In December 2013, the Centers for Medicare & Medicaid Services issued memorandum S&C 14-07-Hospital, stating that facilities could use an alternative equipment management (AEM) plan. The exceptions to the AEM include critical or high-risk equipment, imaging/radiologic equipment, medical laser devices or new equipment for which sufficient maintenance history is unavailable. For these exceptions, testing must follow manufacturers’ guidelines; for all other equipment, an increase in the preventive maintenance intervals is allowed if analysis and documentation illustrate the rationale for the decisions.
Reducing the frequency of preventive maintenance not only reduces labor hours, but can move a facility from preventive maintenance to predictive or reliability-centered maintenance. In addition to labor hours saved, moving to predictive or reliability-centered maintenance will prevent equipment failure, optimize reliability and save costs.
Running reports by equipment device, model or function is the most efficient way to assess preventive maintenance intervals. Facilities professionals should look at the mean time between diagnostic adjustment or repair and the mean time before failure. Most facilities will be able to capture significant labor-hour savings by implementing an AEM on low-risk equipment.
Running these reports by manufacturer also will have an additional benefit — the biomedical engineer will have the documentation necessary to explain to the administrative or purchasing team why to continue or discontinue purchasing certain equipment.
Finding user errors. Most health care facilities will have “user error” or “cannot duplicate” on their monthly reports. Facilities professionals should run a report on their inventory by these categories to identify trends by equipment or department, shift or user. If the issue repeats for certain manufacturers or models, there are typically three reasons: device design, the ambient environment or user characteristics.
Design is more than simply how something is made; it also influences the user’s ability to understand and utilize the equipment. There are visual and tactile considerations on all equipment and often auditory considerations as well. If there seems to be a predominance of one manufacturer or model of equipment that has more user errors, it is probably a function of design.
The environment can result in user errors, especially when lighting is poor at night or when noise levels are elevated during the day. Training staff on the proper use of the equipment will continue to result in user errors if the environmental conditions are not taken into consideration. If there are no discernable trends and user errors still occur, it is most likely due to user characteristics. Are the staff familiar with the equipment? Had the staff with the user errors been working overtime or under a heavy workload? Did a staff member float to another department, or was it a temporary employee? These are all training issues that the department director can address with staff.
Savings and efficiency
Almost every health care facility can find savings and increase efficiency by performing a complete biomedical equipment inventory audit and inputting pertinent data to establish a complete database.
The reports generated from a comprehensive database can illustrate where service contracts can be modified to reduce costs, how to reduce repair costs and downtime by performing maintenance before failure, and show trends in user errors to preclude adverse events.
Facilities professionals also will be able to apply quantitative data to support short- and long-term strategic equipment planning.
Valerie Laktash, CHFM, is director of facility services at Placentia-Linda Hospital in Placentia, Calif. She can be reached at valerie.laktash@tenethealth.com.




