Tech talk: Alarm fatigue, a real-time HCAHPS predictor and smart eyewear
Researchers awake to the issue of alarm fatigue
An interdisciplinary team of researchers at the University of California San Francisco (UCSF) are in the beginning stages of what they call a super alarm, to help combat alarm fatigue among clinicians.
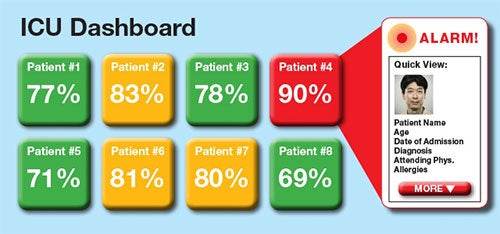
Researchers are working on a smarter clinical alarm to prevent false alerts.
The team is led by biomedical engineer and associate professor Xiao Hu; Michele Pelter, critical care nurse who leads the school’s ECG Monitoring Research Lab; and Richard Fidler, an adjunct professor in the UCSF School of Nursing. Their work on this new super alarm was spurred by the results of a UCSF study that found that there were 187 audible alarms per bed per day in its intensive care unit, with a false-positive rate of more than 88 percent for arrhythmia alarms. Those alarms also happen within the context of a larger environment with other types of noise, further exacerbating the issue.
UCSF’s researchers are developing a device to aggregate disparate data, capture trending patterns and filter out false alarms. Its first iteration of the alarm shows that it can predict Code Blue cases hours ahead of time with reasonable accuracy.
The team’s leaders remark that the unique skills of each member is what will make this project successful. They’ve dubbed it an alliance “between nurses and nerds.”
“As clinicians, we need computer geeks, because they present possibilities we would never have considered — a lab value that at first we may think nothing of, but in combination with an electrocardiography rhythm, may matter,” Fidler told the school’s publication, Science of Caring. “And they need us, because we’ll ask, 'Why can't we capture certain measures that we know are clinically important?”
Real-time HCAHPS scores at the bedside
A new platform to measure patient satisfaction recently has launched following trials at several hospitals. The EveryPatient platform brings HCAHPS into real time with patient feedback occurring in a systemized manner at the patient bedside.
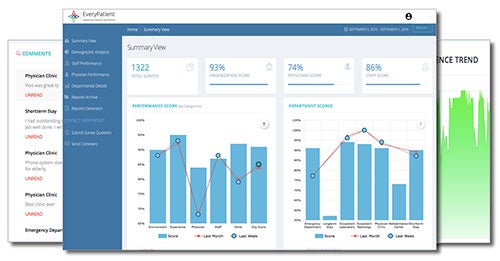
The EveryPatient dashboard allows leaders to monitor patient feedback in real time.
A proprietary survey and algorithm acts as a predictor for HCAHPS scoring based on the Centers for Medicare & Medicaid Services' scoring method. It also allows health care leaders to assess patient satisfaction levels and address issues with the patient at the point of care. The software can break down satisfaction levels at the organizational, departmental and individual levels, and programmed alerts can notify the hospital when scores are at risk of falling below a particular threshold.
During its trial period, EveryPatient was placed in patient-facing departments, such as emergency rooms, radiology, laboratory, etc. Staff offered tablets to every patient capable of filling out the customized, proprietary 15-question survey. The tablets are fitted with an audio and voice-to-comment function to assist with visually, literacy and hearing impaired patients. Collecting responses at the point of care resulted in more than 80 percent of patients completing the survey, while post-discharge patient surveys hovered at 15 percent.
Akindele Majekodunmi, M.D., MBA, co-founder and CEO of EveryPatient says that the continuous data collection the platform provides has helped its clients imporve its HCAHPS scores more effectively.
“Our clients are breaking records when benchmarked against other hospitals nationally, we now have clients that are scoring 100 percent in HCAHPS metrics, this has never been heard of before and we are really proud of this as it validates our technology,” Majekodunmi says.
Eyewear brings clarity to doctors and patients
The Center for Body Computing at the University of Southern California has teamed with VSP Global for an academic study of the pilot version of a new tech-embedded eyewear called Level.

The Level frames were named for famous inventors Nikola Tesla, Marvin Minsky and Hedy Lamarr
Participants will receive a Level frame and accompanying smartphone app that will allow them to track physical activity throughout the day. The current prototype is embedded with a gyroscope, accelerometer and magnetometer that tracks the wearer’s steps, calories burned and activity time.
“Our partnership with VSP Global will accelerate research and discovery as to how to create digital health products and experiences that will elevate, enhance and expand the lives of users,” says Center for Body Computing founder and executive director Leslie Saxon, M.D. “This study is the first of its kind and will provide a crucial road map for validating future products and platforms and for understanding overall consumer health engagement.”




