Making technology talk beyond hospital walls
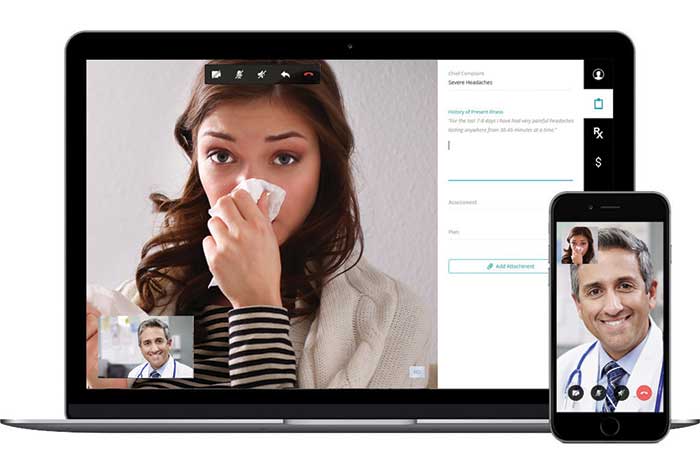
MedStar’s eVisit project enhances connections among providers, patients and medical data.
When Kaiser Permanente, Oakland, Calif., last year announced that more than half of its patient interactions were performed virtually through video visits, telephone and secure messaging, it confirmed a move toward remote health care delivery that has quickly gained adherents in health care organizations throughout the field.

|
2017 Trends: Infrastructure |
| Previous: High-touch technology |
| Next: Collaborative planning |
|
|
Although the desire to treat patients in the most appropriate and convenient setting is driving much of this growth, David Brennan, director of telehealth initiatives for the MedStar Institute for Innovation at Medstar Health, Columbia, Md., also credits reduced equipment costs.
“The infrastructure you need to do videoconferencing has fallen exponentially in the past decade or so,” he says. “We’ve moved beyond carts and dedicated hardware and can now easily scale up video on mobile devices, which gives us a lot of flexibility.”
In fact, MedStar last month rolled out its eVisit service with a free, downloadable app for smartphones and tablets or through a secure computer portal. Operating in partnership with at a Boston-based telehealth company called American Well, these “virtual house calls” are effective in treating common conditions, like mild flulike symptoms, coughs and colds, skin rashes, pink eye, allergies and known urinary tract or yeast infections.
The eVisit program is the latest in a range of MedStar projects to enhance connections among providers, patients and medical data with mobile messaging, secure image-capture apps and interactive patient education tools. Some of the organization’s earliest work in this area established video-based teleconsult programs to expand access across the system to clinical expertise such as stroke specialists, neurologists and medical ethicists.
Overall, Brennan divides such projects into three “flavors” — teleconsults among health care professionals; virtual visits with patients at kiosks, home or work, or in mobile vans; and remote care management that moves information via sensors and patient-reported outcomes.
The last of these projects can sometimes have the most complicated infrastructures.
For example, researchers at Peoria, Ill.-based OSF HealthCare’s Jump Trading Education & Simulation Center studied wired and wireless equipment for home-based monitoring of congestive heart failure (CHF) and chronic obstructive pulmonary disease as well as a device that monitors falls in Parkinson’s patients in partnership with Intel Corp.’s Care Innovations LLC subsidiary.
“The CHF study is looking at home-sensing technology used with basic telemonitoring systems that assess patients’ weight, blood pressure, heart rate and oxygen levels to study if the combined data can predict disease worsening,” explains Kimberly Cooley, R.N., CCRC, research nurse coordinator at OSF Healthcare System. “So, when they're discharged from the hospital, they put that equipment in the home and those readings are transmitted daily to a home care nurse who can monitor how that patient is doing. We are trying to come up with ways to alert clinicians that the patient’s health is declining so we can intervene early to keep them out of the hospital.”
As part of the study, researchers are introducing activity sensors placed in a patient's bathroom, a common area such as a living room or family room, on the patient’s bed, and placed on an appliance that is used frequently, such as an oxygen concentrator, nebulizer, microwave oven or lamp.
The move beyond hospital walls and into patient homes will continue to depend on increasingly flexible and innovative technology infrastructures.




