Technology goes high-touch in the patient environment
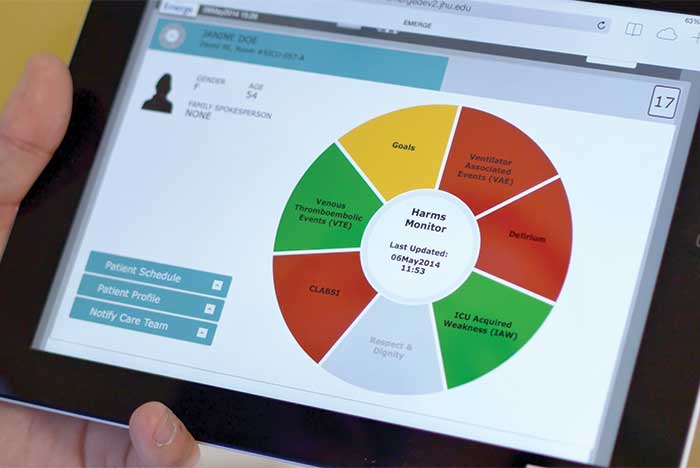
Project Emerge centralizes intensive care unit data and checklists on a clinician tablet app.
As improved patient satisfaction and streamlined patient flow become increasingly important priorities for health care organizations, they’re more often turning to technology to bridge the gap caused by tight budgets and staffing.

|
2017 Trends: Infrastructure |
| Previous: New infrastructure ideas |
| Next: Breaking communication barriers |
|
|
Thomas Jefferson University Hospitals, Philadelphia, for instance, is planning in mid-2017 to launch “cognitive” hospital rooms connected to the IBM Watson Internet of Things (IoT) platform to enhance the patient experience.
The system will provide in-room speakers that allow patients to take control of their hospital stay and overall experience by using a clicker and voice commands to operate lights and window blinds, ask questions about hospital facilities or even get background information on their physicians.
Eventually, the room will learn some of the patients’ preferences, says Neil Gomes, vice president for technology innovation and consumer experience at Thomas Jefferson University and Jefferson Health. Gomes says the goal initially will be to set the system up in about 10 rooms, then expand it to 50, and then 100.
In addition to lighting, a building automation system (BAS) connection will allow patients to audibly control their room temperature. “We have connected systems that we've installed in the room,” Gomes says. “We're not yet connected to the Siemens BAS, but Siemens is working with us to connect the two systems together.”
Elimination of the common causes of preventable problems and integration of data were the basis of another research initiative called “Project Emerge” at Baltimore-based Johns Hopkins’ Armstrong Institute for Patient Safety and Quality in partnership with Hopkins’ University Applied Physics Laboratory (APL).
“The Armstrong Institute and APL started having some conversations about the work APL was doing in systems engineering and there was an immediate recognition that health care isn't really engineered like a system,” says Alan Ravitz, chief engineer of the national health mission area for APL. “And we thought maybe we could apply the principles of systems engineering to the health care domain.”
Using a systems-engineering approach, the project centralized intensive care unit (ICU) data and checklists on a clinician tablet app and added a patient and family app to empower patients and families to communicate with the medical care team, provide details about their care goals and to learn more about the machines and monitors in the ICU room.
Perhaps the ultimate example of high-touch technology has been the growth of wearable sensors.
“Wearable sensors are an exploding health care technology both in acute and chronic care settings,” says Robert Maliff, director of the applied solutions group, ECRI Institute. “As health systems become integrated with patient care wherever it occurs, hospitals will be deploying remote patient monitoring systems, and using wearable sensors to make sure that their patients are following care regimens and [that their] conditions are not deteriorating.”
Maliff is quick to point out, however, that hospitals will need to figure out how to fund these programs as well as how to manage the data the sensors generate. Such challenges undoubtedly will be a constant in health care’s new high-tech, high-touch environment.




