FGI lays out telemedicine guidelines
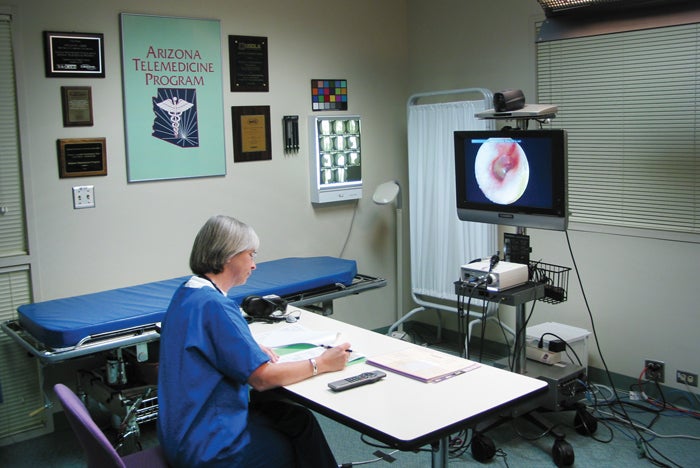
Telemedicine is included as part of the common elements for both hospitals and outpatient facilities in the 2018 Guidelines.
Image courtesy of Arizona telemedicine program
Telemedicine use rose from 54 percent in 2014 to 71 percent in 2017, according to a survey conducted by the Healthcare Information and Management Systems Society’s HIMSS Analytics, and a February 2018 post by the Patient Safety & Quality Healthcare journal indicates that as of 2017, all 50 states have adopted some form of telemedicine reimbursement coverage.
Nonetheless, many questions and inconsistencies still arise in discussions of telemedicine, including how to define the term. The Health Resources & Services Administration (HRSA) defines telehealth as “the use of electronic information and telecommunication technologies to support and promote long-distance clinical health care, patient and professional health-related education, public health and health administration.”
The Centers for Medicare & Medicaid Services uses the HRSA definition and the terms “telehealth” and “telemedicine” interchangeably. However, in announcing the HIMSS 2017 survey results, KPMG LLP suggested a differentiation. Telehealth connects clinicians with patients in their home or via mobile devices, while telemedicine connects primary care or emergency department clinicians to medical specialists via technology.
While there is no shortage of technology — from two-way videos to smartphones — the distinction that telemedicine is more than a home visit via mobile device is important when it comes to designing environments to support these services. There is an inherent difference between connecting via FaceTime with a primary care provider when a patient has a cold versus coordinating patient care with specialists in another location for patients located in underserved areas or where it might be better to avoid unnecessary patient transfers.
A proactive approach
The Facility Guidelines Institute (FGI) Health Guidelines Revision Committee (HGRC) took a proactive approach to design for telemedicine in the 2018 Guidelines for Design and Construction documents for hospitals and outpatient facilities, establishing a few minimum requirements for telemedicine spaces and offering additional recommendations supported by research and best practices. FGI began by establishing a glossary definition for what the Guidelines means by telemedicine: “The use of electronic information and communications technologies to provide and support health care when distance separates the patient and medical provider.”
A note appended to the glossary definition further delineates this simple definition: “Clinical applications of telemedicine may encompass diagnostic, therapeutic and forensic modalities. Common applications include pre-hospitalization assessment and post-hospital follow-up care, scheduled and urgent outpatient visits, medication management, psychotherapy and consultation. Patient and provider consultations, medical imaging, remote monitoring and education are all services that can be provided via telemedicine.
Resources
A variety of technologies, including videoconferencing systems, internet-based websites, digital phones and secure email can be used to deliver telemedicine services. Telemedicine facilitates the exchange of health information, services and education between providers and providers or patients through electronic means.”
Multiple sources were used as a foundation for the proposals that became the basic requirements and recommended appendix language for telemedicine spaces in the 2018 Guidelines, including:
- Papers about telemedicine workspaces from Janet Major (2005) and Elizabeth Krupinski (2014), both of the Arizona Telemedicine Program;
- California Telemedicine and eHealth Center’s “Telemedicine Room Design: Program Guide” (2011);
- Guidelines for telehealth rooms used by the Provincial Health Services Authority in Canada;
- American Telemedicine Association’s telemental health standards and guidelines (2009);
- A consensus report published in the Journal of Digital Imaging on consistency and standardization of color in medical imaging (2015).
FGI requirements for telemedicine spaces are not intended to apply to virtual visits that do not require a physical examination of the patient or visits that originate from a physician’s or patient’s home. Appendix language recognizes the patient experience, understanding that remote communications via electronic equipment can be a necessary supplement to in-person care. A reminder is also included that design of telemedicine spaces should facilitate natural communication for the widest range of participants, including elderly patients, those unaccustomed to electronic communication and those with vision, hearing or cognitive impairments.
Common requirements
Telemedicine requirements are included as part of the common elements for both hospitals and outpatient facilities in the 2018 Guidelines. Where an organization provides clinical telemedicine services, a bay, cubicle or room must be provided to accommodate those services. Requirements are given for the size of telemedicine spaces, privacy, acoustics, lighting, interior surfaces, site identification and storage for equipment. Where low patient volume makes provision of a dedicated telemedicine room impractical, the space also can serve other functions such as a physician’s office, exam room or conference room.
In the appendix, the Guidelines indicates that telemedicine services may include one-on-one interactions, consultations with a patient and family members (e.g., pediatric or elderly patients), examinations supported by a telemedicine presenter located with the patient, or specialty services such as dermatology or orthopedics. Throughout the section on telemedicine, recommendations accompany the minimum requirements for designers to consider when designing telemedicine spaces. For example, each type of service provided may have specific needs for lighting and space to support the clinical function. Thus, it is important to know what services will be provided in the telemedicine space to achieve a functional design.
Space requirements. Where a telemedicine bay, cubicle or room is used for patient examination, the space must be sized so that an exam table can be situated within view of the camera and the following can be accommodated: fixed or mobile telemedicine equipment, peripheral devices, an on-site caregiver or patient presenter, a hand-washing station where hands-on exams are provided and a documentation area. For privacy, the space must also permit arrangement of monitors, screens or other image or data projections so that they are not visible from outside the telemedicine space.
Further considerations for sizing a telemedicine space are described in the appendix. One of these is the proximity of the camera and microphone to the patient. The camera and exam table should be positioned so that a presenter using and manipulating telemedicine peripherals can see both the patient and the monitor, with images being transmitted to the remote clinician’s site. Space for microphones should be available in front of and close to the individuals speaking in the videoconference, ideally at least 4 feet from the telemedicine workstation to prevent audio feedback.
The room should be large enough for the patient and the patient presenter (if one is present) to move around comfortably for the type of clinical service being provided. For example, when an examination includes gait evaluation, the telemedicine space should be large enough for this activity to be captured by the camera.
Acoustics. A telemedicine room must have an acoustic environment that facilitates speech intelligibility and communication. Appendix recommendations suggest that the room be in a quiet location to minimize exposure to background noise that can be picked up by microphones. Therefore, locations near open office areas, busy corridors, stairwells, parking lots, waiting rooms/areas, HVAC systems and toilet rooms are unsuitable.
A telemedicine room also must be designed for the sound isolation rating appropriate for its clinical function. In designing to achieve this minimum sound transmission class rating, consideration of all portions of the room envelope is recommended, including walls, floor/ceiling assemblies, doors and glazing as well as field conditions that may affect the performance of those elements. As well, background noise levels in telemedicine bays, cubicles and rooms must be suitable for the clinical functions performed in the space.
These requirements for speech intelligibility, sound isolation and background noise are all based on the acoustic design requirements in Part 1 of the Guidelines.
Lighting. All spaces intended for telemedicine services must allow direct frontal lighting. However, it is recommended that both direct and indirect lighting be provided to support creation of images with even lighting and accurately reproduced colors. According to the sources on which the new Guidelines requirements were based, full-spectrum or warm, white light (3200-4000 K) with a minimum light level of 150 foot-candles is appropriate.
Means of controlling glare from natural and artificial light sources also are required. For example, shades or blinds can reduce light and glare in rooms with windows. In these spaces, it also should be possible for clinicians and patients to avoid sitting in front of a window unless backlighting can be adequately addressed. Diffused light shining diagonally toward the patient is recommended to reduce shadows on the face caused by overhead lighting or a light source behind the patient.
Interior surfaces. The finishes and colors selected for a telemedicine bay, cubicle or room must be able to support natural rendition of color and pattern. As indicated in the Guidelines appendix, the sources referenced in development of the text were consistent in finding that light to medium blue or light gray matte finishes are best for proper rendering of color and facilitating picture clarity. These shades are preferred because they offer minimal light absorption and reflectivity. If a space is used for other functions, screens or curtains may be used to provide the appropriate background color or to hide clutter (e.g., bookshelves and framed pictures with glass).
The Guidelines requires the backdrop wall color to have a light reflectance value of 30 to 40 percent. In the appendix, a surface finish gloss rating of Level 1 or 2 (flat finish) is recommended rather than a gloss rating of Level 5 (semi-gloss) or 6 (gloss finish) to avoid glare and reflections. Also in the appendix are recommendations to avoid glare and contrast by specifying these light reflectance values for surfaces: 80 to 90 percent for ceilings, 25 to 45 percent for furniture and 20 to 40 percent for flooring.
Site identification. Facility identification must be provided at the telemedicine site so that it appears in the transmitted image unless such identification is embedded in the electronic telemedicine platform. This signage is sometimes required for reimbursement, but is also helpful for reminding clinicians and patients where the person with whom they are speaking is based when telemedicine services are offered between multiple locations.
Equipment-associated issues. Secure storage is required for telemedicine spaces where portable equipment and peripheral devices (e.g., digital cameras, task lighting and electrocardiogram devices) are used. Additional guidance for equipment used for telemedicine services includes camera placement so that participants in the telemedicine communication perceive the exchange as happening eye-to-eye, and provision of temperature controls based on the heat the electronic equipment may generate. Depending on the complexity of equipment used, multiple outlets may be required. Finally, a reminder is given to select and install telemedicine equipment to facilitate cleaning and support infection-prevention practices.
Continuous evolution
Telemedicine and telehealth have evolved quickly over the past few years, suggesting that they will continue to develop at a rapid pace. As technology advances and organizations become more familiar with platforms and service options, minimum built-environment standards to support these practices may need to be refined.
Although HGRC members debated whether advanced technology could make up for shortcomings in the physical environment, robust discussions suggested that many organizations will not invest in the highest-quality technology. Moreover, even some of the most prestigious health care systems in the country acknowledge that they learn from their mistakes and make necessary corrections to the physical environment or communications equipment — an approach not all organizations may be able to afford.
In the end, as language for the 2018 Guidelines was established, the HGRC focused on balancing a small amount of verbiage as required minimum standards with more extensive recommendations in the appendix. The goal was to allow enough flexibility for organizations to ascertain their own level of need based on services rendered.
Spaces for telemedicine communications should strive to maintain the level of safety, privacy, quality of care and patient experience that would be expected for communication when it takes place in person. As more evidence becomes available, telemedicine requirements in the Guidelines will adapt, through revised language for minimum standards and updates from the field in FGI’s “Beyond Fundamentals” platform.
Ellen Taylor, Ph.D., AIA, EDAC, is vice president for research, The Center for Health Design, and a member of the steering committee of the FGI Health Guidelines Revision Committee. She can be reached at etaylor@healthdesign.org.





