FGI’s Guidelines balance risk and cost

The nursing homes chapter in the 2022 Residential Guidelines features clarified resident room sizes and clearances. This room has a cabinet at the entry to store occupant medications that support decentralized medicine delivery and windows that are oversized to maximize natural light and views of nature.
North Ridge at Eliseo by Shoesmith Cox; photo by Benjamin Benschneider
One of the most surprising regulatory conversations I had in the past two years began with a question about droplet versus aerosol precautions and how they relate to the ventilation that should be required to mitigate COVID-19 transmission. I expect these kinds of questions from designers and engineers. I don’t expect them from my retired aunt, an English teacher who has always viewed my interest in health care design regulation as a curious personality defect.
Conversations like this made the 2022 revision cycle for the Facility Guidelines Institute’s (FGI’s) Guidelines for Design and Construction documents unlike any seen before. It is common for Health Guidelines Revision Committee (HGRC) members to hear debate about hand sanitization and what design is appropriate to isolate airborne infectious agents. Only after the onset of the COVID-19 pandemic have these topics become part of dinner table conversation.
This national public focus (and often controversy) over methods for containing infection underscores the important preparatory work the HGRC engages in every cycle. Every four years, a group of experts is convened to update the most recent edition of the Guidelines. This group — the HGRC — asks the simple question: What is a reasonable level of building safety? The HGRC frames that question not only in terms of what’s reasonable for routine events but also for extraordinary ones.
Expectations for 2022
The answers inform the newest edition of the FGI Guidelines documents, which are used by most states and federal agencies, in sum or in part, as regulatory minimums. They are also the de facto planning and design standards for the health and residential community.
To set expectations about what is in the 2022 documents, perhaps it’s best to start with a topic that has not seen major changes. Considering the COVID-19 pandemic era into which the 2022 edition was born, it may be a surprise that there are no sweeping changes adding airborne infection isolation capacity or similar COVID-19-related mitigations. There are a couple of reasons for this.
First, the pandemic occurred at the midpoint of the revision cycle, past the point where new ideas could be considered, except to correct an error or clarify a significant issue. Second, the HGRC does its best to consider changes to minimum standards from a broad perspective and, while there are times when it is appropriate to respond quickly and purposefully, discretion is needed when making significant decisions that will affect health and residential care facilities for years to come.
Typically, during the process of revising the most recent edition of the Guidelines, the approach of the HGRC tends to revolve around conversations on two main topics:
- New ideas and data about relevant changes in how care is provided and in design and construction industry practices.
- The inexorable push and pull of what must be done versus what is recommended or best practice.
To the first point, the 2022 HGRC advanced several ideas it believes will aid in the design of facilities and the provision of care.
As health care organizations continue to adapt to new expectations and growing needs around behavioral health, the HGRC considered many approaches to solving physical environment problems. It tested some of those new ideas and created more options to aid in this response. Sometimes too many options can be overwhelming, but — given the broad spectrum of inventive responses based on unique operational plans — the HGRC believes the menu of space options provided in the 2022 Guidelines for addressing behavioral and mental health care needs will help care organizations and design teams determine how best to move a project forward. Guidelines users should expect to see options for behavioral health crisis units, emergency department rooms designed specifically for behavioral and mental health care, and spaces to accommodate intensive outpatient/partial hospitalization programs.
Similarly, the HGRC acknowledged the need to add guidance for several specific services that may be relatively uncommon for a typical hospital and therefore have not previously had a dedicated section in the Guidelines. These additions are based on well-tested designs or new approaches to old problems that have been employed enough to enter mainstream use. For example, the Hospital Guidelines now has sections on specialty hospital units such as hospice and burn care, and the Outpatient document describes how to create dual-entry exam rooms to support improved patient throughput.

The 2022 Guidelines for Design and Construction of Hospitals includes requirements when a burn trauma ICU is provided. Because burn patients are highly susceptible to infection, patient rooms in this unit must be designed as protective environments.
University of Wisconsin Hospitals and Clinics, UW Health F8/4 burn and wound care ICU, by HKS; photo by Bruce Fritz
After several years’ work, the HGRC created standards for patient care stations for treating low-acuity patients in the emergency department. The requirements for resident rooms in the Residential Guidelines and the requirements for dialysis facilities in all three books were updated to align with federal requirements for participation in the Medicare program. While many of the concepts covered by these requirements could be accomplished before, their inclusion in the Guidelines makes it easier to receive approval from authorities having jurisdiction (AHJs).
To the second point, the HGRC also tested the boundary of “should” versus “shall” language. This is a perennial tug-of-war between minimum standards and best practices. FGI has long held the position that standards should be based on risk. Many Guidelines requirements (e.g., write a functional program and create an infection control risk assessment) are opportunities for care organizations, designers and AHJs to probe the specific risks for a facility and apply the Guidelines in a way that best mitigates those risks.
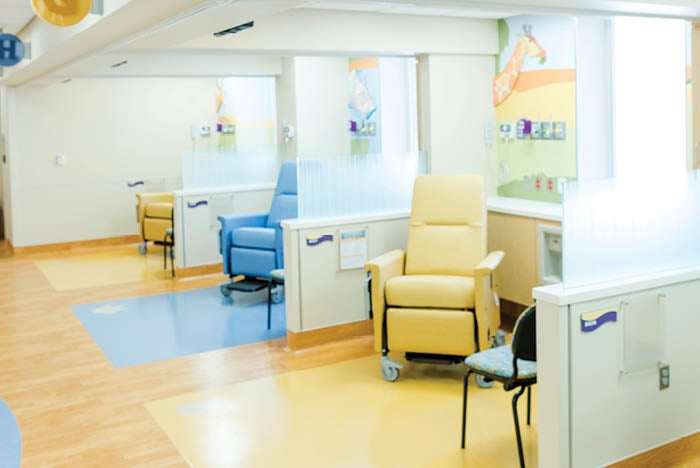
Revisions made to the outpatient dialysis facility requirements in the 2022 Guidelines provide improved sightline requirements, minimum clearances around chairs instead of clear floor areas and modifications for patients who require special precautions.
Children’s Health, Children’s Medical Center, Dallas, nephrology tower renovation, by HKS Inc.; photo by HKS Inc.
Expect to see more flexibility in the 2022 Guidelines requirements based on a clearer understanding of risk, clarity that influences documentation and conversations with AHJs. In several cases, the number of requirements or the size of a room has been adjusted. Most of these changes are reductions that result from learned experience and a careful review of existing requirements.
The 2022 revision cycle saw several changes that cede control back to health and residential care organizations and design teams to make good decisions for the projects they represent. However, along with this control comes risk. For example, a requirement for commissioning and training for special systems (e.g., elevator control, access control, special power control, etc.) was deleted. This could be seen as a good deal for hospitals with a very robust in-house commissioning program and clear contractual expectations for getting these systems up and running, training staff, and handing off operations and maintenance responsibilities for such systems.
From the perspective of these hospitals, their procedures cover — if not exceed — the requirements in the Guidelines. For organizations that do not have such a program, or perhaps that can barely muster the resources to keep up with a big project, this change transfers risk back to the organization. The risk is that the design team or the facility staff will not be adept enough to ensure the systems function properly and staff won’t know how to maintain them. It’s a classic discussion about self-determination, where some facilities, staff and patients may benefit and others may not.
The HGRC ultimately did not settle a few important issues — primarily the proposal to include a chapter on extended stay centers in the 2022 Outpatient Guidelines. This facility type, often associated with an outpatient surgery facility, is intended for postoperative care for patients who cannot travel home the same day because of distance or who may need care for more than 24 hours post-procedure. Because the services provided in such a facility would be relatively limited (i.e., follow-up for simple ambulatory surgery procedures), the HGRC anticipated a physical environment less restrictive than that of a hospital would be permitted.
However, concerns arose over the inclusion of an extended stay center as an outpatient facility, as the type of care provided would challenge some fundamental concepts of what separates inpatient services from outpatient services. That traditional line — 24 hours of continuous care for a specific patient in a specific place — has been carefully defined and articulated over the past few decades in the building and life safety codes, not to mention the licensing codes in many states. The heart of the concern is that defining an extended stay center as an outpatient facility would create conflict and confusion across requirements and cause significant challenges to enforcement. This concept is still an excellent idea and one the HGRC will pursue in the next cycle.
Anticipating 2026
In addition to extended stay centers, the HGRC expects to pick up several other topics in the 2026 cycle. A primary focus will be considering the lessons the industry continues to learn from the COVID-19 pandemic and determining how to incorporate this knowledge into the Guidelines. There have been many calls to rethink the physical environment over the past two years, but the HGRC does not react to those voices without focused thought from a broad group of perspectives. FGI’s Emergency Conditions Committee was formed to do just that, and their efforts resulted in a white paper and a series of recommended changes to the Guidelines. It’s now the task of the HGRC to take those recommendations and vet them through the HGRC’s rigorous process.
Another exciting effort will be to consider a new facility designation from the Centers for Medicare & Medicaid Services (CMS). In 2021, the Consolidated Appropriations Act created a new federal designation intended to allow certain hospitals to participate in a new reimbursement program for the “rural emergency hospital.” The operational footprint of this facility type appears to be a little different than a traditional rural or critical access hospital. Effectively, it is an emergency room with the potential for some wraparound services and perhaps the addition of a skilled nursing unit. The CMS rule-making process is already underway to launch the program by 2023. The HGRC will watch carefully as CMS further determines the functions permitted and their expectations for the provision of care in rural emergency hospitals. The 2026 cycle will be a good opportunity to consider standards for this new facility type and describe those fundamental requirements in the Guidelines.
Also, there is interest in considering development of survey standards for existing facilities. Like most building and construction codes, the Guidelines documents provide fundamental requirements for new construction and major renovation projects. However, the current edition of the Guidelines should not be applied retroactively to existing facilities unless the physical environment or the function of a space is changed. Here is the rub, though: Most AHJs and accrediting organizations perform annual surveys of existing facilities, and putting an existing facility into the appropriate context may require access and understanding of many Guidelines editions. The interesting concept is to consider all the previous iterations and establish a “lowest common denominator” set of survey standards that could be used for existing facility surveys. This approach does not intend to encourage a new facility to go backward, such as surveying a one-year-old facility to standards from 1960. Rather, the goal is to create a good starting point for existing facility surveys.
The HGRC will also continue conversations it’s been having for years. Additional attention will be given to spaces for treatment of behavioral and mental health patients. The HGRC has new territory to chart in facility types that range from forensic to residential, and it will continue exploring extended stay centers.
Finally, the health care fields all bore witness as the pandemic evolved into a staffing crisis. Now the HGRC must consider how to design buildings that are more efficient for the staff. For the Guidelines, that translates to asking how the regulations assure safety while accommodating efficiency. The pandemic has exacerbated chronic problems around transitioning patients out of the hospital into other institutions. Maybe the HGRC needs to create a new or redefine an existing hospital space to aid in those transitions? The HGRC doesn’t adequately describe the design of long-term acute care facilities, whether in the hospital or as a standalone facility. This is worthy of at least a new section, and perhaps a new chapter. All these ideas require a challenging, interrogating review that asks repeatedly: What is reasonable? What is a fundamental requirement, and what is a best practice? What is the substantiation to support the conclusion?
Broader perspectives
To my aunt’s question, I gave her the simple yet unsatisfying answer of an AHJ: it depends. Describing something that is measurable can be done in finite, albeit complex, ways. Sorting those measurements into categories helps make sense of complexity. What “should” be done versus what “shall” be done with those categories often depends on one’s interpretation and perspective. But don’t worry, with each revision cycle, the HGRC gathers — and acts on — better information.
The HGRC has broader perspectives around the table, which leads to richer discussions. It has a community of designers who are always asking “What’s next?” and “What’s better?” There is a country full of AHJs and facilities engineers whose goal is not mere compliance but enhanced protection and safety for both patients and staff. And there is a broad array of clinical personnel who keep the HGRC focused on how the physical environment can best support staff and improve patient outcomes.
Essentially, a whole team of health care design professionals is working on answering my aunt’s question. And it’s an exceptional team.
E-commerce site and digital library created for the 2022 FGI Guidelines
The Facility Guidelines Institute’s (FGI’s) 2022 Guidelines for Design and Construction documents are available for purchase in paperback and digital formats. The digital format features enhancements such as productivity tools that allow users to highlight important text; create notes on a specific section; bookmark pages; and review errata and formal interpretations, as well as application guidance, at the associated section of the Guidelines. The digital format is available as a single-user or multiple-user license and is renewable annually.
The new e-commerce website delivers pricing transparency and offers a user-friendly checkout, with options to create an invoice for a purchase order and (for nonprofit organizations) to select a tax-exempt option and upload tax-exempt documentation. These cart options speed up the ordering process for nonprofits and government organizations purchasing the Guidelines and reduce the operational burden on account administrators.
Organizations taking advantage of the multiple-user license may invite an unlimited number of users to join the licensed account and will only be charged for the number of individuals needing access to the Guidelines at the same time. Account administrators for multiple-user licenses also may designate access to users in any number of locations without incurring additional site-based fees.
The goal of FGI’s new e-commerce site is to give users of the Guidelines convenient and cost-efficient access to the documents from one location. Digital and paperback versions of the 2018 and 2014 Guidelines can also be purchased directly from FGI’s e-commerce site. For those needing access to older editions, the 2010 Guidelines and previous editions may be downloaded in PDF format at no cost.
John L. Williams is an executive director within the office of community health systems at the Washington State Department of Health. He has been a member of the HGRC since 2011 and is chair of the 2026 FGI HGRC. He served as vice chair during the 2022 Guidelines revision cycle. He can be reached at john.williams@doh.wa.gov.




