Efficient emergency department designs
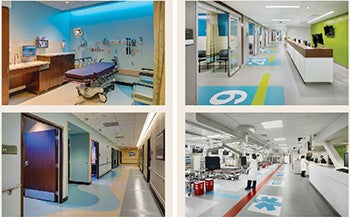
Top Left: The pediatric treatment room lighting in Florida Hospital Kissimmee's emergency department can be changed to match a child's favorite color. Bottom Left: The department features separate pediatric (pictured) and adult treatment areas. Top Right: Treatment room and trauma bay numbers are indicated by floor graphics at the Pavilion for Advanced Care expansion to Penn Presbyterian Medical Center in Philadelphia. Bottom Right: The EMS insignia is incorporated into the flooring to identify where these providers stand.
In the emergency department (ED), time counts. “Whether it’s a minor laceration or a massive [heart attack], in the view of the patient and the consumer, it’s an emergency. And they’re looking for rapid treatment,” says Susan S. McGaughan, R.N., NE-BC, central region business manager, emergency departments, Connecticut-based Hartford HealthCare.
EDs used to be considered the back door to the hospital, “built without any thought toward patient flow and efficiency,” says C. Michael Remoll, M.D., medical director of the ED at Anne Arundel Medical Center, Annapolis, Md.
But EDs are increasingly the primary entry point for hospital patients. “As we become more interested in patient flow and efficiency and patient satisfaction,” Remoll says, “it becomes more important to determine how you want to function and then to build [the ED] around that.”
“Nobody wakes up in the morning saying, ‘Hey, I want to go to the emergency room today,’” says Marvina Williams, R.N., senior medical planner, Lean black belt and senior associate in the Atlanta office of design firm Perkins+Will. “The biggest satisfier for patients is being able to be treated in a timely fashion.”
You may also like |
| New strategies in ED design |
| Trends for freestanding EDs |
| Designs to improve patient flow |
| |
Efficient ED design is important both to save the lives of seriously ill or injured patients and to make getting stitches a little less miserable.
Efficiency and functionality
According to Williams, reducing waste and providing value to the customer are key to facility design. “Meeting with the users and understanding their current processes and then developing future process maps that improve the patient and staff experience provides a facility that is efficient and functional,” she says.
Efficient triage areas and departmental layouts that separate low-acuity patients from those in need of more acute care can be central to increasing patient throughput and decreasing wait times in the ED. At Anne Arundel Medical Center, a rapid clinical evaluation area and several blood draw stations near the front of the ED help to move low-acuity patients through the treatment process efficiently. Susan Gray, R.N., the hospital’s ED clinical director, says, on average, only 1.1 percent of people who arrive at the department leave without being seen.
In the ED at Hartford HealthCare’s MidState Medical Center, Meriden, Conn., patients are greeted in the lobby and quickly registered and assessed by a doctor or nurse; there’s no front area called a waiting room, “because our expectation is that people are not waiting on that side of the environment,” McGaughan explains. “They are waiting for their treatment within the clinical space.” Since the hospital transitioned to its newly designed and expanded ED, the average time it takes for a patient to be assessed by a provider after entering the department has dropped from greater than 30-45 minutes to between 12 and 16 minutes, she says. Eighty-five percent of patients are seen by a provider within half an hour, versus less than 50 percent in the old ED.
Other ED design developments include the use of private rooms instead of curtained-off treatment bays. Treatment rooms often are arranged in modular groupings, or pods. The modular layout enables hospitals to staff and operate the ED in accordance with daily or seasonal fluctuations in the patient census. Special populations, like pediatric and behavioral health patients, are provided dedicated areas where possible so that their needs can be managed more efficiently. Waiting rooms within the ED provide a comfortable place for patients to await test results, freeing treatment spaces for use by other patients.
High capacity
The ED at Parkland Hospital, Dallas, is designed for 180,000 patient visits annually, a figure Kathy Harper, EDAC, vice president of clinical coordination for the new Parkland campus, expects the hospital to meet within its first year of operation at the 2.5-million sq. ft., 862-bed facility.
“About 80 percent of our inpatient volumes come through our ED,” Harper says. “We had to ask ourselves, ‘What volume can we truly handle on this campus?’” Maximum inpatient capacity was a significant factor in the design of the ED, which has 154 treatment rooms divided among the department’s standard ED, Level I trauma, women’s health and behavioral health programs.
The treatment rooms are organized into pods of 12 or 14. Windows in the treatment room doorways are made of two panes of glass with alternating stripes of frosted and clear glass, which can be positioned for privacy or visibility. The solid doors have additional leaves so the rooms can be opened wide enough to admit a trauma team.
The majority of the treatment rooms are standardized at 135 sq. ft.; there are also 10 resuscitation rooms that cover almost 700 sq. ft. each. Four trauma rooms are sized and equipped as surgical suites. “If we do not have time to transport the patient directly to the OR [two floors above the ED], which is always our first preference, we can do procedures directly in the trauma rooms,” Harper says. The ED has five rooms designed to be used as step-down recovery space.
There are two trauma elevators. The largest of these, specially designed to hold an entire trauma team and equipment, is known at the hospital as the “megavator.” It can transport patients from a rooftop helipad to the trauma department in about 30 seconds, a trip measured in minutes at the existing Parkland Memorial Hospital. “Seconds count when you have a trauma,” says Harper.
Dan Thomas, AIA, EDAC, senior medical planner and director of health care planning in the Dallas office of design firm HDR, says evidence-based design informed much of the project, such as the inclusion of natural light in all waiting areas. Harper says the design is intended to help people who are experiencing a health emergency feel comfortable and give them privacy and family space, so “they can just be who and what they need to be at that particular time.”
Community care
Streamlining patient flow was one of the primary concerns in the expansion of the ED at Florida Hospital Kissimmee, says Robert Geissler, the hospital’s director of nursing, emergency services and observational medicine. “There are a lot of correlational studies that say the sooner [patients] can see a doctor, the better outcomes they have,” he says.
The expanded ED has separate entrances for walk-in patients and those who arrive by ambulance, and a separate pediatric waiting room. There are two triage rooms, one for rapid assessment and one in which caregivers can begin treatment protocols. Two eight-bed, fast-track treatment areas for low-acuity patients are located on one side of the ED; on the other side, there are 18 critical care beds — including two trauma bays, one for adults and one for pediatric patients, and two rooms for behavioral health patients. In a separate area, there are four treatment rooms designed specifically for pediatrics; each has an underwater theme and lighting that can be changed to match a child’s favorite color. The ED also has a test results waiting area furnished with 12 recliners and a big-screen TV.
Geissler reports that since completing the ED project last October and subsequently building a three-story bed tower at the facility, admissions at Florida Hospital Kissimmee are up 20 percent. “They used their ED as kind of the seed for that market,” says Todd Robinson, AIA, EDAC, principal, Earl Swensson Associates Inc., Nashville, Tenn. Despite the higher volume, the ED’s door-to-provider time and the time it takes to transfer an ED patient to an inpatient bed both have gone down by about 30 minutes, and patient satisfaction scores, as measured by Press Ganey Associates Inc., South Bend, Ind., have risen to near the 50th percentile nationally, from below the 25th percentile, Geissler says.
Technology’s role in improved ED performance

HKS Inc., Dallas, has developed a conceptual design for serving the nearly half of ED patients who can be treated without a traditional bed.
Technology is fundamental to efficient emergency department (ED) designs and operations. “Technology is so important — looking at what is new,” says Marvina Williams, R.N., senior medical planner, Lean black belt and senior associate in the Atlanta office of design firm Perkins+Will. Digital registration kiosks and bedside registration systems streamline the registration process, allowing patients to be treated quicker. Electronic patient tracking boards can reduce wait times and improve turnover by helping caregivers to monitor information critical to patient flow.
Rush University Medical Center (RUMC), Chicago, uses patient flow software by TeleTracking Technologies Inc., Pittsburgh, to increase organizational effectiveness. The system monitors available beds by specialty, automating a process previously performed by three separate nurses walking the hospital carrying clipboards and searching out empty beds, says Edward J. Ward, M.D., FACEP, assistant chief medical officer and vice chair of the RUMC department of emergency medicine. Getting patients into beds sooner frees up available space in the ED and decreases wait times. With the TeleTracking system, Ward says, the hospital no longer has patients in hallways, waiting for rooms — a situation he describes as “a patient satisfaction killer” — and it is rare for the hospital to go on bypass.
According to Ward, the level of detail the system provides about what patients the facility can handle helps the hospital to operate effectively and make better decisions on allocating resources. Neurologists at RUMC used patient tracking data to calculate the number of patients declined by the hospital by service line and the cost per declination to make a case for establishing a new stroke program at the medical center. Telemedicine features of the software enable RUMC to extend these resources into the community by allowing physicians at several area hospitals to consult electronically with RUMC doctors.
Ward says the system is essential to the hospital’s transfer program, too. The software coordinates transfer requests and automatically documents the process. The transfer center handles nearly 4,000 patients a year, contributing approximately $53 million to hospital operations, he notes.
Future ED environments may leverage technological advances. According to designers at HKS Inc., Dallas, research by leading ED operations analysts shows that nearly half of incoming ED patients can be treated without a traditional bed. HKS has developed a conceptual design for these patients that requires much less square footage than a standard ED treatment bay. The design features semi-enclosed seating areas, called pods, with pull-out tables and other amenities similar to first-class airline accommodations. Each pod has room for the patient and two family members as well as the provider. The environment offers enhanced privacy and personalization, says Mik Pietrzak, M.D., chief medical adviser, HKS Team ED. Patients can use an iPad to communicate with caregivers, play music or change their personal lighting settings. Parametric speakers create a cone of sound around each pod to contain noise and protect patient privacy. The pods can be arranged in a variety of ways to optimize flow and staffing efficiency.

Efficient design helps to move emergency department patients through the treatment process at Anne Arundel Medical Center, Annapolis, Md., which reports that an average of only 1.1 percent of people who arrive at the department leave without being seen.
Treating trauma
The Pavilion for Advanced Care is a six-story expansion to Penn Presbyterian Medical Center (PPMC), Philadelphia, which is part of the University of Pennsylvania Health System. In addition to increasing PPMC’s ED capacity by 16 beds — plus a five-bay rapid assessment treatment area and space to wait for test results — the project added a Level I trauma center to the facility.
“While it originates in the ED, [trauma] touches every department,” says Alyson Cole, assistant executive director for professional services, PPMC. “It requires some special thought in the design of the building.” The new tower is topped by a helipad large enough to accommodate a Black Hawk helicopter. Two of the new pavilion’s floors are dedicated to intensive care. The radiology and surgery departments are positioned to allow easy access from the trauma center and ED; one operating suite is designated for trauma cases. To help the medical center manage an influx of higher-acuity patients, the project team developed a compounding pharmacy for the facility and ensured that the blood bank had the capacity to support a Level I trauma program, says Mary Frazier, AIA, LEED AP, principal, Philadelphia-based design firm EwingCole.
The trauma center and ED include several features designed to make them more comfortable and efficient for patients and staff. Clerestory windows bring natural light into as much of the space as possible, Frazier says. This includes the five-bay trauma resuscitation area. Treatment room and trauma bay numbers are indicated by bold, bright floor graphics. The emergency medical services (EMS) Star of Life insignia is incorporated into the flooring at each trauma bay to identify where EMS providers should stand as part of a care team. The 29 ED treatment rooms include coat hooks and outlets for charging handheld electronics for family members’ convenience. One treatment room, designed for bariatric patients, is outfitted with an overhead patient lift. Garage-type doors can be rolled down to conceal carts and casework in one treatment room, so it can be converted easily to ensure the safe care of behavioral health patients. Two rooms in the department are designed for bereavement or consultations.
Cole says the impact of the project is difficult to measure just yet, since ED renovation is ongoing (it’s scheduled for completion at the end of this year) and the trauma center has been open only a matter of months, but she notes that ED and hospital admissions are up and referrals continue to be strong. In the community, “there’s a perception that we have a new capacity for care,” she says.
Disaster-ready
The McCormick Foundation Center for Advanced Emergency Response at Rush University Medical Center (RUMC), Chicago, is designed to handle standard emergencies and respond to mass public health disasters like a pandemic or bioterrorism event.
The center’s 60 private treatment rooms are each sized and equipped to handle two patients, if necessary, to double ED capacity during a crisis. Medical gas lines and outlets are installed in the columns of the hospital’s lobby so this space can be used to care for up to 200 patients. The medical center can create a “wall of water” to decontaminate ambulances outside the facility. Portable decontamination units can be connected inside the building’s enclosed, secure ambulance entrance; a 10,000-gallon tank is installed beneath the ambulance entrance to contain contaminated water. A shower room off the ambulance entrance will allow a smaller number of individuals, on foot or on stretchers, to be decontaminated prior to entering the ED.
The treatment rooms are arranged in four pods, designated A, B, C and D. In addition, there are three negative-pressure isolation rooms, each with a private bathroom and an anteroom for gowning and decontamination. If additional isolation rooms are needed, the air handling system is engineered so that all of pod C, or all of pods B and C, can become an isolation unit comprising up to 42 beds.
Pod B is designed for critical care patients and has a dedicated enclosed area for behavioral health patients. In the critical care rooms, medical equipment is installed on booms for easy cleaning and maintenance. The three behavioral health rooms utilize harm- resistant design and materials and allow for direct observation of patients. Pod C is staffed for pediatrics and Pod D has adjacent radiology services, including two dedicated computed tomography scanners.
The number of patient visits to the ED has risen annually since the facility was completed, from 58,284 in fiscal 2012 to 71,949 last fiscal year. Shonda W. Morrow, R.N., director of nursing resource management and operations, RUMC, says that given this volume of patients, the medical center is undertaking several process improvement efforts to decompress the ED and flow patients more efficiently. Edward J. Ward, M.D., FACEP, assistant chief medical officer and vice chair of the RUMC department of emergency medicine, says the facility project has given staff the opportunity to design, build and operate a state-of-the-art building.
Quality experience
“As a design professional, I want [patients] to have the best experience they can in the circumstances they are in,” says Thomas. He says the physical environment of the ED is part of the delivery of care: Designs that allow people to work safely and efficiently reduce stress, so patients, physicians and staff can focus on healing.
Amy Eagle is a freelance writer based in Homewood, Ill., who specializes in health care-related topics. She is a regular contributor to Health Facilities Management.
The growing importance of freestanding EDs
Freestanding emergency departments (EDs), though not yet approved in all states, are a growing way for hospitals and medical groups to extend emergency services beyond the traditional hospital setting, says Kevin M. King, ACHA, ACHE, associate AIA, senior design manager for architecture firm Earl Swensson Associates Inc., Nashville, Tenn.
Davis Hospital and Medical Center, Layton, Utah, which is part of the Franklin, Tenn.-based IASIS Healthcare system, recently opened a freestanding ED on the medical center’s Weber campus in Roy, Utah, eight miles from the main hospital campus.
Leslie A. Christiansen, R.N., CEN, Davis Hospital emergency department director, IASIS Healthcare, says the area is experiencing a lot of growth, and while the community didn’t need another acute care hospital or urgent care center, it was lacking in emergency services. Hill Air Force Base, located across the freeway from the Weber campus, has a clinic but does not provide emergency care. And the 15-minute drive from the Weber campus to the hospital can take much longer when the road is blocked, as often happens, by freight train traffic. The freestanding ED was seen as a way to deliver centralized emergency medicine to the region and to stabilize and transport patients who need more specialized treatment to the appropriate setting, such as a stroke or trauma center. The hospital reports that recently an injured child’s life was saved because emergency medical service providers were able to quickly access the freestanding ED facility.
The 16,000-sq. ft. ED has 14 treatment rooms, eight of which are arranged in two pods of four rooms. Each pod has a central work area and its own bathroom, a layout Christiansen describes as convenient for patients and staff. There is also a trauma bay, a main orthopedic room, a negative-pressure isolation room (which also has its own bathroom) and two overflow rooms that the ED shares with a radiology department. The ED offers full-service laboratory, mammography, respiratory and radiology services, including X-ray and computed tomography. The hospital plans to add portable magnetic resonance imaging soon.
In the two years the freestanding ED has been open, its patient volume has more than doubled, from 300 to 400 patient visits a month up to 1,000. The average length of stay is one hour and 38 minutes. “Our turnaround times are so short that it’s actually becoming quite a popular place,” Christiansen notes. “I want the public to say, ‘They’re really good. The doctors are really good, the nurses are all [certified emergency nurses]. They’re awesome!’ But what really gets them is the hour and 38 minutes,” she laughs.




