Researching design dangers in equipment and technology
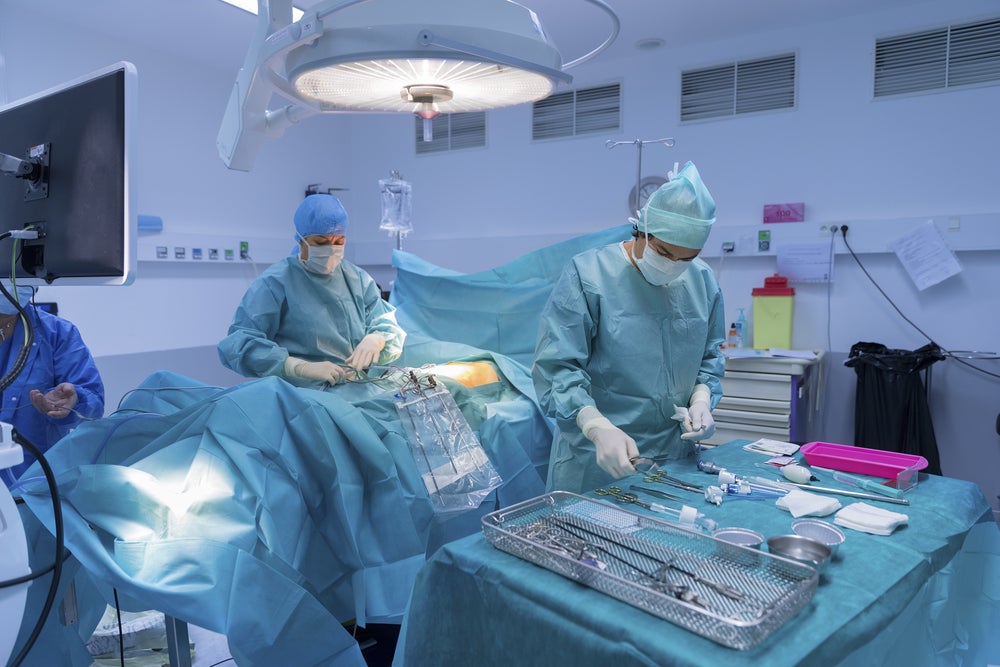
Research into HAIs includes fans in operating room heater-cooler units that can generate HAI-spreading air currents, water reservoirs and other wet environments in surgical equipment and plumbing fixtures that can lead to biofilm formation.
As a well-known authority on drug-resistant pathogens and health care-associated infections (HAIs), Michael Bell, M.D., deputy director of the Centers for Disease Control and Prevention’s (CDC's) division of health care quality promotion, spends a lot of time breaking down silos to talk to health facilities professionals of all stripes on the mechanics behind HAI transmission.
 |
2017 Trends: Infrastructure |
| Previous: Collaborative planning |
| Next: New air-quality research |
|
During the Association for the Healthcare Environment’s EXCHANGE annual conference in September, Bell’s general session went beyond the event's environmental services focus to cover areas of interest to biomedical engineers, facilities managers and those who furnish clinical spaces.
While discussing one of his current research projects, for instance, Bell described fans in operating room heater-cooler units that can generate HAI-spreading air currents, water reservoirs and other wet environments in surgical equipment and plumbing fixtures that can lead to biofilm formation, and equipment ranging from overbed tray tables to endoscopes that are difficult to clean due to contours and crevices.
Eventually, Bell is hoping to develop a list of design “red flags” that health facilities professionals can consider when purchasing or specifying equipment for hospitals. “It's sort of a ranking list of safety levels based on certain design features that we recognize,” Bell says.
While noting that this project will be less about specific products and more about design characteristics, others have been looking into some of the same issues. For instance, ECRI Institute, Plymouth Meeting, Pa., mentioned heater-cooler devices used in cardiothoracic surgery as No. 5 in its recently published list of Top 10 Health Technology Hazards for 2017.
Among other health care technology hazards, ECRI also cautions against overlooking simple steps in infusion pump management; inadequate cleaning of complex reusable instruments; missed ventilator alarms; undetected opioid-induced respiratory depression; software management gaps; occupational radiation hazards in hybrid operating rooms; automated dispensing cabinet setup and use errors; surgical stapler misuse and malfunctions; and device failures caused by cleaning products and practices.
As the CDC, ECRI and others turn a sharp eye toward the role of equipment and technology in patient safety, such research likely will be a growing area of emphasis.




