Designing efficient materials management spaces

Better designed and operating materials management systems are a key substructure of an efficient health care organization.
Materials management is an underappreciated health care operation that either enables or undermines the organization's greater mission.
Also in this article |
| Renovating for operational improvements |
|
|
The real opportunity to increase capacity and decrease cost is on the front line. Bulk material transport and storage may be done by a few people under the materials management umbrella, but this work is dwarfed by the countless hours of real point-of-use materials management done every day by nurses, doctors and others across health systems.
It is common for nurses to spend 20 percent or more of their total time performing fundamental materials management tasks (i.e., searching, transporting, counting and sorting) and it is not difficult to find nurses who spend more than 50 percent of their time on these tasks.
Meeting supply demands
This challenge is felt in every corner of the health system but, for illustrative purposes, the focus should be on surgical services. This is arguably the heart of today’s hospitals, with increasing need for efficiencies and decreasing focus on inpatient stays.
It is also where many key supply chains meet, such as instruments that are owned, loaned and borrowed; consumable supplies; mobile equipment; and, of course, the patient and staff. Add to that the demands of surgeons and anesthesiologists that typically demand highly customized and infinitely variable personal preferences. Everything must be synchronized carefully and highly reliable or the entire system underperforms.
As demand continues to grow, the system will suffer with instruments, supplies, information and staff missing. Every hospital is seeking ways to improve on-time starts, eliminate cancellations, speed up turnovers and generally find capacity. Clearly, there must be a need for more space, more stuff and more staff.
You may also like |
| Trends in supply chain management |
| The business case for pharmacy automation |
| Advancing the health care supply chain |
|
|
Yet, nearly every hospital has sacrificed crucial surgical space to meet storage needs. In fact, some hospital operating rooms (ORs) are being used primarily as storerooms. Add to that the lost capacity due to delays related to searching for missing tools, supplies and equipment and it becomes difficult to tell whether more ORs are needed or the approach to OR materials management needs to change. If staff are spending 20 percent or more of their time managing supplies, are more staff needed or is better management of existing supplies the answer? And do increased levels of stock improve the ability to deliver care or is it added clutter and expense?
The requirement is simple: Have what is needed where it is needed and when it is needed. Design and operations both deserve attention. If building or renovating, the potential exists to eliminate both initial and ongoing operating expenses while making things easier down the road. In considering whether or how much construction is needed, the realization may be that far less new space is required than thought.
Many hospital leaders are highly skilled clinicians. The opportunity to design new space comes along only a few times in a career at most. Biases trend heavily toward a focus on clinical skill and personal competence, not systems and structure. Designers know that user requirements are passionately declared but often inappropriate. And, similarly, designers relying on industry standards can be led astray if those standards don’t keep up with the rapid pace of change
on the floor.
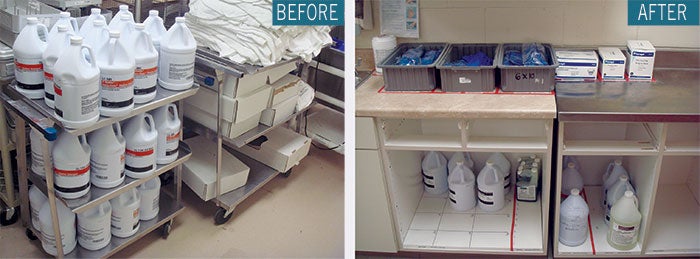
Organized storage of liquid products enables simple reordering routines.
Design advice
Often, the temptation is to design tomorrow’s facilities using yesterday’s thinking. And, despite the upgraded look and feel, the building may be functionally inefficient before it opens. Most designs are too generic and not flexible enough. The following advice will help to avoid these pitfalls:
Less is more. After new construction, many hospitals have random shelves, cabinets and sometimes rooms that have no clear use. They are inserted as placeholders, assuming that something will need to go there.
Those are traps from the start and don’t demonstrate purpose-driven design. Empty space demands to be filled. Clutter accumulates, hiding the important among the miscellany and making everything harder to find. It’s rare to need more storage space when good systems are put into place.
Scarcity demands precision — smaller spaces require better management, make it easier to know inventory levels, limit the amount of counting and searching, and minimize the risks of obsolescence and damage. Of course, this only works as part of a holistic approach — simply leaving space out won’t work either.
Design for what is needed. Extra storage space without clear purpose is not future-proofing nor is it inherently flexible. Typically, too much space exists in the wrong places and not enough in the right places. Different teams in different locations behave differently and they must be understood.
Whatever hours are invested in customizing designs to local processes and behaviors will reap tenfold returns in the long run. Instead of creating superfluous space, facilities planners should spend the time and energy actually understanding what is needed down to the granular level: work to be done, what needs to be stored, quantities and replenishment systems.

Smaller, more-organized supply carts are lighter, more maneuverable and can be easily wheeled into rooms to be restocked.
Often, fewer big shelves and storerooms are needed, and smaller but thoughtful point-of-use storage is required where the work actually happens. Most work doesn’t occur in cabinets by the wall. Instead, work happens at the bedside or the bench. Simulation is a great tool and facilities planners should not be afraid to use it in many different forms. Paper-based and computer-based simulation are helpful, but most valuable is physical simulation where people can walk and touch and experience the design firsthand.
Flexibility is paramount. Regardless of how good people are at planning and customizing designs, it’s certain that plans and designs will be inadequate as technology, demand and knowledge continue to evolve. Consequently, it is important to plan to the extent possible, but even more important is to plan for change. Rooms intended for one specialty need to switch to another temporarily or permanently.
Facilities planners should start by assuming that every storeroom, cabinet and shelf will be the wrong size and in the wrong place, and then look for other approaches. One alternative is fully mobile storage — nothing fixed and everything modular.
With every single aspect of the design, facilities planners should ask, “How can this be more flexible?” Instead of custom-built shelving, is modular an option? Instead of built-in cabinetry, can walls be flat and use freestanding cabinetry? Instead of fixed walls, can modular walls or other means of isolation be used? Can walls move, slide or rotate? Instead of complex multipurpose fixtures and equipment that are built-in, can small, mobile options be used that are easy to move or replace as needs change?
The possibilities are endless if flexibility is the priority — with flexibility, the risk of not planning enough space or not understanding the needs drops dramatically.

High supply shelves can cause efficiency and safety concerns in hospital supply areas.
Operating in the space
Design aside, operations professionals can look at daily activity to make things better. Whether trying to figure out how much extra space is needed or simply bringing recent construction up to its intended potential, getting materials management under control will relieve pressure in the system. The following advice will help to enhance operational efficiency:
Systems over storage. Materials management is not just storage. As much time and energy is spent on designing and managing storage space, the tendency is to underinvest in designing the systems around materials.
Operations professionals should identify and maintain demand requirements. They must determine whose responsibility it is to understand these needs, to keep them current and to rationalize them.
They also should consider what triggers materials replenishment. Computers seem like an obvious answer, but they often are underutilized and the quality of data input drives the quality of data output.
Operations professionals must determine who retrieves and stocks and how they do it. Is counting necessary or can making quantities obvious eliminate counting? How and when should ordering take place? How are people alerted to disruptions or back orders?
Additionally, professionals should determine quantities and storage locations. Depending on how requirements and replenishment are addressed, the actual count and storage space required can vary drastically. Finally, operations professionals must determine how the risk of obsolescence and expiration can be managed. How are materials added or removed as needs change?
Avoid clutter. Whether part of a Lean program or simply decluttering, opertions professionals should get rid of distractions. They should be thoughtful in the use of limited prime real estate. Just-in-case items usually can be stored down the hall, thus allowing staff to focus on what’s needed all the time with contingency plans for the exceptions.

Properly organized OR supplies are easy to find, easy to see if missing and difficult to overstock.
Improve responsiveness. Long or inconsistent lead times require higher levels of inventory. Local suppliers with high reliability allow for less stock. Partnering with others inside the organization or across organizations is often an option to manage safety stock better and to reduce local inventories. And operations professionals shouldn’t forget internal suppliers: As a rule, sterile processing departments present many opportunities to improve responsiveness. If every instrument and set could be turned over reliably within hours, how many fewer instrument sets would need to be stored?
Simplify the equation. Often, the tendency is to overcomplicate things, to overanticipate and try to plan for scenarios that rarely arise, making system changes based on single incidents (i.e., a physician’s making a one-off request for a single, rare instrument for a particularly unusual surgery). Delayed customization is one simplification technique. Rather than pre-customizing, aim to keep things as vanilla and separate as long as possible, and customize at the latest reasonable moment to keep the possibilities high while keeping the materials management problem minimal.
Most hospitals have put effort into rationalizing vendors of similar products and reducing the number of similar units (gloves of every type and size are a simple but common example). But more can be done. If point-of-use materials were managed better, how much simpler could pick lists be? How much less rework would be needed (fewer items picked and put away, fewer kits assembled and then disassembled)? How much easier would it be to change rooms or shift schedules if better real-time customization were enacted?
Teamwork required
The opportunity to dramatically reduce both short- and long-term costs is great. Better designed and operating materials management systems are a key substructure of an efficient health care organization.
It seems simple, but it is surprisingly difficult to make actionable. To succeed, planners need to get help. They must recognize that different people bring different levels of expertise. Having experts develop a design in isolation is faster and easier, but often leads to unforeseen problems.
The best designs are achieved by diverse teams with diverse expertise, including the people who do the work, manage the work, support the work, supply or depend on the work, know the rules and regulations, and the people who know how to make complex systems work together.
When systems are well-designed and -maintained, it’s shocking how much is possible with the space and staff that already exist.
Lewis Lefteroff, MSIE, is managing member at Opus Solutions LLC.




