Building better behavioral health care facilities

View "Letting the light in" gallery
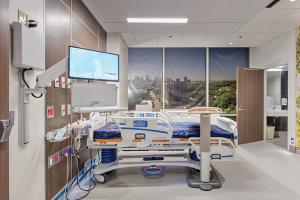
The psychiatric medical unit at Mercy Health Saint Mary’s, Grand Rapids, Mich., is serene and welcoming. Daylight fills the open floor plan, which is warmed by natural wood tones, and a large aquarium brightens one wall. “There’s a lot of natural light, a lot of room to move about,” says Carrie Mull, the unit’s clinical services manager.
It’s a marked difference from the previous location, which she describes as having been dark, institutional and crowded.
You may also like |
| Behavioral health design regulations |
| Interior spaces for behavioral health |
| Rise in behavioral health care facilities |
| |
The new 28-bed unit was created by renovating a traditional racetrack design to fit the physical space with the hospital’s model of care. Mull says, “You have to have the unit design integrated with the unit culture. I’m pretty passionate about saying that you can’t have one without the other.” Prior to the new design, she says the hospital’s care team saw some improvement in patients after establishing a collaborative, non-paternalistic approach to treatment. “But then when we combined it with the unit design, that’s when we really saw the outcomes soar,” she says.
Opening the layout
The new design at Mercy Health Saint Mary’s cuts through the existing unit from east to west to open up the layout, bringing in sunlight and creating a variety of open common spaces, says James M. Hunt, AIA, co-founder, Behavioral Healthcare Architecture Group, a specialty firm with offices in New York and Topeka, Kan. Hunt served as a consultant on the project for lead architecture, engineering and interior design firm Progressive AE, Grand Rapids.
Hunt explains that behavioral health patients generally are encouraged to spend time out of their rooms, participating in activities with other patients. “So the whole layout and flow and use of space is entirely different” from general acute care, where most activity takes place in the patient room, he says.
The open plan at Mercy Health Saint Mary’s keeps staff and patients visible to one another. Instead of a central nurse station, there are built-in benches throughout the unit where nurses can chart using workstations on wheels. “There’s never a time a patient can’t find a nurse,” Mull says. This reduces anxiety on the unit and the risk of patient falls.
Like any health care project, safety was paramount in the design and material selection. The aquarium, for example, is housed behind a protective layer of polycarbonate. The unit as a whole is meant to help people feel comfortable and amenable to treatment. According to Mull, patients experience less frustration in an environment that honors their humanity. “If you design a unit that’s respectful to them, you have a reduction in aggressive behavior,” she says.
Creating mindful space
Safety and comfort are two main goals of any behavioral health care design project. Hunt says, “We’ve learned over time that those two don’t have to be an either/or situation. We can provide both within the same environment, but it takes a different way of looking at it than what’s been typically done in medical institutions.”
Hunt also consulted on the design of the new Cherry Hospital, a state-run psychiatric facility in Goldsboro, N.C. The project’s architect of record, the Freelon Group, Research Triangle Park, N.C., is now part of architecture and design firm Perkins+Will. North Carolina Department of Health & Human Services spokesperson Olivia James says patient and staff safety was considered in all design decisions at Cherry Hospital — including materials, furnishings, circulation routes and use of space. For example, anti-ligature door hinges, handles and locking mechanisms are installed in all patient areas to prevent self-harm. “Many of these anti-ligature devices were not on the market until just a couple of years ago, and they were produced in response to the need by psychiatric hospitals,” James says.
These products confer a high level of safety without an institutional appearance, says Hunt. “It’s the direction all health care needs to go,” he adds.
Cherry Hospital’s main off-unit activity zone is organized as a therapy mall with classrooms, courtyards, a library, medical clinic and laboratory, gymnasium, group therapy and dining space. Located on the second level, the therapy mall is just one floor away, by elevator or stairs, from the rest of the building. James says that this is an improvement over the hospital’s previous campus, where staff members routinely had to transport patients between buildings. “This one up/one down concept allows a much safer transition of patients to and from the mall activities,” she says.
Common design elements throughout the facility include high ceilings, vandal-resistant light fixtures, durable finishes and furnishings, and natural light. “Natural light is a key design element,” James says. “All areas have utilized natural light to open spaces and make them less confining.”
Transparency and light also are key to the design of the Comprehensive Behavioral Health Center at Kingsbrook Jewish Medical Center, New York City, designed by the Behavioral Healthcare Architecture Group. At this facility, interior glazing to the corridor gives rooms a feeling of openness, making them more comfortable spaces to inhabit, says William N. Bernstein, AIA, LEED AP, co-founder, Behavioral Healthcare Architecture Group. Hunt notes that largely in response to recent hurricanes, the glass industry has developed products that are high-strength and perfectly clear, well-suited to use in behavioral health care. “There’s a lot of effort to create a safe environment and create a really appealing environment at the same time,” Bernstein says.
Solid, secured, natural-wood furnishings add to the appeal of patient rooms at Kingsbrook. Built-in benches provide a spot for patients to sit and read, or for counselors to sit, rather than on the bed, when seeing patients in their rooms.

View "Letting the light in" gallery
Design with dignity
Skyland Trail, a mental health treatment organization offering residential and day treatment programs in Atlanta, opened a new clinic in March to provide expanded primary care and wellness services to people with mental health diagnoses. “We’re providing a medical home for that population, with respectful care and clinicians who understand the interaction of physical and mental health issues,” says Beth Finnerty, president and CEO, Skyland Trail. “It’s a beautiful facility,” she adds.
The clinic has four exam rooms, a phlebotomy room, laboratory, pharmacy and infirmary. It features mocha-colored concrete floors in the lobby and a blue, green and cream color scheme throughout that Louise Labus, ASID, senior associate of Collins Cooper Carusi Architects Inc., Atlanta, describes as “calming, natural, clean and classic.” Accent material made from reclaimed wood enhances the natural look and symbolizes the patient experience of recovery and renewal.
Skyland Trail recently broke ground on a young adult campus located up the hill from the organization’s main campus and clinic. Michael L. Collins, AIA, LEED AP, principal, Collins Cooper Carusi Architects, notes hilltop sites are where people traditionally have built their most valued and protected environments. The 32,000 sq. ft. campus for 18- to 25-year-old patients will comprise three connected buildings with an interior courtyard. The site plan includes a number of garden spaces designed for therapeutic activities, outdoor games, artistic expression or peaceful contemplation. Horticultural therapy, recreation and social engagement also are important parts of the Skyland Trail program.
The facility’s treatment spaces are planned to include floor-to-ceiling glass to provide a visual connection to the outdoors. Views will be somewhat protected and away from the courtyard, to minimize distraction. Group therapy rooms are designed similar to classrooms, but will be furnished with mid-size lounge chairs. These rooms also can be used for staff meetings while staff offices will be located across the hall.
The two-story, 32-bed residential wing will be linked to the treatment spaces by a glass-enclosed bridge. The bridge will be closed during the day to prevent patients from isolating themselves in their rooms, away from daily group activities. Metaphorically, it will represent the transition between patients’ home and work environments and their journey to recovery, Finnerty says. A variety of shared spaces in the residential wing, such as a family room, lounge and game room, are meant to encourage patients to socialize outside their private rooms near a strategically positioned nurse station. Casters allow furniture to be rearranged easily, so people can congregate as they choose.
Each patient room will feature a large window with a built-in window seat to give personal spaces a homey feel, explains Jeff Morrison, AIA, LEED AP, associate, Collins Cooper Carusi Architects. Windows in the patient rooms will extend low, so patients can view the landscape even while resting in bed.
Skyland Trail is consulting on the development of HopeWay Center, an adult residential and day treatment campus being designed by Perkins+Will’s North Carolina office. The center, which is scheduled to open next year, will have separate zones for residential, therapeutic, dining and administrative purposes. According to Bill Blue, board chair of the HopeWay Foundation, the project team wants to bring together practical and aspirational concerns to present a warm, welcoming, nurturing, safe environment.
“Walk into lots of behavioral health facilities in this country and you’ll immediately realize what’s missing. What’s missing is good design. Because for a long time it wasn’t prioritized, and it’s pretty clear from the facilities,” says project architect Kevin Turner, AIA, LEED AP, principal, Perkins+Will. “Until we start building buildings that look like we as a society treat people with mental illness in a way that is dignified, then people will want to avoid treatment. We’ve got to send the message that you can receive treatment and you can do it with dignity.”
Continuum of care
Rebecca Kleinbaum Sanders, AIA, NCARB, health care principal in the Minneapolis office of architecture, engineering and planning firm HGA, remarks that there is a continuum of care in behavioral health, just as in general health care. Patients may require an emergency department or crisis center, acute care, residential care or a day treatment center, depending on their needs. “It’s important to think of all the different settings,” says Kleinbaum Sanders. Different settings entail different treatment environments and levels of patient observation.
Hazelden Plymouth (Minn.), is an addiction treatment center operated by the Hazelden Betty Ford Foundation. The center provides a variety of residential and outpatient services for patients age 12 to 25, as well as family programs. In the entrance lobby, regional limestone and cherry wood give a sense of stability and warmth. The treatment spaces include art and music therapy rooms and a gymnasium with a climbing wall, all intended to keep patients engaged and actively learning to interact with others. The residential area has a living room, quiet lounge and snack area for group activities. Individual sleeping areas are separated by half-height walls.
Hope House, Martinez, Calif., a 16-bed, short-term residential treatment facility operated by mental health service provider Telecare Corp., is meant to serve as an alternative to inpatient hospitalization in times of crisis or as a step-down, transitional living environment. According to Kleinbaum Sanders, the facility is designed to give people room to grow and develop toward integrating into the community. The facility has single and double bedrooms. Areas like the group kitchen give people a place to learn and practice life skills.
The ultimate goal
Hunt stresses that while the patient-caregiver relationship is the most important aspect of recovery, design can play a significant role.
“A building’s not going to heal anybody,” he says. “But you can put patients in a space that makes them worse. You can take a patient who is suffering from depression and put them in a facility that makes them feel like they’re being punished for being ill. And if we give them an environment that makes them feel that way when they come in, we’re going to deepen that depression. We’ll make them more difficult to treat.”
The ultimate goal in the design of behavioral health facilities is to make patients feel at ease, comfortable and receptive to treatment. “If we can accomplish that, I think we’ve done our job very well,” Hunt says.
Amy Eagle is a freelance writer based in Homewood, Ill., who specializes in health care-related topics. She is a regular contributor to Health Facilities Management.