Improving operating room cleaning efficiency
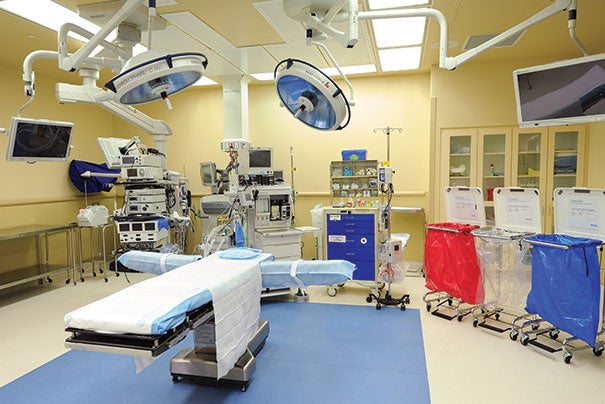 |
| Photo courtesy of Ecolab Responsibility for cleaning the OR for the next patient varies by hospital. |
Patient safety and prevention of health care-associated infections have always been and will continue to be driving forces in the health care environment. Surgical services departments are increasingly challenged to ensure patient safety while improving operational efficiency and maintaining cost-effectiveness for patients undergoing operative or other invasive procedures.
You may also like |
| 2015 ES Department of the Year |
| Budgeting advice for ES professionals |
| Technologies to improve hospital cleaning |
| |
For health care facilities, time is money — and that is especially true in the operating room (OR). ORs often feel a lot of pressure for quick turnover times to help increase the number of surgeries they execute per day.
There are several important steps in preparing an OR for the next patient. These include but are not limited to removing the case cart, bagging trash and linen, cleaning and setting up anesthesia equipment, cleaning and disinfecting high-touch objects, mopping the floor, making the bed, opening for the next case, interviewing the patient, preparing medications for the next patient, and counting and prepping.
Taking a Lean approach to this challenge can improve both the speed and the thoroughness of an environmental services (ES) staff.
Hospital to hospital
Responsibility for cleaning the OR varies from hospital to hospital. As part of a project to learn who cleans the operating room, 250 hospital OR directors across the country were surveyed by Ecolab, a St. Paul, Minn.-based health care vendor.
The results of the study showed that 62 percent of room turnovers are completed by the OR staff, 19 percent are completed by a combination of the OR and ES staffs, and 19 percent are cleaned by the ES staff alone.
Many hospitals have a goal of 20 minutes to turn a room over from wheels out to wheels in. The cleaning and disinfecting portion of room turnover is a priority, but there are many additional factors that can affect room turnover time. The goal for hospital staff is to control as many factors as possible.
Processes that must be put into place by the OR staff and managers to ensure a clean and safe room for the next patient include:
• Cleaning teams available immediately post-surgery;
• Efficient and effective room turnover and cleaning supplies available;
• Training on best practices for cleaning and disinfecting an OR;
• Monitoring the thoroughness of cleaning and providing feedback to drive continuous improvement;
• Defining roles and responsibilities clearly.
In addition, hospital management teams incorporate evidence-based guidelines and recommended practices into perioperative standard operating procedures in an effort to ensure that best practices are followed. Surgical services departments also are incorporating Lean and other process improvement methodologies to identify and eliminate waste and inefficiency in the perioperative area.
To optimize operating room cleanliness and efficiency, two organizations partnered on a Lean OR throughput project in a two-phased implementation process.
Lean OR throughput
Crestwood Medical Center, Huntsville, Ala., has 19 ORs and averages 1,100 surgeries per month. As part of a larger Lean program that looked at the entire perioperative process from registration to discharge from the post-anesthesia care unit (PACU), Crestwood was interested in optimizing between-case cleaning and room turnover efficiency in the OR, with a secondary emphasis on terminal cleaning. With its already-developed program to address these important issues, an OR throughput and cleanliness study was conducted by the hospital and Ecolab.
To do this, leaders formed a multidisciplinary team that included OR and ES staff, hospital leadership, a corporate clinical expert, a Lean Black Belt team and two subject matter experts from the vendor.
A value-stream analysis was completed to outline the steps, time and value of each step in the process. The team then did a rapid improvement event where members implemented the new process. Once the process was implemented, the results were measured to see if the objectives had been met.
Processes observed included room turn time, cleaning method, linen use, equipment storage and use, the application, contact time and material compatibility of the current disinfectant, and current roles and responsibilities related to cleaning the OR.
Baseline thoroughness of cleaning high-touch objects (HTOs) was measured, and between-case turnover time and motion studies were conducted. The teams collected pre- and post-implementation data to determine the impact on room turnover time, thoroughness of cleaning and asset costs.
After the initial observation of cleaning staff, Crestwood and the vendor saw a few key areas for improvement, including:
• Cleaning consistency. HTOs like procedure lights and OR table controls were not cleaned consistently between cases.
• Equipment location. Environmental hygiene equipment and linens were not located conveniently for staff.
• Cleanliness recognition. Staff could not tell when a room had been cleaned.
• Disinfectant contact time and equipment damage. The hospital’s bleach disinfectant needed a 10-minute contact time, requiring the replacement of as many as two OR mattresses every three months because of damage.
Key initiatives
After collecting the initial findings, experts identified key initiatives for process improvements. These initiatives were introduced to staff in two phases.
Phase 1 introduced the vendor’s products, tools and training to improve cleaning outcomes. The program provides:
• An OR environmental hygiene program that focuses on HTO cleaning and uses fluorescent marking gel to objectively measure the thoroughness of disinfection cleaning on critical surfaces. The cleaning outcome data and observational information is captured on a handheld device and wirelessly transmitted to a secure database from which real-time data and customized reports can be generated. The reports help to drive continuous improvement and provide compliance to current guidelines and industry recommendations.
• Training on cleaning practices. Staff members participated in hands-on training on environmental hygiene best practices that was developed by the vendor and awarded recognition by a nurse organization.
• Cleaning kits that improve OR turnover time and that include absorbent linens, armboard covers, pillowcases and headrest covers, bags and disposable microfiber wipes and mops. Microfiber technology reduces water and chemical usage while effectively cleaning and disinfecting surfaces. It also reduces lint in the OR.
• A cleaning station that provides access to cleaning products and tools at the point of use and is designed to prevent cross-contamination. Tools such as a squeegee-style sweep set are designed to improve cleaning efficiency and minimize the risk of cross-contamination.
• A one-step disinfectant cleaner designed for general hospital cleaning, disinfecting and deodorizing of hard, nonporous inanimate surfaces. With a five-minute contact time for Clostridium difficile spores, it helps to improve room turnover time while providing favorable material compatibility.
Staff members spent one month familiarizing themselves with the new products, tools and cleaning procedures before implementing Phase 2, which included a Lean rapid-improvement event (see sidebar, this page) focusing on clearly communicated roles and responsibilities for the room turnover process.
Data were collected before implementation — immediately following the rapid-improvement event and then again six months later. After execution of Phase 1 and Phase 2 initiatives, Crestwood saw many positive outcomes, including:
• A threefold improvement in thoroughness of cleaning HTOs, for both between-case and terminal cleaning;
• A five-minute disinfectant contact time;
• Room turnover time decreased by five minutes from wheels out to room ready for next case;
• Clear roles and responsibilities were defined that helped to eliminate rework and omission;
• Turnover packs left on the OR table became the visual cue that the room was clean;
• A “Lean board” was created to communicate results to staff.
Six months after training, the room turnover time continued to be five minutes faster than it was prior to the OR throughput project and thoroughness of HTO cleaning remained higher than 80 percent for terminal and 90 percent for the time between cases. This confirmed that the process was not only improved temporarily, but that the improvement was sustained over time.
Crestwood did not need to replace any costly OR mattresses in the six months following conversion to the daily disinfectant cleaner.
Implementing Lean
More hospitals are implementing Lean projects to create standard work and improve critical processes that affect patient outcomes.
The partnership among Crestwood leadership and staff, corporate clinical leadership, corporate Lean consultants and the vendor improved OR throughput and cleaning efficacy, provided performance feedback for continuous improvement and preserved valuable assets.
Most importantly, this collaborative project ensured that the ORs were thoroughly cleaned, which may help to prevent the transmission of pathogens that can cause surgical-site infections.
Linda Homan, R.N., BSN, CIC, is senior manager of clinical and professional services for Ecolab, St. Paul, Minn. She can be reached at Linda.Homan@ecolab.com.
Six tools to help apply Lean methods to hospital cleaning
Lean is a set of operating philosophies and methods that help to create maximum value for patients by reducing inefficiencies and waiting time. It emphasizes the consideration of the customer’s needs, employee involvement and continuous improvement.
The value of Lean is that it engages the creativity and skill of the staff who are doing the day-to-day work and promotes collaboration across the work stream. There are six tools commonly used in health care cleaning to reduce inefficiencies and improve processes:
• Value stream maps to define what delivers the most value to the patient;
• 5S (sort, set in order, shine, standardize and sustain) to help create a safe and organized work space;
• Process maps to identify waste in a process;
• Standard work to standardize processes to deliver consistently and reduce complexity;
• Root-cause analysis and problem-solving tools;
• Visual management (visual reminders of performance, such as daily huddle boards and surgery flow boards).
A popular approach to continuous improvement is the rapid-improvement event (RIE). An RIE is a 3- to 5-day event that brings together a multidisciplinary team with the objective of improving a specific process. The goals of an RIE are to identify improvement opportunities, develop solutions and implement them quickly. The steps include: Define the improvement, collect the data, analyze the data, implement improvements to deliver the desired outcomes, and implement controls to make sure the outcomes are sustained.
The success of Lean is not in the number of tools used or the number RIEs sponsored. Lean requires engagement, collaboration and a commitment to continuously improve patient safety and satisfaction, treatment outcomes and staff development.


