Conducting facilities assessments
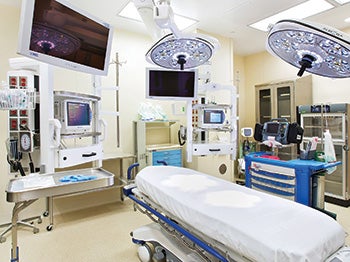 |
| Surgical suite updates can present significant operational ramifications. Photo © Kevin Chu/KCJP |
Health care delivery in the United States is undergoing substantial changes as health systems across the country now begin to feel the full impact of the Affordable Care Act. Health systems are merging and partnering at all levels, which requires combining, updating and repurposing existing facilities as well as creating new ones.
In this environment, successful health systems face an increasing need to plan accurately for future capital expenditures. It's imperative that they prioritize bottom-line efficiency to capture and control market share in their demographic and deliver world-class affordable and accountable care. With multiple requests for investments, some more urgent than others, it's crucial that administrators choose where to invest based on accurate data and thorough analysis.
A facility assessment delivers this data and analysis, helping administrators invest their capital strategically today and craft an effective plan for projected expenditures over the next decade.
In-depth evaluation
A facilities assessment is a process in which a health system retains a team of experts to survey and evaluate its real estate on the basis of condition, investment needs, viability for reconfiguration and other factors. Assessments can focus on a single building or an entire system of buildings. In-depth assessments address space utilization, occupation factors and business growth models.
Modern and well-maintained health care facilities are important for safe and efficient patient care. Health systems must position their facilities as pre-eminent, cutting-edge institutions at the forefront of emerging technologies in every sector — from radiology to interior finishes to patient room comfort. Managing all of these priorities while staying within a predetermined capital budget and preserving existing revenue streams is an ongoing challenge.
Facilities assessments also help administrators decide which buildings should be updated, and which should be demolished and replaced. If an old building requires constant maintenance and renovation, replacing it may be more cost-effective than maintaining it over the long term. In many instances, buildings have reached their effective service life. This may be a result of aged or outdated infrastructure, an inability to reconfigure the space in a cost-effective manner, floor-to-floor heights that make serving the spaces too expensive, a column grid layout that is not conducive to an efficient floor plan layout, or simply too many prior reconfigurations. Not all buildings are suitable for reconfiguration without considerable capital investments and many times it does not make economic sense to renovate.
When hospitals merge or acquire new systems, they take ownership of new buildings and real estate — both major acute care centers and the outlying outpatient network. These facilities are often aging, poorly maintained, inefficient or visually dated. When real estate holdings increase, acquiring systems may not know what condition the new properties are in.
As a system grows or contracts, capital budgets change. Systems need continuous investments across the board. A capital budget must cover new equipment, updated infrastructure, changing clinical delivery models, aesthetic upgrades for patient satisfaction and compliance with new codes, among other items. The results of the facilities assessment will prioritize a system's strategic investments, helping administrators to use the resources at their disposal for maximum impact.
Navigating the process
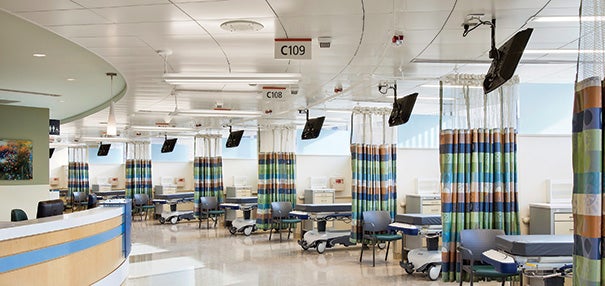 |
| Selective infrastructure upgrades should be scheduled to reduce clinical flow impacts. Photo © Chris Cooper |
The first step in a successful facilities assessment is to quantify the effort and the outcome. Health system administrators must define the objectives, focus and the targeted final outcome.
This process then proceeds with the selection of a qualified assessment team. Administrative champions make up a key component of this team. They shepherd the process, facilitate access to the facilities and explain the process to individual building administrators. These team members act as conduits to senior leadership, keeping them informed of progress, milestones, challenges and results.
The rest of the team should consist of qualified professionals to undertake the work, including architects, engineers, program managers and cost estimators. The architect should lead the team and serve as a primary point of contact. Preferably, these professionals should be known to the health system and already have worked on the facilities that will be studied. This promotes efficiency, saving the time and cost of familiarization. It also allows the team a running start because they may be aware of pre-existing conditions. A collaborative process is key to the successful delivery of an assessment because multiple professionals will have multiple places of focus.
Once the team is assembled, members define the deliverable and the work process. They ask and answer questions that help them determine which facilities should be assessed, what major challenges must be overcome, and how deep the study must go. Each system calls for a different level of survey. Older buildings may need extensive review, while newer ones may need only code comparisons. The team defines the parameters of the assessment according to the following criteria:
- Size and age of the facility;
- The age and condition of expansions and additions;
- The physical condition, including the condition of structural, mechanical and electrical systems;
- Systems serving information technology, nurse communication, emergency notification and similar functions;
- Level of code or guideline compliance;
- Facility functionality, such as department adjacencies;
- Facility energy-efficiency and infrastructure conditions;
- Overall aesthetics of the facility;
- Site parameters, expandability and parking capabilities.
Once these parameters have been established, the team should agree on the level of detail required to record the conditions. A simple rating system on a scale of one to five can be helpful. This can be used to evaluate and document the aesthetic appearance of a facility, the conditions of internal finishes, and the condition of infrastructure, air handlers, electrical systems and all of the components being assessed. This rating system establishes priorities and makes it simple to understand a critical need vs. a deferred maintenance issue.
Moreover, assigning a color to each numerical rating easily communicates needs — with green as the best condition and red as critical. This color system then can be carried throughout the final reports, including all the assessment sheets, floor plans and even the executive synopsis.
After completing the recording parameters, the team establishes a timeline for completing milestones such as the physical survey, draft findings, date of delivery to the cost estimators and final presentation to senior leadership. The project manager is responsible for maintaining open and collaborative lines of communication and ensuring that the assessment remains on track from inception to completion.
The team then visits, surveys and documents every single space. Using iPads can help to document the findings, make notes in real time on the plans provided, update spreadsheets and record changes or inconsistencies with the documentation before the survey. This may include previous floor plan changes or air-handler replacements completed by the facility at the local level. Using advanced technology facilitates a streamlined and accurate recording system that can be shared by all team members.
The engineering teams associated with the specific buildings should undertake a similar survey. Their task is to assess the existing building systems, their life expectancies, how critical the system is to the immediate function of the building, and whether the system is the appropriate and efficient solution to the space.
Hospitals and medically related facilities are estimated to consume 11 percent of all power generated in the United States, so their systems and equipment need to be highly efficient to be cost-effective. Upgrades to equipment like refrigerators and magnetic resonance imaging machines have been known to yield an 18 to 29 percent reduction in electrical consumption. Likewise, mechanical, electrical and plumbing systems must operate efficiently.
Once all the spaces have been assessed, the compilation of data begins. The team creates individual sheets for each room or space, noting deficiencies, aesthetics or code items. Here, again, color coding of the plans for each department is helpful.
The complete data set then is delivered to the cost estimators, who evaluate the capital expenditures required for the recommended changes. The construction manager assigns costs to each element of the assessment and assists the team in determining year-over-year project cost escalation. In addition, this allows health system administrators to project capital cost expenditures over several years and create a projected investment schedule to fit their budgets.
As they decide what updates to prioritize, administrators also should consider the impact a project will have on a functioning unit or facility. For example, if a new surgical pavilion can be completed without interruption to the existing surgical suite, no revenue will be lost. While renovating the same suite may cost less, it also may take operating rooms out of service, resulting in lost revenue.
In some instances, though, a system's immediate needs outweigh the long-term outlook. In this Band-Aid approach, the system then will require a short-term investment, knowing that these costs cannot be reclaimed in the future. For example, one cancer center installed trailers that remained on-site for more than three years so that patient care could continue during the demolition of current facilities and construction of new facilities. With rapid changes in technology, especially the growing efficiencies in mechanical and electrical systems, current systems investments must be weighed carefully against the future, but often waiting is not an option.
Results and reports
When a facilities assessment is finished, the team presents hospital administrators with a book that contains an executive summary of findings, including colored floor plans and spreadsheets showing the data gathered by the team. Ideally, administrators can easily reconfigure the spreadsheets to show campus allocations, building allocations, health system priority allocations or service line costs, such as total investment proposed for acute care facilities. Each budget also should contain hard and soft costs, capital costs, equipment and infrastructure and, again, escalation costs.
These detailed facilities assessment reports enable the health system to determine the best allocation of their resources by distinguishing between needs and wants. The data contained within the reports will tell them if it makes more long-term financial sense to build or replace an existing building than to continue to invest in capital project upgrades.
One key to publishing a successful report is to make sure it appeals to a broad group of recipients. If the report can be understood only by one group of professionals, it will be relegated to a backroom shelf. The challenge is that not all hospital administrators think alike. If the document, or its synopsis, reads like an engineering report, only the facilities folks will use it. If it is full of complex strategies for phased projects like a master plan, only administrators will be drawn to it. To succeed, the report must strike a balance.
A recently produced 300-page project report opened with a first-page overview that instantly told administration which of its six facilities needed to be replaced. The page used a graphical, colored chart, with a red triangle representing worst cases and a green circle indicating those in good condition. Readers who needed more detail in support of the recommendations could flip to the appropriate section. Color coding and photography also were used.
Using the data contained in the reports, health system administrators can strategically plan for maintenance and growth, projecting expenditures for the next five to 10 years. With data from the reports, administrators can decide whether to replace current buildings before systems fail or to invest in newer and more efficient facilities.
Smart investment
Committing the resources to a facilities assessment is a smart investment in the future of a health system. The findings of the assessment report can act to spotlight deficiencies that need to be addressed immediately, sometimes before other clinical investments can be made.
Aran A. McCarthy, AIA, NCARB, is a principal for health care in the Philadelphia and New York City offices of Francis Cauffman. His email is amccarthy@franciscauffman.com.
Achieving efficiencies of scale
A health facilities assessment gives hospital administrators a clear understanding of the state of their spaces and the ability to group potential projects together. This can improve financial efficiency in the following ways:
• Coordinating projects. Traditionally, after identifying the need for a renovation or additional space, a health system searches for the best location without always considering the optimal infrastructure. Engineering upgrade projects can run parallel to aesthetic upgrades or more extensive renovations, and sometimes funds are wasted because renovations are not coordinated. For example, when an aesthetic upgrade project requires removal and replacement of a ceiling, it makes sense to install a sprinkler system at the same time. If the ceiling replacement is completed first and a sprinkler system is required later, a facility may need to destroy a good ceiling to install the piping.
• Determining suitability of space. If an institution is considering multiple investments in the same location, the facilities assessment will inform decisions about whether these investments are valuable. Why invest in a cosmetic upgrade of a space if the mechanical systems servicing the area won't be able to support it? The facilities assessment gives administrators the foresight to understand not only what can be seen, but what is behind the scenes. This leads to better decisions and more strategic investments.
• Increasing purchasing power. The assessment also gives administrators the ability to package projects of a certain type to reduce overall project costs. Whether they're aesthetic upgrades or air-handler replacements, the health system gains greater purchasing power based on size and scope if they are undertaken together. In an industry that is currently experiencing unprecedented collaboration and merger activity to increase purchasing power in the marketplace, taking the same approach to capital expenditures makes sense.




