FGI Guidelines help to redefine imaging spaces
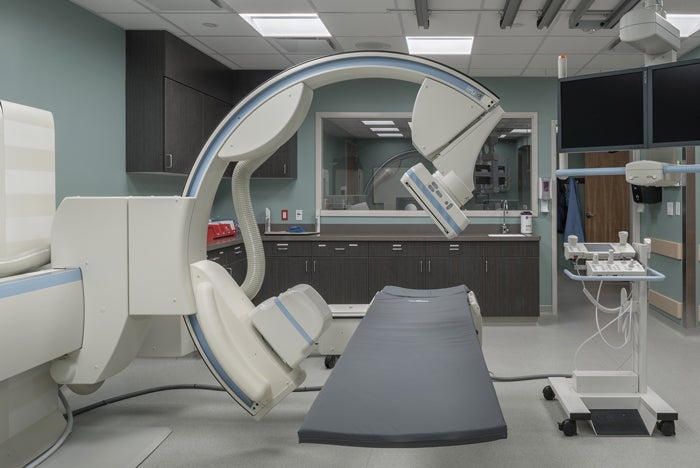
Supporting role: C-arms frequently support image-guided interventions or procedures, and would typically be designated as Class 2.
Image © RAD-Planning, used with permission
Although Shakespeare’s line “a rose by any other name would smell as sweet” posits that the name given a thing doesn’t change what it is; a corollary is that names do matter as they become the representation of a thing in the describing and retelling.
At the heart of the new classification system for imaging services in the 2018 edition of the Facility Guidelines Institute’s (FGI’s) Guidelines for Design and Construction for hospital and outpatient facilities is an appreciation for the power of a name.
Understanding this new convention is key to enabling health facility planners and designers to seamlessly implement requirements in their imaging unit designs based on the classification system.
Imaging in transition
In the past, imaging design standards focused on the radiology device (modality) to be installed rather than the type of care the device would support or the setting in which it would be placed. As long as one could call radiology “diagnostic (only),” questions of setting didn’t really matter much. For a long time, a doctor’s office X-ray patient wasn’t substantially different from a hospital X-ray patient. When this was the case, it made sense to base the planning and design of imaging facilities on the technical criteria of the device and not the setting or the patient.
Today, however, the breadth of patient acuity and intervention supported by imaging services makes the prior approach outdated. No more are computed tomography (CT) suites universal, whether located in a physician practice or an outpatient imaging center or serving an emergency department (ED)/trauma unit. Imaging still frequently serves “walkie-talkie” patients (i.e., those who come in and leave under their own power), but the range of acuities served by imaging now includes patients with altered mental status, emergent patients, critical/intensive care unit patients, post-surgical patients and those undergoing general anesthesia.
In addition to broadening patient acuities, clinicians are doing more to patients during imaging than in decades past, such as image-guided biopsies (e.g., ultrasound-guided biopsy) and image-guided therapies (e.g., magnetic resonance (MR)-guided focused ultrasound). Some of these activities fall squarely within the definitions that hospitals would use to characterize “procedures” instead of “exams.”
This burgeoning use of diagnostic imaging services as a platform for intervention is occurring simultaneously with the expansion of what one might think of as typical interventional imaging, whether in cardiology, vascular surgery, neurology, pain management or other specialties. What was once a relatively clear boundary separating diagnostic imaging from intervention is now blurred.
Just as the patient acuity and intervention levels seen in diagnostic imaging are being pushed up, interventional proceduralists and surgeons who previously operated without imaging increasingly want the real-time information that imaging resources provide. The boundary conditions that had distinguished “diagnostic imaging” from “interventional radiology” from “surgery” have been muddied from all sides. While popular naming conventions may still describe a “diagnostic imaging” department, those names suggest a limitation that no longer exists in practice.
When this patient acuity and intervention scope creep collides with historic naming conventions, one may fail to recognize just how significantly the underlying conditions have changed. How many planners and designers think of radiology services as interventional platforms? How quick are owners, designers and planners to dismiss the MR-guided breast biopsy as a one-off special case?
When one-off exams occur monthly, though, they’re no longer one-offs. When organizations want to use imaging resources to support the care of higher-acuity patients or the delivery of procedures, the care of the patient must supersede the technical requirements of the imaging hardware in the design of the imaging facilities.
Keeping pace with changes
The 2018 FGI Guidelines documents have implemented a classification scheme for hospitals and outpatient facilities to correlate the planning and design of imaging suites with the level of support needed by the patient. This new system identifies three distinct levels — Class 1, Class 2 and Class 3 — which mirror existing distinctions among examination or treatment rooms, procedure rooms and operating rooms, respectively. While the nomenclature for imaging services may be new, it builds on existing room-use distinctions that have been applied broadly throughout the health care community.
FGI’s imaging classification system differentiates imaging services based on three criteria: patient acuity, level of invasiveness and use of anesthesia. The highest patient condition in each of these categories defines the class level to which a room should be designed and built. For example:
- If a room truly serves as a diagnostic imaging facility, where the greatest level of intervention is the use of IV contrast, then the room would be appropriately designated Class 1.
- If the room is intended to support image-guided biopsies, imaging for patients who need clinical monitoring or percutaneous/minimally invasive procedures conducted under image guidance, the room should be designated Class 2.
- If the room is intended to serve an image-guided, open surgical procedure, then it needs to be designated Class 3.
This new class system demands more of planners and designers than the prior approach to designing imaging facilities. To answer questions about the classification of imaging modalities, it is now necessary to have a number of programming and clinical-use questions resolved in advance. Will this imaging resource be used for patients who require clinical monitoring? Life support? Will it support intervention or therapy that would make it a procedure room (Class 2)?
To correctly determine the appropriate classifications for imaging rooms, input from clinicians is essential early in the planning phase. This includes those who oversee imaging services as well as referring physicians who expect to use the facility’s imaging tools for their patients and allied clinicians (e.g., anesthesia, respiratory or cardiology professionals) who may have patient care responsibilities during imaging.
These questions may uncover ambiguous classification conditions, such as transcatheter aortic-valve replacement, which may appear to live in the gray boundaries between classes. When discovered, such ambiguous conditions should prompt a health care organization to conduct a risk assessment to determine how it wishes to manage the risks and which class of room is appropriate for a particular procedure.
Because of the cost and complexity of imaging spaces, not to mention their essential role in clinical care, upgrading an imaging facility (from Class 1 to Class 2, or Class 2 to Class 3) post-occupancy may be both prohibitively expensive and disruptive. For these reasons, it is advisable to spend some time in the planning process anticipating likely future upgrades to the clinical use of a room. Doing so will help ensure that the facility’s imaging rooms will meet the needs of potential future uses or, at the very least, can be cost-effectively modified to meet the higher demands of an upgraded clinical use.
While the intent of the FGI classification system is to provide a consistent structure to the planning of imaging suites, it is recognized that anesthesia, in particular, has different uses with patients of different risk profiles. If the level of intervention is such that a patient couldn’t tolerate the pain associated with an exam without anesthesia, then the space should be built to a minimum of Class 2.
If, however, the anesthesia is provided to an otherwise healthy patient to overcome anxiety, it is the intention of the 2018 Guidelines that a Class 1 room, with the medical gases and emergency power indicated for Class 2, could be appropriate to the task. The other Class 2 requirements, such as those for infection control, HVAC, system component room access and others, would not be required for a Class 1 room supporting anesthesia for patient anxiety alone.
Achieving compliance
So, how should these new classification standards be manifested in a set of documents? This will depend, in part, on what state or local officials require.
If the authority having jurisdiction (AHJ) requires programming statements, the clinical use for imaging rooms should be clearly identified in the program documents. Anticipated highest use for patient acuity, intervention and anesthesia should be indicated for each imaging room. Keep in mind that a submitted program document (and the limits defined therein) may determine the specific parameters for a building, use, accreditation or license.
In the design and construction documents, designers should clearly indicate the class designation for any imaging space. This extends from identifying the class on the floor plans to indicating classification on schedules for finishes, HVAC equipment and infection control plans, when applicable.
For AHJs who review documents under the new 2018 FGI standards, the change is similar. AHJs will be explicitly looking for the imaging class designations in the design and construction documents and checking for internal consistency in this labeling. A CT unit located adjacent to an ED, with a dedicated holding area for patients on gurneys, is unlikely to be operated as a Class 1 suite, even if it is labeled on the plans as such.
Make sure the clinical use and imaging classification are specified in the documentation and the design criteria are followed for the indicated clinical use and class of each imaging room. These criteria are clearly referenced in the imaging requirements of the 2018 hospital and outpatient Guidelines.
Keep in mind that clinical scope creep in an imaging space beyond a defined use may potentially violate AHJ criteria for approval of the design. In fact, the development of the imaging classification system was spurred, in large part, by the increasing patient acuity and interventions seen in imaging facilities and a desire to make sure that facilities and practices provide the appropriate supports.
An expansion in a space’s clinical use (e.g., from Class 1 to Class 2) should be seen as a change in use, invoking new design requirements even if the imaging device itself has not been replaced. This possibility emphasizes the importance of an early, clear understanding of the potential clinical use(s) of a space.
Forward-thinking design
In deference to Shakespeare, the name of a rose does not alter its fragrance. The designation of an imaging resource, however, does communicate a richness of meaning and expectation. In this case, the name matters significantly. An MRI is not an MRI, irrespective of where and how we use it. Devices are not universal in their clinical application, and the rooms in which we place them should not be understood to be modest site-adapted variants of cookie-cutter templates.
The 2018 Guidelines imaging classification system will help facility planners, designers and AHJs tailor hospitals and outpatient care centers to the specific needs of imaging services patients. Building on the existing differentiation of clinical services routinely used in health care facilities, FGI’s Class 1, Class 2 and Class 3 imaging room design criteria will help health care organizations respond to the remarkable, ongoing changes in clinical use of imaging services that have been seen over the last 20 years. Further, the new system will support the creation of facilities that have been appropriately designed for the delivery of modern medical diagnosis and treatment.
Tobias Gilk, MRSO, MRSE (MRSC™), is a design consultant with RAD-Planning, specialists in radiology design. He can be reached at TGilk@RAD-Planning.com.